"Wheal of Fortune": Approaching and managing the allergic patient (Proceedings)
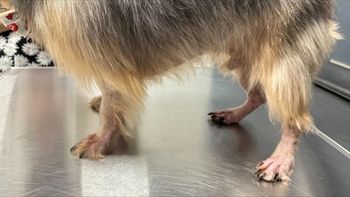
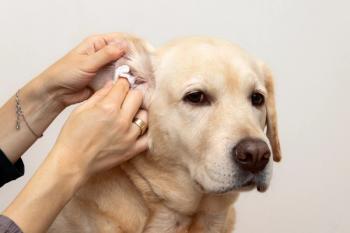
Pruritus, in its various forms, is a common complaint in small animal practice and has a multitude of causes. Many clients want to know what is making their pet itchy, they want an accurate answer quickly, and they want immediate relief for their pet.
Pruritus, in its various forms, is a common complaint in small animal practice and has a multitude of causes. Many clients want to know what is making their pet itchy, they want an accurate answer quickly, and they want immediate relief for their pet. Therein lays the pickle, of course. A "derm work-up" can be time consuming and the one therapy that helps most conditions (at least temporarily), comes with a host of side effects. This is the diagnostic and therapeutic approach I take that seems to cause me the least amount of self-induced alopecia and helps the client understand the complexity of this problem.
Ask questions
I take a team-approach to medical history gathering, the most important diagnostic event in a dermatology work up. When an itchy pets comes in, the clients fill out a questionnaire regarding their perception of the problem; the staff has questions they are trained to ask; and I ask questions. This information, before I've even examined the pet, allows me to generate and rank differentials (e.g., is this likely a contagious problem, allergies, etc). You can skip the questionnaire and who or you staff can ask some key questions:
1) At what age did the problem start?
< 6 mons: r/o parasites, cutaneous adverse food reactions (CAFR)
1-3 years: r/o atopy, flea bite hypersensitivity (FBH) CAFR
5-10 years: infection secondary to metabolic disease, FBH; CAFR
>10 years: neoplasia; CAFR, and fleas.
2) Distribution of pruritus: "Where's the itch?"
If 75% or more of the symptoms are from the "waist" caudally, FBH has to be the primary rule out and strict flea
control is recommended for all (haired) pets in the home.
3) Are any other pets in the home also pruritic? If so, this raises my suspicion of fleas or contagious external parasites such as scabies, cheyletiella, lice, or Demodex gatoi in cats.
4) If there is itch and infection or lesions such as papules, pustules, crusts, or hair loss, which came first?
Infection can be pruritic. If lesions / infection precede itch, make sure to do scrapings ± blood work to rule out immune suppression. Pemphigus foliaceus can cause concurrent pustular dermatitis and pruritus.
5) If problem is long standing, is it seasonal?
6) Has any previous treatment helped or worsened the problem? Make sure to ask if improvement was even temporary.
Causes of pruritus that may not respond to steroids include food hypersensitivity, parasite infections (scabies may improve transiently and then no response), bacterial and yeast infections. Pemphigus foliaceus may respond poorly to anti-inflammatory doses of steroids.
Examining the itchy patient
• Look for evidence of infection: patchy alopecia, papules, patchy scaling, thickened skin, odor. Tape cytology is helpful to identify a yeast overgrowth.
• Check ear margins: if ear margins are scaly and pruritic, think scabies.
• Use a flea comb, good light and paper towel to collect debris / scale / detritus.
• Scrape, scrape and scrape. Demodex gatoi (cats) and Demodex injai mites (dogs) can cause pruritus. Check fecals (hypersensitivity to intestinal parasites; Demodex gatoi or cheyletiella mites may show up in feces).
• If this is a new dermatitis (with primary skin lesions) in an older pet, recommend a biopsy.
If this work does not illuminate a cause and / or you are unable to take time to gather this history and do diagnostics, here is a reasonable approach based on the signalment and persistence of the problem.
Young adult, healthy pet with normal skin, first time offender
• Assure regular and good flea control for all pets in home.
• Start fatty acids and antihistamines.
o Omega 3 dose: ~ 40 mg / kg / day.
o Give client a list of antihistamines to try if first choice does not help.
o Zyrtec: Dogs 2.5 – 10 mg po bid; cats: 2.5 mg po qd – bid.
o Hydroxyzine: D/C: 2.2 mg / kg po bid-tid.
o Chlorpheniramine: Dogs: 2.5 – 8 mg b-tid; cats: 2.5 mg b-tid
o Loratidine: D/C: 0.25 – 0.5 mg / kg / day
o Also: Benadryl, Amitriptyline
• Bathe with gentle shampoo every 2 weeks.
• Use topical anti-pruritic therapy such as topical triamcinolone (Genesis, Virbac).
• Treat infection if present (3 week course of cephalosporin, potentiated amoxicillin, clindamycin).
• Recheck / follow up in 4 weeks.
Adult healthy pet who is a repeat offender
• Educate client that diagnosis is needed (is the food hypersensitivity or atopy).
• Start restricted diet. I explain to my clients that while blood tests are available for food allergies, unfortunately, these tests lack both sensitivity and specificity. Regardless of the results of the test, I am going to recommend a restricted diet. So save your money for the expensive prescription food.
• If level of itch warrants, start systemic corticosteroids (oral preferred). Temaril-P is a good choice for dog >35 lbs; I do not think it works as well in smaller dogs. For cats, I prefer (methyl)prednisolone or dexamethasone; I have also had success with transdermal forms of these steroids in some cats despite lack of documentation of efficacy of this form.
• Treat infection if present.
• Make sure client continues food trial for at least 8 weeks.
• This is also a good time to start epidermal lipid replacement therapy (cerumides, phytosphingosines). A current wave of research in atopic dermatitis (food or non-food induced) is focusing on the inherent defect of the epidermis of these patients. The topical barrier enhancement therapies have potential benefit as an adjunctive therapy (Allerderm Spot-on, Virbac; Seborrhea Spot-on, Douxo; DermaScent, Adventix).
• For the owner who places "getting to the bottom of the problem" at a high priority, I will offer doing food trial and allergy testing / immunotherapy concurrently, with the warning that over time, we may find one or the other to be unnecessary.
• If the food trial fails to control pruritus, then we know we are most likely dealing with atopy. (Occult external parasites should be kept on the list and if any reasonable suspicion of scabies or cheyletiella, do an empirical treatment for this.)
What about contact allergies?
Many clients presume their pets' allergies are to something the pet contacts, such as carpet, laundry detergent, grass, etc. While this is possible, type 4 delayed hypersensitivity reactions such as contact dermatitis are uncommon compared to atopy and CAFR. Signs that make me suspicious of contact dermatitis:
• Symptoms limited to ventrum, feet, medial pinnae, chin.
• Papules and pruritus concurrent with poor response to antibiotics.
• Worsening after known exposure to suspected allergen. Common contact allergens include plastic, concrete, certain plants (such as the Yew plant), and wool. Some items such as carpet cleaner can be a contact allergen or can canuse non-immunologic irritation.
When I do suspect contact dermatitis
• If possible, remove suspected offender.
• Clean carpets using dilution of vinegar in warm water only to remove residual detergent.
• Wipe the ventrum of the pet / affected areas with damp, cool, clean cloth twice a day, especially after contacting suspected allergen.
• Start pet on pentoxifylline, 10-15 mg/kg bid.
• Consider having the pet wear a shirt or body suit to prevent contact.
For the atopic patient non-responsive to antihistamines and restricted diet
First, I assess the need for client education or adjustment of expectations. Phrases that are "red flags" to me:
• When are we going to find a treatment to cure my pet's itching (cure is a four-letter word in my practice)?
• I just want to know what my pet is allergic to.
• So nobody knows what causes this, huh?
• How long do the shots / pills / insert therapy here last?
• These are clients who need eye-to-eye discussion about 1) chronic, incurable nature of allergies; 2) lack of accurate test to identify allergies; testing is to designs immunotherapy; 3) follow up is critical to success.
When to recommend allergy testing and immunotherapy ("I want my cake and to eat it too", therapy)
1) young pet (<6-7 yrs), especially large breed dogs; 2) owner expresses desire to minimize medications with any potential side effects because tgey understand this is life-long treatment; 3) Cats who are indoor / outdoor / hunters where immune suppression could be life-threatening; 4) the household that cannot / will not do a restricted diet.
Which type of testing is best?
Intradermal testing is still considered the "gold standard" because it evaluates presence of IgE and mast cell degranulation within the skin, where most symptoms occur. However, a positive reaction does not mean that reaction if causing the patient's signs (dogs and cats with no dermatitis can have positive reactions on a skin test). Also, there is a subset of atopic patients who have non-reactive skin tests. The skin test is also affected by recent use of systemic and topical steroids and antihistamines as well as fatty acids and some sedatives.
Serologic testing for atopy has the advantage of easy sample procurement and less interference with medications. However, again, these tests are subject to false positive and false negative reactions. Serologic tests may be affected by the time of year and lack of recent allergen exposure. At this time, there is no standardization of testing between the commercial laboratories. Recent work has shown >90% correlation between Greer and HESKA testing, and demonstrated a method to monitor intra- and inter-laboratory standardization, if other laboratories will follow suit.
Obviously I am a bit biased but feel the best option for allergy testing is referral to a dermatologist for intradermal ± serologic testing. Dermatology clinic staffs offer more detailed follow up and adjustment of immunotherapy. If referral is not feasible, the success rate of immunotherapy based on serologic allergy testing is not much lower than that for intradermal testing (IF all other causes of pruritus have been ruled-out). Use a laboratory with good customer service and good quality control (i.e., good intra-assay repeatability).
During the early phase of immunotherapy, medications such as cyclosporine, antihistamines, and low-dose oral steroids can be used to keep the pet comfortable. These supportive medications should be stopped or tapered significantly as the pet reaches maintenance therapy to assess response to the injections.
When to recommend oral cyclosporine: 1) Pet over 6-7 yrs of age (if not cost prohibitive); 2) Owner unable to do immunotherapy; 3) cannot get pet off steroids in order to do allergy testing; 4) immunotherapy has failed. A study presented at the 2009 dermatology meeting showed the 4 weeks of cyclosporine at 5 mg / kg / day did not suppress intradermal or serologic test results. We do not know the effect of longer use of the medication.
One way to make cyclosporine less expensive is to also have the pet (dog) taking ketoconazole. Ketoconazole inhibits the cytochrome P450 system, thereby slowing the metabolism of concurrently administered cyclosporine. Also, some compounding pharmacies can make cyclosporine in a suspension for more tailored dosing of small pets. These "tricks" may affect the bioavailability of cyclosporine compared to the trade name product, Atopica.
Owners do need to be advised of potential side (beyond the GI side effects) effects of cyclosporine (increased risk of viral infections, toxoplasmosis in cats; decreased tumor surveillance). One comment I make is "steroids come with known evils; the side effects of oral cyclosporine are more unpredictable." With that said, I have patients for whom cyclosporine has "saved" their life in the eyes of their owners.
When is it okay to recommend long-term corticosteroids? 1) A dose of < 1.25 – 1.5 mg / lb of prednisone / month keeps pet (dog) comfortable; 2) Older pet in whom nothing else works; 3) owner understands risks v. benefits.
When I am using steroids long term, I give clients blank calendars for them to record the pet's use of steroid (as well as general itch level and other medications). Every 4 weeks I like the calendars return to calculate the mg / lb / month used to know if I need to add in other therapies.
Selected references
1. 20th Proceeding NAVDF 2005, pp. 103 (Fadok); p. 126 (Glaum, MC, MD); p 164 (Patterson, AP);p 191 (DeBoer); p. 196: (Jackson, HA et al)
2. 21st Proceedings NAVDF 2006 p. 161 (Jackson HA); p 192: (Hnilica KA et al).
3. Lee K, Blankenship KD, McCurry ZM, et al. Performance characteristics of a monoclonal antibody cocktail-based ELISA for detection of allergen-specific IgE in dogs and comparison with a high affinity IgE receptor-based ELISA. Journal compilation (c) 2009 ESVD and ACVD.
4. Olivry et al; Vet Dermatol. April 2006;17(2):95-102.
5. Scott D, Miller WH, Griffin CE. Kirk's Small Animal Dermatology, 6th ed. WB Saunders.
6. Task Force on Canine Atopic Dermatitis; Veterinary Immunology and Immunopathology Special Issue 2001.