Surgery STAT: Congenital portosystemic shunts
Congenital portosystemic shunts usually are single vessels that develop inside or outside the liver (Photo 1). Because these vessels carry blood around the liver instead of through it, the normal hepatic processes of metabolism, storage and production are disrupted.
Congenital portosystemic shunts usually are single vessels that develop inside or outside the liver (Photo 1). Because these vessels carry blood around the liver instead of through it, the normal hepatic processes of metabolism, storage and production are disrupted. Most animals with congenital portosystemic shunts (CPSS) present with mild to moderate clinical signs that are not life-threatening. The most critical component for their long-term treatment is restriction of dietary protein to reduce substrates for ammonia formation by colonic bacteria. Diets for dogs with CPSS should be 15 percent to 20 percent protein on a dry matter basis, readily digestible, high in zinc and vitamin E, and low in manganese. Sources of gastrointestinal hemorrhage (gastritis, parasites), which provide additional protein substrate, also should be treated. Ammonia production and absorption can be reduced by administration of lactulose, antibiotics such as neomycin or metronidazole, or unflavored yogurt with active cultures. Cystitis should be treated with appropriate antibiotics based on urine culture and sensitivity; infection may persist if uroliths are present.
Photo 1: Large portophrenic extrahepatic PSS (arrow) coursing along the lesser curvature of the stomach and the esophagus.
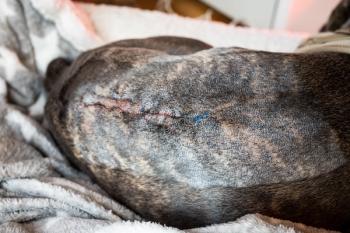
Occasionally animals with CPSS present with seizures. Because seizures may be secondary to hypoglycemia or encephalopathy, animals should be treated for both conditions (Photo 2). Owners can be instructed over the phone to rub a sugar source along their dog's gums while they are preparing to transport it to the clinic. If the animal is not seizing upon arrival, a catheter should be placed immediately and blood samples obtained before drug administration.
If the animal is actively seizing, IV boluses of diazepam (0.5-1 mg/kg) and 25 percent dextrose (2-15 mls) can be administered with a butterfly catheter before placing a more permanent intravenous line. Diazepam can also be administered rectally (1 mg/kg). Diazepam boluses can be repeated two to three times if gross motor activity does not subside, and also can be administered as a CRI (0.5-1 mg/kg/hr). Because diazepam is absorbed into the plastic, only one to two hours of CRI solution should be prepared at a time. Retention enemas of lactulose (5-25 mls) are administered to decrease toxin absorption and production. Animals that continue to seize with the above treatment may either have a different underlying pathology (i.e., epilepsy or hydrocephalus), or may have central neurologic damage from prolonged seizures. When brain damage occurs in animals with PSS, surgical correction of the PSS is unlikely to result in clinical improvement. Persistent seizures are treated with IV boluses of phenobarbital (2-5 mg/kg; repeated up to three times) and phenobarbital CRI (2-10 mg/h) or intravenous sodium bromide. If cerebral edema is suspected, glucocorticoids and mannitol are recommended. Animals with intermittent seizures may require maintenance oral antiepileptic drugs (phenobarbital or potassium bromide).
Photo 2: Because seizures may be secondary to hypoglycemia or encephalopathy, animals should be treated for both conditions.
With proper medical management, weight and quality of life stabilize or improve with treatment in most dogs. One third of dogs do well with medical management as the sole method of treatment, with many living to 7 years of age or older; dogs that are older at presentation or have a higher BUN live longer. Over half of dogs treated with medical management alone are euthanized, usually within 10 months of diagnosis, because of uncontrollable neurologic signs and, in some cases, progressive hepatic fibrosis and subsequent portal hypertension. Surgery is therefore considered to be the treatment of choice for dogs with congenital PSS. My personal experience is that most clinically affected cats that are medically managed for PSS live one to two years after diagnosis.
Dr. Tobias is an ACVS board-certified surgeon who specializes in small-animal soft-tissue surgery; her primary research interest is congenital portosystemic shunts in dogs. Dr. Tobias is full professor at the University of Tennessee and lives in Knoxville with her husband, two children, and a multitude of unmanageable pets.