Puncture wounds of the equine sole
Puncture wounds of the sole in horses can range from simple to complex-even life-threatening-depending on the area of penetration.
Puncture wounds of the sole in horses can range from simple to complex—even life-threatening—depending on the area of penetration.
All foreign objects (e.g., nails, screws, glass, wooden objects) that manage to gain entrance to the internal structures through the sole of the foot have one thing in common—they carry debris and bacteria with them. Regardless of the injury's location, consider all sole punctures medical emergencies.
When encountering a patient with a puncture wound, I always ask the client, "Did you pull the object out?" Usually the answer is yes. But I prefer to hear, "No, I left it in and placed blocks around it, so you could see it and radiograph it first." Ah, but that's unlikely.
My second question is, "Did you save the object?" Usually the client has.
Another question of vast importance: "When did you pull the object out?" If it was removed several days ago, my job just got a lot harder, as we now have an anaerobic Petri dish brewing somewhere in the foot.
It's important to have the penetrating object in hand so you can judge its length and width. If it's a metal object, determine how corroded it is. In the case of many types of porous objects, the piece may appear broken (i.e., you'll be searching for fragments). Sometimes nails, screws or other metal objects are bent, which indicates forceful puncture of the foot. Or the object may have been bent before entry, which would indicate you need to look for a puncture that doesn't follow a straight route into the foot.
Investigate further
After you've gathered as many clues as possible about your penetrating object, sedate the horse and perform the following:
1. Proceed with an apical or posterior digital nerve block of the foot, depending on the location of the puncture.
2. Aseptically prepare the foot, find the entry hole and place a probe within the sole.
3. Obtain lateral, dorsopalmar and oblique radiographs of the foot.
4. Use curettes to open the wound all the way to its most distal extreme in an aseptic manner.
5. Take a sterile swab for culture and cytology.
Once opened and explored, puncture wounds should be packed with antibiotic-soaked gauze (amikacin is most commonly used) or diluted povidone-iodine and gauze. The greater the hole's diameter, the more pressure should be applied to the packing. Aseptically bandage the foot as soon as possible, and then affix a shoe with a water-tight hospital plate to the foot (Photo 1).
Photo 1: A typical hospital plate in place.
Review the anatomical location of the sensitive structures below the equine sole. This will help you with diagnosis and prognosis (Photo 2). The ungular tissue or bulbar mass below the heels (red dots in Photo 2) consists of collagenous tissue rich with circulation. An object penetrating the heel area can cause abscessation of the tissue and possible bacterial migration along the ungular cartilage, which may even gain entrance to either the distal interphalangeal or proximal interphalangeal joint.
Photo 2: A typical solar view of a hoof. The colored dots indicate the approximate puncture sites and the underlying structures.
Nails or other objects that enter the middle and medial sulcus of the frog (green dots in Photo 2) often go in at an angle, following the path of least resistance toward the deep flexor tendon (Photo 3).
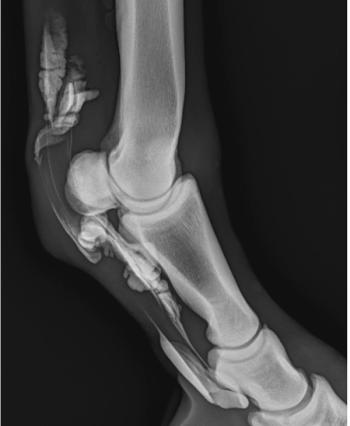
Photo 3: A radiograph with a probe inserted to the depth of the navicular bone.
Street-nail procedure
Objects penetrating the palmar half of the frog (green dots in Photo 2) are capable of causing devastating injury, as the deep flexor tendon, navicular bone and its bursa lie in this area. The ideal surgical procedure for this problem is commonly called the street-nail procedure.
For wounds that penetrate to the depth of the deep flexor tendon, navicular bone or navicular bursa, aseptically prepare the foot for surgery, perform an appropriate block and place a tourniquet at the level of the fetlock. General anesthesia is often preferred to provide the best access and sterility.
Make a large rectangular incision (around the puncture wound) through the palmar frog. The incision should be large enough to give good visualization of the surgical site. It's easiest to lift out the frog and surrounding tissue in layers. This allows slow access to the site and continued step-by-step visualization of the foreign body tract.
Perform a culture and test sensitivity when first reaching the end of your surgical incision (i.e., the appearance of devitalized tissue). When you've reached the deep flexor tendon level, remove any tendon that appears dark, soft and devitalized. Check the surrounding tissue for damage or debris. If the navicular bone also appears devitalized, use a curette to scoop out all necrotic portions of the bone until healthy white bone tissue is observed.
If you're unsure as to whether the navicular bursa or distal interphalangeal joint have been compromised by the penetrating object, infuse the joint through the navicular bursa or through a traditional distal interphalangeal injection site with saline solution and appropriate full-spectrum antibiotics. This will either yield a flow with pooling in your surgical site or will appear patent and under pressure.
Once the wound is clean of all devitalized and necrotic tissue, perform a strong saline flush of the site, and then pack it with antibiotic-impregnated polymethylmethacrylate beads (AI PMMA). Using pressure, fill the rest of the lesion with gauze soaked with diluted povidone-iodine. The most commonly used antibiotic for AI PMMA is imipenem and cilastatin (Primaxin—Merck & Co.).
Postsurgical care
Deep structures in the palmar half of the frog that have been penetrated will rapidly grow exuberant granulation tissue. The necessity for pressure packing the surgical site cannot be stressed enough. Deep packing under pressure allows the structures to regrow without producing granulation tissue. The packing should be changed daily, and the AI PMMA beads should be changed every 10 days (Photo 4).
Photo 4: AI PMMA beads within a street-nail surgical incision that are ready for replacement with fresh beads.
It is important to apply a Patten shoe with a hospital plate (Photo 5). If the deep flexor tendon has been affected, apply the Patten shoe before surgery and the 3-inch bar postoperatively.
Photo 5: A typical Patten shoe with removable 3-inch bar.
Lower the Patten shoe bar as the wound heals. The foot will require shoe removal and trimming four to six weeks postoperatively; at that time, the Patten bar can be lowered to 23/4 or 21/2 inches. If the horse is lame after the bar height is reduced, go back to the height you just removed. The reduction in bar height provides a step-down process for the deep flexor tendon that allows it to accommodate small increments of increasing load during the healing process (Photo 6).
Under no circumstances should you allow the horse to load the foot without the Patten shoe in place, as further tearing and disruption of the affected area will occur. (Note: If either the navicular bone or navicular bursa has been damaged, then the deep flexor tendon has as well.)
Photo 6: Patten shoe bars that decrease in height by 1/4 to 1/2 inches.
Objects may penetrate in front of the frog in the area directly distal to the third phalanx (P3) (blue dots in Photo 2). Infections in this area can cause full solar abscessation and bone infections with sequestrum. A 65-degree dorsopalmar view of the P3 will demonstrate fractures, sequestra that appear as darker bone than the surrounding bone of normal lucency (Photos 7 and 8, p 5E). Injecting a radiopaque liquid into the puncture site and then radiographing it will help determine the extent of the solar disruption (Photo 9, p 5E). Wounds with small penetrating tracts but with large areas of solar disruption should be injected daily with an antibiotic such as amikacin.
Photo 7: A puncture wound to the P3 that has been open and the necrotic bone removed. Note the shoe and hospital plate were affixed to the foot before surgery.
Penetration of the sole as it approximates the hard hoof wall in areas other than those just described (yellow dots in Photo 2) tend to cause painful abscesses of the solar corium, but if treated correctly they will rarely cause problems to other foot structures.
Photo 8: A radiograph of the foot in Photo 7 after surgery. Notice all dark bone and sequestered fragments have been removed.
In addition, keep in mind that all wounds to the solar corium of the foot will cause protrusion of the corium. This is extremely painful and requires a pressure foot packing over the opening to force the corium back inside the foot. Even minor wounds fall into this category.
One of the complications that may arise from penetrating wounds that are sufficiently painful to produce a nonweight-bearing stance is laminitis of the unaffected feet. It's well worth your effort to protect these feet from the beginning. Losing a case to secondary complications is emotionally devastating to everyone involved.
Photo 9: A lateral radiograph of a probe inserted into a puncture wound that reached the depth of the P3 body. Note the arrows showing the injection of a radiopaque fluid into the clean tract demonstrating the undermined sole.
Conclusion
Penetrating wounds, even complicated ones, can be treated successfully — just remember that some require more extensive time, work and patience than others.
Andrea E. Floyd, DVM, has specialized in equine podiatry for more than 25 years. She is the owner of Serenity Equine, Evington, Va., and the author of Equine Podiatry. Dr. Floyd is a member of the American Veterinary Medical Association, American Association of Equine Practitioners and the American Farriers Association.