Another skinny horse with a normal physical exam: Now what? (Proceedings)
Weight loss or ill thrift is a common presenting complaint for many medical problems of horses.
Weight loss or ill thrift
Weight loss or ill thrift is a common presenting complaint for many medical problems of horses. These cases can be frustrating because physical exam findings, including rectal palpation, are often unremarkable. However, an ordered approach to further evaluation is useful for equine practitioners to diagnose many medical disorders as well as to determine when referral to a hospital may be the next logical step. In addition, a standardized approach to horses with weight loss allows the practitioner a more realistic expectation of what services a referral hospital may or may not be able to provide for their clients.
History and physical examination
During performance of the physical exam on horses with weight loss, it is important to collect a complete history while also attempting to document the magnitude and time course of weight loss. A helpful tool can be implementation of body weight measurement (weight tape) and body condition scoring (BCS) during semiannual or annual preventive care visits. Having this information within the past few months would allow a practitioner to have a comparison basis to better document weight loss.
Performance of a rectal examination on horses with weight loss, especially when results of the remainder of the physical exam are unremarkable, cannot be overemphasized. Rectal palpation can reveal abdominal masses including neoplasia or abscesses due to metastatic Streptococcus equi subspecies equi or Corynebacterium pseudotuberculosis infections. In addition, abnormal kidneys and ureteroliths can be palpated in some horses with chronic renal disease. When performing a rectal exam on a horse with weight loss, it is important to attempt to reach the mesenteric root by palpating the aorta as far cranially as possible. The root of the mesentery contains a number of lymph nodes and is a common location for abdominal abscesses.
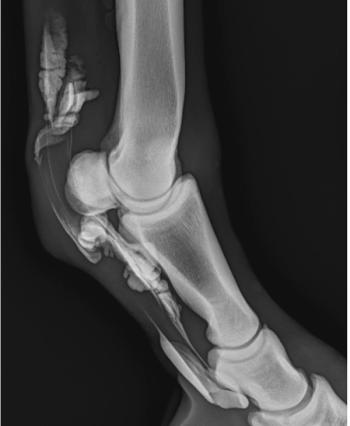
Next, the importance of a complete oral exam also cannot be overemphasized. For example, over the past decade I have seen several horses referred for evaluation of a poor appetite that had a stick lodged between the upper dental arcades (Figure 1). A complete dental exam is also essential, especially in horses 15 years of age and older in which poor dentition may be the primary problem (Figure 1).
Figure 1 A stick can be seen lodged between the upper dental arcades in the oral cavity of a horse that presented for weight loss over the past week along with a decreased appetite (left); dental abnormalities such as the large hook on the caudal upper cheek tooth (right) can also lead to weight loss and a decreased appetite.
Assessment of management and appetite
Before more serious medical conditions that lead to weight loss (and referral) are considered, it is essential to determine whether or not the horse is actually consuming an adequate amount of feed daily to maintain body condition. In a group setting dominant horses may chase younger and less competitive horses away from feed and correction of weight loss may simply require separation of the group at feeding time or breaking the herd into smaller groups with less of a dominance hierarchy. Next, during cold weather caloric requirements increase and if feed availability is not increased weight loss will ensue. In this situation most of the horses in the herd are found to be thin, rather than a single individual. Thus, when the horse in question is part of a herd, it is essential to look at the remaining horses to determine overall body condition of the group: more severe weight loss in an individual animal would support a medical condition while an overall decrease in condition of the herd would support a management problem. To further answer the question of whether or not a horse is eating adequately or not, it is often helpful to offer the horse a flake of hay or a couple of pounds of concentrate feed as part of the initial evaluation. "Quidding" or dropping of chewed up hay boluses can be observed and the horse's aggressiveness of eating can also be assessed.
Initial blood work
Collection of blood samples for a complete blood count (CBC) and serum biochemistry profile is generally warranted in horses with ill thrift. The CBC is probably the less rewarding of these tests. Frequently, mild anemia (packed cell volume [PCV] of 27-30%) is the only abnormality detected. Mild anemia may be a consequence of chronic disease but it is also important to recognize that PCV values of 29-31% may be normal for adult horses that are not in a regular exercise program. Occasionally, however, rare conditions such as leukemia may only be detected with a CBC.
Chronic renal disease is probably the best example of a medical disorder leading to weight loss that can be easily detected on serum biochemistry: detection of azotemia with hypercalcemia is pathognomonic for chronic renal disease. Chronic liver disease is most often supported by an increase in gamma-glutamyl transferase (GGT) activity as increases in activity of this enzyme are specific for the liver. Finally, it is important to look at total protein, albumin, and globulin concentrations. Detection of either increased total protein concentration or hypoproteinemia typically directs further diagnostic testing. An elevated protein concentration is a consequence of an increase in globulin concentration as the only cause of hyperalbuminemia is dehydration. An increase in globulin concentration supports chronic inflammatory disease including chronic infection (e.g., abdominal or thoracic abscess, cholangiohepatitis, pleuropneumonia, and others) or neoplasia. In contrast, a decrease in total protein concentration in the horse is almost always indicative of a protein-losing enteropathy (PLE), although a rare horse with hypoproteinemia may have neoplasia with large volumes of pleural or peritoneal effusion or a glomerulopathy. When an owner may be reluctant to spend the money for a CBC and serum biochemistry profile, a less expensive option is to collect a sample of EDTA-anticoagulated blood to determine PCV and total solids (TS) with a refractometer. TS provides an estimate of total protein concentration (in the absence of hemoglobinemia or lipemia); thus, it can prove to be a useful screening tool for presence of hyper- or hypoproteinemia.
Specific medical problems that may present with weight loss
The list of medical problems that can present with a complaint of weight loss is extensive. For the remainder of this presentation, the discussion will be limited to the emerging PLE consequent to Lawsonia intracellularis infection, inflammatory bowel diseases (IBDs), and chronic liver disease consequent to either infection (cholangiohepatitis) or hepatotoxicity.
Lawsonia intracellularis
Lawsonia intracellularis infection causes a syndrome of ill thrift and weight loss (without obvious diarrhea) that has been coined "equine proliferative enteropathy" (EPE). EPE has emerged as an important disease of foals and weanlings over the past decade but disease in older horses has not yet been recognized. Lawsonia intracellularis has long been known to cause proliferative enteropathy in pigs. In both species, the organism is typically found in the apical cytoplasm of intestinal crypt cells. Infection results in crypt cell expansion and elongation that manifests grossly as hyperplasia and thickening of the distal half of the small intestine. Inflammatory cells and goblet cells are reduced or absent but lack of a functional brush border leads to malabsorption and weight loss. Fecal shedding occurs as infected epithelial cells are sloughed into the intestinal lumen. With pigs the disease spreads through comingling of carrier animals with naïve pigs but in horses the source of infection and means of transmission remains unclear (although a fecal-oral route is probable). EPE commonly affects only a few individuals in the herd although larger outbreaks have been described.
Affected foals and weanlings are usually not recognized until they have been infected for one or more weeks. Although they may have mild diarrhea, this is not a consistent finding and the most common presenting complaints are weight loss with a dull attitude (ill thrift). Characteristic findings include marked hypoproteinemia (<3.0 g/dL) in combination with thickened small intestinal walls (wall thickness often >1.0 cm; normal is <3 mm) detected on abdominal ultrasonography (Figure 2). In addition, more careful palpation of the ventrum often reveals mild to moderate ventral edema. In fact, these findings are nearly pathognomonic for EPE in a foal or weanling.
A recent retrospective study of 57 foals and weanlings with L. intracellularis infection revealed an age of onset from 2 to 8 months of age. Further, a seasonal occurrence was noted with animals affected from August through February but it was unclear whether this seasonality was due to increased risk of exposure or was simply consistent with the age at which foals and weanlings are most susceptible. 81% of the young horses had ventral edema and all had moderate to severe hypoalbuminemia (74% <2.0 g/dL). Fever and diarrhea were found in only 19% and 32% of affected patients, respectively.
Figure 2 Transabdominal ultrasonographic image of a weanling foal with severe hypoproteinemia and thickened small intestinal walls consistent with Lawsonia intracellularis infection.
Lawsonia intracellularis is a fastidious organism that cannot be cultured from feces; thus, testing of feces by polymerase chain reaction (PCR) is pursued in an attempt to establish a definitive diagnosis. However, both false-positive and false-negative PCR test results can occur as the organism can pass through the intestinal tract without causing disease and intermittent shedding of infected epithelial cells in a foal with clinical disease could leading to varying test results. Consequently, an immunoperoxidase monolayer assay (IPMA) to detect antibodies in serum can also be used to assess infection and an IPMA titer >60 is considered positive for L. intracellularis infection. In the report of 57 cases, 38/51 horses tested positive by fecal PCR and 38/47 had a positive serum IPMA titer. Only 26 foals had both positive fecal PCR and positive serum IPMA results while 13 horses had a positive serum IPMA but a negative fecal PCR and nine horses had a positive fecal PCR but a negative serum IPMA titer. In the same report the authors also tested 103 apparently healthy herd mates of the sick foals and found six with positive fecal PCR test results and 34 with positive serum IPMA titers (both tests were not performed on all foals).
Treatment of foals with L. intracellularis infection includes supportive care (fluid therapy, colloids, and parenteral nutrition in more severe cases) and antimicrobial agents. The organism is susceptible to macrolides (erythromycin, azithromicin, or clarithromicin), chloramphenicol, and tetracyclines. The most common treatment is IV oxytetracycline for 5-10 days and some practitioners follow-up with doxycycline after IV treatment has been discontinued. In the report of 57 foals, 93% survived but recovery can be prolonged (several months) and musculoskeletal complications such as tendon laxity can develop from the prolonged cachexia. Further, these foals were predominantly bred for racing and their sale price was lower than healthy foals from the same sires when the recovered patients were sold at yearling sales.
Inflammatory bowel disease
Inflammatory bowel diseases (IBDs) can cause weight loss, ill thrift, and intermittent colic. Although classic cases that present with moderate to severe weight loss and hypoproteinemia (primarily hypoalbuminemia) are uncommon, it is probable that more subtle forms of these diseases also occur in horses with mild weight loss or recurrent colic. IBDs should be considered in horses with weight loss or recurrent colic in which other problems (e.g., gastric ulcer disease, parasitism, sand accumulation, NSAID sensitivity, etc.) have been excluded. Although both are non-specific findings, detection of mild to moderate hypoalbuminemia and thickened intestinal walls on transabdominal ultrasonography can be supportive findings. Additional diagnostic tests worthy of consideration include a carbohydrate absorption test and rectal mucosal biopsy. IBDs are further characterized by histological changes in the bowel mucosa and submucosa into distinct diseases.
Granulomatous enteritis. Granulomatous enteritis (GE) is characterized by weight loss and soft feces can accompany more advanced stages of the disease. Diagnosis is supported by "flat" carbohydrate absorption curves and evidence of lymphocytic-histiocytic submucosal infiltrates in bowel biopsy samples. The cause is suspected to be an inappropriate or excessive response to unidentified antigens. In some instances, a similar syndrome has been caused by intestinal lymphosarcoma and Mycobacterium avium has been isolated from affected bowel and mesenteric lymph nodes in a few affected horses.
Multisystemic eosinophilic epitheliotropic disease (MEED). MEED has some similarities to GE; however, bowel submucosal infiltrates are predominantly eosinophilic and affected horses also commonly have nodular and ulcerative skin lesions. The latter often affect the coronary band and may cause lameness. As with GE, the cause is suspected to be an inappropriate or excessive response to unidentified antigens. The diagnosis is established by detecting eosinophilic infiltrates in skin and bowel biopsies.
As with the other immune-mediated diseases, corticosteroids are the treatment of choice for GE and MEED. Generally, corticosteroid therapy produces transient improvement for a period of months to a couple of years but the long-term prognosis for these disorders remains guarded. Further, development of laminitis is always a concern when long-term corticosteroid treatment is used.
Chronic liver disease
Both cholangiohepatitis and hepatotoxicity (with ingestion of pyrrolizidine alkaloid containing plants or alsike and red clover) can have weight loss as the presenting complaint. With cholangiohepatitis, recurrent colic and recurrent fevers may also be recognized. With hepatotoxicity, secondary photosensitization of the non-pigmented skin can also be a presenting complaint. Physical exam of horses with liver disease often reveals a dull attitude but occasionally hepatic encephalopathy can also develop. Detection of icterus is variable but, when present, supports liver disease. Clinicopathological assessment reveals elevated hepatic enzyme activities allowing diagnosis of hepatic disease as the primary problem. A simple clue that ingestion of a hepatotoxic plant by horses at pasture is the cause of liver disease is detection of photosensitization and elevated hepatic enzyme activities in several horses within the group while cholangiohepatitis typically affects individual animals. Transabdominal ultrasonography is useful to assess liver size in horses with liver disease. Obstructive disease (cholangiohepatitis with or without associated choleliths) typically leads to an enlarged liver with a rounded edge that extends beyond the costochondral junctions on the right side. A liver biopsy is relatively east to collect and provides useful information for prognosis (extent of hepatic fibrosis).
Treatment of cholangiohepatitis requires long-term antimicrobial treatment, usually with a potentiated sulfonamide, until liver enzyme activities have returned to normal. This may require months of antimicrobial treatment and GGT activity is the one to monitor. Periodically, colic episodes or exacerbation of liver disease resulting in anorexia may need to be addressed with further supportive care (e.g., fluid therapy, NSAIDs, etc.). Treatment of hepotoxicity is supportive once exposure to the offending agent has been stopped. In the upper Midwest, the primary cause of hepatotoxicity is ingestion of alsike and red clover and treatment is warranted because the prognosis is generally favorable. Treatment of photosensitization may require administration of corticosteroids systemically and topical skin therapy. Further exposure to ultraviolet light can be prevented by stabling horses during the day and/or applying sun block to nonpigmented skin.
Supplemental readings available on request to the author