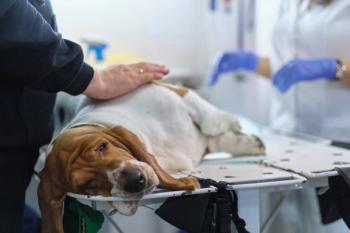
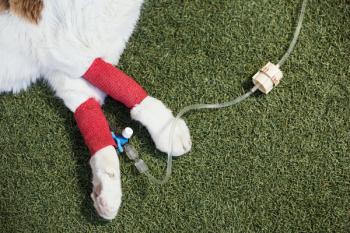
Canine rehabilitation evolving to aid arthritic, post-op patients
Dr. Darryl Millis, DVM, Dipl. ACVS, CCRP answers questions about the growth of rehabilitation therapy, common conditions encountered and how they are treated, advice to veterinarians and owners and his views on where the field is going.
KNOXVILLE, TENN. - Shortly after concluding his residency, Darryl Millis, DVM, Dipl. ACVS, Certified Canine Rehabilitation Practitioner (CCRP) and professor of orthopedic surgery at the University of Tennessee College of Veterinary Medicine, noticed that human athletes who had been injured were usually able to return to elite function after suitable recovery and therapy. It was this observation that sparked his interest in applying similar concepts to the care of injured animals. DVM Newsmagazine spoke with him about his work in animal rehabilitation and the care of dogs in particular.
Dr. Darryl Millis (PHOTO: STOCKBYTE/GETTY IMAGES)
DVM: How has the field of rehabilitation grown in the last few years? Which types of treatments are most common?
Dr. Millis: Our biggest users of rehabilitation are from postoperative care but we are seeing more chronic, geriatric, nagging-injury types of cases, where they have arthritis in multiple joints and they're not candidates for surgery or there's no surgical technique that would be appropriate for them at the present time. They come in primarily for aquatic treatment, both underwater treadmill and swimming. The buoyancy of the water helps take some of the pressure off painful joints plus they receive all of the other benefits of aquatic therapy — cardiovascular, muscle strengthening and joint motion.
We still use therapeutic exercises, cryotherapy, heat therapy, passive range-of-motion, stretching; those are all very important parts of rehab. But we're also using things like extracorporeal shock-wave therapy, low-level lasers and neuromuscular electrical stimulation.
DVM: What are the most common conditions you see? Describe the challenges of working with your canine patients.
Dr. Millis: We see a lot of postoperative intervertebral disk patients. They go into and come out of surgery with different degrees of disability. Our goal is to try and keep their musculoskeletal physiology healthy, like providing resistance training, though they may not be able to move their legs, trying to keep some tone in the muscles and normal range of motion in the joints.
As they begin to develop some motor function, the keys are to assist them in a standing position so they can use their forelimb muscles, trunk, abdominal and back muscles to try to keep the body upright, and to begin work on re-patterning their gait.
Swimming is a great way for dogs to use their voluntary motion naturally and begin moving their limbs in somewhat of a rhythmic pattern. The final stage would be normalizing the gait so they don't drag their feet or stand with their feet in an abnormal position, and to work on balancing. We do a lot of proprioceptive activities such a wobble boards, walking on irregular surfaces and other unbalancing exercises. All of those things help dogs learn where their feet are in space and how to respond to perturbations in the position of the body so they don't fall over.
The other common thing we do is postoperative care for tibial plateau leveling osteotomy surgery for cruciate ligament rupture. Initially we work on keeping the swelling down and getting the dog's range of motion back. If we don't get it back by two weeks post-op, some of those patients will have permanent loss of motion. We don't want to have too much force placed on the leg initially because the joint and tissues are remodeling, and if we get too aggressive too early we may actually make things more painful.
So, we do low-level activities for the first three weeks or so. Then we start them on an increasingly challenging program, including limb use, pain control and muscle strengthening. Hopefully by about six to eight weeks after surgery they're pretty much returning to normal.
The biggest challenges of working with dogs are motivation and verbal communication. It's not the type of thing where we can tell them to lift their leg 20 times as in human physical therapy. But there are a lot of things we can use that they like doing and can be trained to do, such as going up and down stairs or sit-to-stand exercises.
One of the things we want is to have functional activities, and with the dog that means walking, trotting and running. Underwater treadmills take advantage of the dog's natural gait patterns and help strengthen the patient because of the resistance that comes from moving through water. And dogs walking in water have a very exaggerated joint motion. So we're getting muscle strengthening, gait patterning and a greater range of motion than we could achieve with normal dry-ground activity.
DVM: Are canine rehabilitation procedures merely adaptations of those used on humans, or are some techniques specific to animals? What kind of sharing goes on between the two disciplines?
Dr. Millis: I do think that's the way the field should go, with collaborative efforts, because physical-therapy techniques are not taught to a great extent in veterinary colleges, and veterinary applications are not taught in human physical-therapy colleges. It could be dangerous to apply certain types of treatments to animal conditions if you don't know the basic physiology, anatomy and disease conditions that animals have, as well as appropriate rehabilitation techniques.
I think there should be a certain knowledge base, skills and training with animals before being able to treat them. This is a potential issue that will have to be addressed by state practice acts. In almost all states physical therapy/rehabilitation must be performed under the direct supervision and referral of the veterinarian, regardless of who is performing it. But state practice acts are so varied; some of them are very clear and some are not as clear.
If we want this discipline to move in a credible, scientifically sound fashion, then we have to provide basic entry-level training to people who want to see this area grow and learn how to do it correctly. That was part of the reason we started our certificate program — to protect the public and make sure animals weren't harmed. We're the only university-based course in the United States that offers rehab training. We also offer the course in Europe. Close to 400 people have passed the examination and have their CCRP. In terms of total numbers of people who have taken the courses, it is approaching 2,000.
DVM: What advice would you give veterinarians and owners who have animals in need of rehabilitation but who are not near a dedicated facility?
Dr. Millis: It's nice to have all the extra tools such as aquatic therapy, neuromuscular electrical stimulation and ultrasound, but you can do a lot with just your hands and basic exercises.
Something as simple as a passive range of motion, stretching, cryotherapy and low-level activities right after surgery are very important. And many are already doing basic rehab such as changing an animal's activity level, maybe promoting some additional work like stepping over cavaletti rails or going up and down stairs or ramps — basic exercises for strengthening and overall joint function.
The best way to find a certified practitioner is to go to the Web site
DVM: Where is the field of animal rehabilitation going?
Dr. Millis: The next 10 to 15 years are going to be really exciting. Right now before the AVMA there is a proposal to form an American College of Veterinary Sports Medicine and Rehabilitation. It's in the one-year, public-comment period, and if all goes well there will be a specialty college similar to internal medicine or surgery.
Outcome assessment is a big area that we've been actively researching and trying to compare different types of protocols to see what makes the biggest difference. We have a study going on with the Morris Animal Foundation to look at the efficacy of low-level lasers, transcutaneous electrical nerve stimulation and acupuncture for hip and stifle arthritis.
More and more people are incorporating rehabilitation as part of an overall treatment program but there is still much room for improvement. My goal is for every postoperative patient to have some rehab, whether it's a home-care program or a professionally administered one.
Wetzel is a free-lance writer in Cleveland, Ohio.