Neurologic conditions of neonates (Proceedings)
The neurologic examination of the foal has many similarities as that of the adult horse but there are some important differences.
The neurologic examination of the foal has many similarities as that of the adult horse but there are some important differences. Any neurologic examination should begin with observation of any deviation of behavioral patterns or events. The newborn foal should assume sternal recumbency soon after birth, stand within two hours of birth and nurse within three hours of birth.
The foal should be mentally alert during this time. Foals may exhibit submissive behavior when approached by a human or a horse besides its dam. The general activity of foals is eating, sleeping and running in circles around their dam! A pattern of eating and sleeping is established early with the foal usually lying down after a meal. Normal foals are easily aroused from their sleep. Submissive behavior in the foal consists of raising its head and exhibiting a chomping motion with its mouth.
Some important differences are noted in the cranial nerve examination of the foal versus the adult horse. Foals lack a menace response for the first few weeks of life. This is learned reflex. Because foals have a high sympathetic tone they will often appear to lack pupillary light reflex. Pupils may have a slight ventral medial deviation until 1 month of age. Foals also have an inconsistent response to the “slap” test. Cranial nerves 5,7,9,10,11 and 12 are needed for an effective nursing/suckle. Finally the foal may be noted to protrude its tongue to one side but still have good tongue tone.
The spinal reflexes of the foal are usually hyper reactive in comparison to adult. They may have a strong extensor rigidity at first and crossed extensor reflex is common in the contralateral limb in response to withdrawal reflex for first 3 weeks of life. Strong restraint of newborn foal may result in collapse. The newborn foal's gait is choppy and dysmetric at first but becomes more coordinated each day.
Localizing the lesion is the goal of the neurologic examination. The most common neurological signs that foals are presented for include depression, lack of suckle and seizures. These signs would localize the lesion to the brain of the foal. The clinician needs to keep in mind that other non-neurological diseases can present with these signs, problems such as septicemia and hypoglycemia. The differential for these signs in the foal can be divided into acquired problems or those that are congenital. Acquired problems include neonatal encephalopathy, trauma, septic meningitis and as mentioned before metabolic such as hypoglycemia. Congenital problems that result in neurologic disease in the foal include CNS or skeletal malformations and genetic defects.
Neonatal Encephalopathy
Neonatal encephalopathy (NE) is the most common cause of seizures in the newborn foal. The etiology of NE is not simple – it has been felt that an asphyxial event plays an important role. In near term fetal monkeys - hypoxia must be sustained for a period of 60 minutes for neuronal swelling to occur. The neonate is adapted to handle short non-progressive periods of hypoxia. In the foal a sustained progressive hypoxia could be brought about by premature separation of the placenta during parturition, umbilical cord torsion or chest compression during delivery.
A more recent theory by Palmer et al as to the etiology of NE suggests that mares with untreated placentitis were 3.4 times more likely to produce foals with NE and that treatment of placentitis in the mare had a protective effect against NE (OR= 0.15). It is hypothesized that placentitis results in cytokine production in fetal fluids and a fetal inflammatory response syndrome (FIRS). Proinflammatory cytokines in the fetal circulation may increase blood brain barrier permeability resulting in leak of cytokines into the brain and activation of the microglia – neuroinflammation. The real etiology may be a combination of both with neuroinflammation making the brain more susceptible to hypoxic ischemic insults.
Hess-Dudan makes a distinction between 2 types of NE foals based on the appearance of their clinical signs. Some foals will have clinical signs at birth. The delivery or placenta may be abnormal, and foals look more immature. It is felt that there may be due to chronic insult in utero. A second set foals may have a delayed onset of clinical signs. These foals are usually born full term. They appear clinically normal at birth and may even stand and nurse. The onset of neurologic signs in these foals begins within 6-12 hours. In these cases it is felt that the insult took place at time of delivery.
The clinical signs that can be seen in affected foals include loss of suckle, loss of affinity to the mare, depression, recumbency and finally seizure activity. Clinical signs may include all of the above or may stop at any stage.
Diagnosis is made through elimination of other causes of depression and seizures in the newborn foal. Complete blood work including a CBC and glucose helps to rule out in utero infection or hypoglycemia. Examination of the placental may be helpful to identify placentitis. Gross changes may not be evident and histopathology of the placental tissues may be more definitive.
The first goal of treatment in any foal with seizure activity is to eliminate the seizures and prevent recurrence. Diazapam or midazalam (0.11-0.44 mg/kg) is safe and effective for short term anti-seizure effect. The disadvantage of these drugs are that they have a short duration of action and need for multiple dosages. Phenobarbital (2-10 mg/kg as needed) is a longer acting anti-seizure medication but it is easy to over dose the foals and it may cause respiratory depression, hypotension and hypoperfusion. It is important to start with the lower dose and infuse slowly over 15 minutes. The peak effect occurs in 45 minutes. If seizure activity continues then give an additional dose to effect.
Treatment of the NE foal is mostly supportive but it is labor intensive. Foals need constant observation in order to prevent self trauma. Eye care is necessary to prevent ulceration. Nutrition must be provided for the foal via an indewelling nasogastric tube every 2 hours because they often lack a suckle response. Decubital ulceration can occur from the recumbency so soft cushions and leg wraps will help to prevent this.
Head Trauma
Head and neck trauma are fairly common in the history of seizuring foals. Foals will react to restraint by rearing up and falling over backwards hitting the poll of their heads. The resultant force can fracture the skull or produce subdural hematomas. Fractures of the frontal and parietal bones, temprous petral bone and basisphenoid bone are common. Intracranial bleeding can occur in the subdural space or can be parenchymal. Cerebral trauma will present with signs of blindness, depression, head pressing, seizure and coma. Brain stem trauma may produce signs of nystagmus, facial paralysis, strabismus and/or gait abnormalities.
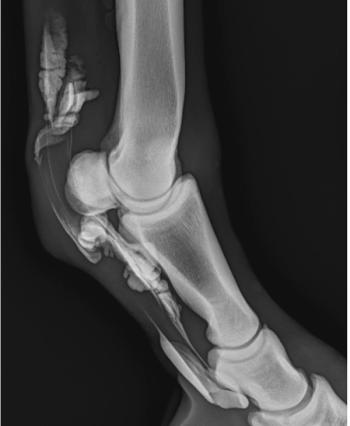
Trauma usually has an acute onset which may be witnessed by owner so diagnosis of the cause of seizures is known. It is important to determine the extent of the injury in order to determine a prognosis. Radiographs of the foals head may not be as helpful as one may expect. The foal's skull has multiple radiographic suture lines which make it difficult to recognize fractures unless they are displaced. A CT or MRI of the head is more diagnostic. These modalities will image the bone component but also the subdural space and brain parenchyma.
The prognosis for head trauma can be good if it is restricted to minor subdural hemorrhage but extremely grave if it involve parenchymal damage. Treatment is mostly supportive care.
Septic Menigitis
Septic meningitis in the foal is a manifestation of septicemia. One report found approximately 10% of confirmed septic foals had meningitis. I have found it to be an infrequent manifestation of septicemia. Foals usually have a history of failure of passive transfer and signs of sepsis. Additional neurologic signs that they may present with include cervical pain, proprioceptive deficits, intention tremors, seizures, opisthotonus and coma. It may be difficult to distinguish meningitis from neonatal encephalopathy by clinical signs alone. Generally septic meningitis is a slower onset than NE.
The pathogenesis of septic meningitis is hematogenous spread of bacteria. The CNS of the equine neonate has an incomplete blood-brain barrier. Bacterial seeding can take place through open tubulocisternal endoplasmic reticulum of the cerebral endothelia and choroid plexus epithelial cells. Cerebral spinal fluid acts as a good growth media and there are inadequate immune defenses to stop proliferation.
The diagnosis of septic meningitis is the same as the diagnosis of sepsis with the addition of a CSF tap. CSF can be obtained from either the atlanto-occipital or the lumbo-sacral space. Normal CSF should be clear, pale yellow and have few cells (1-5 cells/μl). These cells should be monocytes or lymphocytes. Neutrophils are not present in normal fluid. CSF protein ranges from 82-138 in normal foals. Foals with septic meningitis will have CSF that is cloudy in color and have increase protein and cells with a differential cell population that includes neutrophils.
The basic treatment of septic meningitis is the same as that for sepsis with the exception of antibiotic choice. The antibiotics that we use as a first line of defense for septicemia do not penetrate the blood brain barrier even in the inflamed state!. Antibiotics that penetrate CNS include the following: Chloramphenicol – effective against gram +, Trimethoprin sulfa - increasing resistance, Cefotaxine –broad spectrum, bactericidal, and Ceftazidime- broad spectrum, bactericidal.
Prognosis for septic meningitis is poor.
Congenital causes for seizure-like activity
Lunn reported a familial occurrence of narcolepsy in miniature horses. Signs of narcolepsy were present at birth or within 3 days of birth. Foals would collapse when stimulated by suckling or handling. Clinical signs lessen as the foals mature.
Egyptian Arabian foals appear to have 2 different types of seizure problems. The first is a benign pediatric epilepsy. The foals are normal between seizures which may be single or multiple,. Central blindness may be seen during postictal phase;. Prognosis is generally good with the foals outgrowing the signs in a few months. The second type of seizures seen in the Egyptian line is called Lavender foal syndrome. It is called such because affected foals have a washed out coat color that may have a lavender appearance. These foals show constant seizure activity from birth that is non-responsive to anticonvulsants. It has been suggested that this is due to a defect in the choroid plexus. Prognosis for this problem is grave.