Tick-borne diseases in humans: The One Health approach
Veterinary professionals beware: tick-borne diseases are on the rise in both humans and animals. Brush up on identifying ticks, diagnosing the diseases they transmit, and treating and preventing them from spreading.
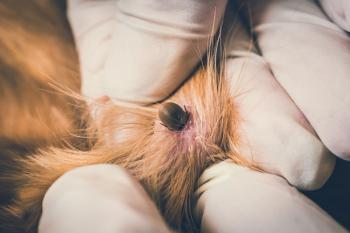
A female black-legged tick (Ixodes scapularis) "questing" for live hosts. (Image courtesy of Dr. Richard Gerhold)
Tick-borne diseases are on the rise in both humans and animals. The Centers for Disease Control and Prevention recently announced that the number of tick-borne bacterial and protozoan diseases in humans in the United States more than doubled between 2004 and 2016, with more than 48,000 human tick-borne disease cases reported in 2016.1 Although diseases such as Lyme disease comprised 82% of all tickborne diseases reported during this period, other important diseases, including ehrlichiosis, Rocky Mountain spotted fever (RMSF) and anaplasmosis, have been emerging in various parts of the country.1
In animals, the prevalence of these tick-borne diseases as well as cytauxzoonosis has increased in many regions. In determining whether tick-borne disease is a cause of illness in animals, a good travel history is imperative given that various species of ticks and tick-borne diseases are more common in certain geographic areas. More information on tick-borne disease distribution and prevalence rates can be found on the
Diagnosis of tick-borne diseases
Testing for tick-borne diseases is warranted in animals with suggestive clinical signs as described below. Polymerase chain reaction (PCR) testing (detection of pathogen DNA) is more sensitive than serology for detecting RMSF and Anaplasma/Ehrlichia species during the acute phase of the disease (prior to the development of an antibody response). Therefore, if an animal presents with acute signs suggestive of tick-borne disease (fever, lethargy, thrombocytopenia, leukopenia, arthropathy, neurologic dysfunction, renal failure), PCR is the best diagnostic test. Whole blood should be obtained for the test before any antibiotic is administered.
Serology is useful for detecting chronic or persistent infections, during which the number of pathogens is lower or pathogens are absent from circulation and may not be detected as easily by PCR. This is particularly true for Lyme disease, given that the Borrelia organism localizes in the tissues and is difficult to detect in the blood. Antibodies to these tick-borne agents may persist for several months to years, so detection of antibodies does not distinguish current infection from previous exposure. Also, high seroprevalence to these agents has been documented in healthy dogs in endemic areas, such as the southern United States, and most dogs exposed to Anaplasma or Ehrlichia species will not develop overt clinical disease. Therefore, tick-borne serology tests should only be the first step in determining whether there has been tick exposure. Follow-up physical exam and ancillary testing, including complete blood cell count (CBC), urinalysis, blood smear and PCR, should be performed before the animal is treated. Animals that are clinically normal and have normal CBC and urinalysis results should be monitored but not treated unless clinical signs develop.
Tick identification
Tick bodies are divided into two primary sections: a fused head and thorax, and an abdomen. Adult and nymphal forms have four pairs of legs, whereas larval forms have three pairs of legs; no ticks have antennae. Establishing whether ticks are larvae or other stages is important in determining the likelihood of the tick being infected with various pathogens. Unless transovarial transmission occurs from adult female to eggs, larvae are unlikely to be infected with pathogens. Because nymphs and adults have acquired more blood meals from various hosts, they are more likely to be infected with a pathogen that is maintained via transstadial transmission. Thus nymphs and adults generally present a higher risk of transmitting a disease.
Ticks are excellent disease vectors due to their persistent blood-sucking ability, resistance to environmental conditions and high reproductive potential among females. Wounds and inflammation may occur just from tick saliva during a blood meal acquisition. These wounds are capable of being infected with a secondary myiasis leading to further tissue trauma and disease.
Ticks are classified as soft bodied or hard bodied. Soft ticks lack a scutum (dorsal, hardened plate) that covers the entire dorsum of males and forms an anterior shield in females. In addition, the mouth parts of soft ticks are located on ventral aspect of the body. Hard ticks, of which there are more species, contain a scutum and have anterior-facing mouth parts-these ticks are encountered more typically in human and animal tick infestations. Furthermore, hard ticks attach to the host and obtain a blood meal until replete. Female ticks fall off after repletion and use blood meal for egg development. Both hard- and soft-bodied nymph and adult ticks can be identified based on visual exam; however, larvae are difficult to identify without a microscopic.
Important ticks that can cause disease in people and animals in the United States are listed in Table 1.
Table 1. Important hard ticks that cause zoonotic disease
Tick Species
Location Affected Species Common Disease Vector Comments
Dermacentor variabilis
(American dog tick) Eastern half of US and West Coast; rare in central US Dogs, cats, humans, horses, cattle, foxes, rodents and other mammals A common vector of RMSF (
Rickettsia rickettsii
); an infrequent vector of tularemia Although its name would suggest that RMSF is most common in Rocky Mountain regions, it is more commonly found in parts of the mid-Atlantic, midwestern, and southeastern US.
Rhipicephalus sanguineus
(brown dog tick) Wide distribution All stages parasitize on dogs and will attach to other animals; humans are nontypical hosts Vector of
Babesia canis voglei
in dogs, tularemia,
Ehrlichia canis
, and RMSF; very important vector of RMSF in humans and dogs in southwestern US This tick species can survive indoors (e.g. house, kennel, veterinary clinic) for months to possibly years without a blood meal.
Amblyomma americanum
(Lone Star tick) Wide distribution, but mainly in southern and mid US; populations are advancing northward All stages feed on wild and domestic animals, birds, and humans; a significant pest for humans and animals Can transmit
Coxiella burnetii
(Q fever), tularemia,
Ehrlichia chaffeensis
,
Ehrlichia ewingii
, RMSF,
Cytauxzoon felis
(cats only); vector of southern tick-associated rash infection in humans Large silver spot on scutum on females only (hence the name “Lone Star”)
Ixodes scapularis
(black-legged tick; previously called deer tick)
Ixodes pacificus
(California black-legged tick)
I scapularis
: Wide distribution in eastern, southern, and midwestern US; highest populations in upper Midwest and New England/mid-Atlantic states
I pacificus
: West Coast Larvae feed on wild animals, nymphs and adults on humans; adults are more common in late fall and winter
I scapularis
: Primary Lyme disease (
Borrelia burgdorferi
) vector in upper Midwest and New England/mid-Atlantic states; vector of
Babesia microti
in humans and
Anaplasma phagocytophila
in humans and animals primarily in eastern US and upper Midwest.
I pacificus
: Primary Lyme disease vector on the West Coast N/A
RMSF, Rocky Mountain spotted fever; US, United States.
Zoonotic tick-borne diseases
Tick paralysis
Potentially fatal reaction to a paralyzing neuromuscular toxin secreted in the saliva of a female tick late in her feeding. Cattle, sheep, horses, dogs and humans seem to be most affected.
Clinical signs include headache, vomiting, general malaise and loss of motor function and reflexes, followed by paralysis that starts in the lower body and spreads to the rest of the body.
Respiratory failure and death can result. Signs disappear rapidly when the tick is removed, suggesting that the toxin is rapidly excreted or destroyed.
Lyme borreliosis
Agent: Borrelia burgdorferi
Vector: I scapularis (eastern and midwestern United States), I pacificus (western United States)
Species affected: Humans, dogs, horses
Geographic distribution: New England and mid-Atlantic states, upper Midwest and Pacific Coast. Most cases occur in the spring and summer, during nymphal emergence, and in late fall and winter, during adult emergence. Because adult stages are active in cooler months, it is imperative to use year-round preventives for animals and to always do good tick checks on animals and humans regardless of time of year.
Clinical signs: Signs in animals include endocarditis and joint pain; can cause potential fatal kidney disease in dogs. In humans, signs include joint pain, heart disease and neurologic disorders.
Diagnosis: Serology, PCR, physical exam, CBC, serum chemistry, urinalysis
Treatment: Tetracyclines
Rocky Mountain spotted fever
Agent: Rickettsia rickettsii
Vector: Dermacentor variabilis and Rhipicephalus sanguineus (primarily in southwestern United States)
Species affected: Dogs and humans. Cats can seroconvert but there is no evidence of disease in cats.
Geographic distribution: Primarily the eastern United States, where it is the most frequently reported tick-borne disease. Agents other than R rickettsii can lead to spotted fever group disease in humans.
Clinical signs: Flulike symptoms as well as petechial hemorrhage or skin rash and often severe headaches in people. In animals, severe muscle and joint pain, fever, anemia, leukopenia or leukocytosis and often thrombocytopenia.
Diagnosis: Serology, PCR, physical exam, CBC, serum chemistry
Treatment: Tetracyclines
Human granulocytic anaplasmosis
Agent: Anaplasmaphagocytophilum
Vector: I scapularis; can be transmitted by blood transfusion
Species affected: Cats, dogs, horses and humans
Geographic distribution: Throughout the United States and most of the world. Most common in New England, mid-Atlantic states and upper Midwest.
Clinical signs: Dogs: Bleeding presenting as petechial or ecchymotic hemorrhages, depression, lethargy, fever, stiff and swollen joints, lymphadenopathy and leukopenia; less often neurologic disease. Cats: Disease is not well characterized in cats but similar clinical signs as in dogs have been reported. Horses: Lameness, depression, fever, hemorrhage, possible limb edema. Humans: Depression, fever, hemorrhage; signs may be worse with coinfection with Lyme disease or Babesia
Diagnosis: Clinical signs, PCR (acute cases), serology (chronic), CBC to look for leukopenia, blood smear to look for morulae in granulocytes
Treatment: Tetracyclines
Preventing tick-borne diseases in humans and animals
Rather than abstaining from spending time outdoors due to fear of tick-borne diseases, people should instead take some easy preventive measures to minimize disease transmission. These simple measures will substantially help reduce the chances of acquiring a tick-borne disease:
Wear light-colored clothing that has been sprayed with an approved tick repellent.
Walk in the middle of wooded paths. If going into brush or other more common tick habitats, tuck pants into socks.
Be sure to do a thorough tick check on all areas of the body, particularly areas where hair is present.
Keep lawns mowed and remove leaf litter.
For animals, be sure to keep pets on year-round tick preventives and do periodic tick checks.
Cytauxzoonosis
Agent: Cytauxzoon felis
Vector: Amblyomma americanum
Species affected: Cats
Geographic distribution: Mainly found in southeastern United States, but it has been reported from as far north as the Dakotas and New England
Clinical signs: Fever, dehydration, icterus, lymphadenomegaly, hepatosplenomegaly
Diagnosis: PCR, blood smear (negative blood smear does not rule out infection) because in early infection only schizonts are seen in macrophages.
Prevention: Keep cats indoors (and use a prasite preventive).
Treatment: Atovaquone plus azithromycin
Infectious cyclic thrombocytopenia
Agent: Anaplasma platys
Vector: Rhipicephalus sanguineus
Species affected: Dogs; reports of cats and sheep being infected outside United States
Geographic distribution: Worldwide
Clinical signs: Bleeding due to cyclic thrombocytopenia; may be worse with co-infection with canine ehrlichiosis, which is transmitted by the same tick
Diagnosis: clinical signs, PCR (acute cases), serology (chronic). Don't treat seropositive animals that are clinically normal.
Treatment: Tetracyclines
Canine ehrlichoisis
Agent: Ehrlichia canis
Vector: Rhipicephalus sanguineus
Species affected: Dogs
Geographic distribution: Worldwide
Clinical signs: Fever, anorexia, lethargy, thrombocytopenia, lymphadenopathy, edema, bone marrow suppression
Diagnosis: Clinical signs, PCR (acute cases), serology (chronic), CBC to look for leukopenia, blood smear to look for morulae in monocytes
Treatment: Doxycycline
Reference
1. Rosenberg R, Lindsey NP, Fischer M, et al. Vital Signs: Trends in reported vectorborne disease cases-United States and territories, 2005–2016. MMWR Morb Mortal Wkly Rep 2018;67(17):496-501.
Newsletter
From exam room tips to practice management insights, get trusted veterinary news delivered straight to your inbox—subscribe to dvm360.