Surefire methods to control atopy and complicating problems (Proceedings)
Atopic dermatitis, also known as atopy and previously called allergic inhalant dermatitis, is considered to be a genetically based condition whereby the animal develops an IgE antibody response to environmental proteins resulting in disease, most commonly allergic dermatitis.
How to Stay on "Top" of Atopy
Atopic dermatitis, also known as atopy and previously called allergic inhalant dermatitis, is considered to be a genetically based condition whereby the animal develops an IgE antibody response to environmental proteins resulting in disease, most commonly allergic dermatitis. Access of these proteins is perceived to be primarily via absorption through the skin. The proteins are commonly allergens representing pollens of grasses, trees, and weeds, as well as mold spores, house dust, house dust mite antigen, insects and other miscellaneous environmental substances. The incidence of atopic dermatitis in the canine population has been estimated to be between 3% and 15% of the total canine population. Geographic variation is a relevant aspect of the development and presentation of clinical disease. Studies have demonstrated that parasite presence may be a factor encouraging the development of canine atopy. The incidence of atopic dermatitis in dogs may be greater in parts of the country where fleas are more prevalent, as well as increased presence of pollens and other proteins. Other information suggests that viral infections or even vaccination with modified live viral vaccines may augment the production of the specific antibody (IgE) to environmental allergens. The increase in environmental pollutants and indoor allergens has also been postulated as another reason for the increased incidence in the development of atopic dermatitis seen in people. Genetic influence plays an important role in the predilection for this disease and may explain the increased incidence through owner preference for pedigree dogs. In general, atopic dermatitis is a common dermatologic problem observed in the dog. PATHOGENESIS OF CANINE ATOPIC DERMATITIS
The development of canine atopic dermatitis occurs in two stages. The first is considered the sensitization phase of disease development. In this stage, specific proteins (allergens) such as a grass, tree or weed pollen, is absorbed into the skin where a specific cell type (Langerhan's cell) located in the lower part of the epidermis acts as an antigen processing cell and binds the allergen. The allergen then is processed by the Langerhan's cell which migrates from the skin to the regional lymph node where it interacts with T-cells. More specifically, these T-cells are T-helper cells. In addition to the presentation of the allergen protein to the T-helper cells, there is stimulation and proliferation of other memory T-cells and effector T-cells. These T-cells, in turn, interact with B-cells which are used for the production of antibody. During the sensitization stage no disease is observed.
The second stage involves the elicitation of disease. Subsequent exposure to the specific allergen and percutaneous absorption in the sensitized individual, leads to the processing of the allergen by the Langerhan's cell, which again presents the allergen to the immune system already producing specific IgE against the offending allergen. The presentation of the allergen to memory T-helper cells then leads toward the elicitation of cytokines that induce cellular proliferation and IgE production from B-cells (e.g. interleukin 4). The IgE is bound to mast cells and basophils. The mast cells are important in the subsequent development of the clinical signs of the disease through the release of pro-inflammatory mediators. The allergen binds to the specific IgE on the mast cell and the cross-binding of two of the IgE molecules results in this degranulation. Subsequent inflammation is observed as the development of allergic dermatitis and pruritus. Latent reactions may occur as a consequence of the initial immediate reaction.
CLINICAL FEATURES OF CANINE ATOPIC DERMATITIS
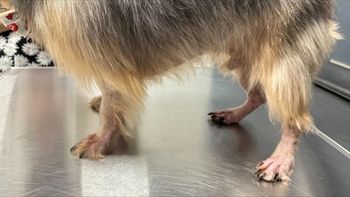
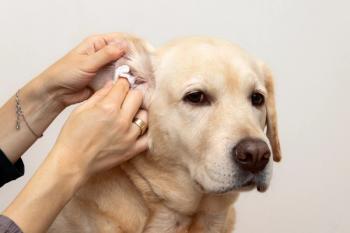
Canine atopic dermatitis is characteristically observed in dogs between six months of age and three years of age where 75% of the animals will initially show the clinical signs. Earlier age of onset has been observed in dogs as young as 2.5 months and dogs have been known to develop symptoms as late as seven years of age. Predominant features of the condition include pruritus affecting the face, legs, feet, ventrum and the ears. Other diseases with similar clinical features include adverse reaction to food (food allergy) and canine scabies. Allergic otitis externa is commonly seen as part of the clinical presentation and is the major primary cause of otitis externa leading to secondary infection in the dog. In addition, ocular changes may also be observed with conjunctivitis, epiphora and possibly secondary complications of infectious conjunctivitis with mucopurulent discharge. Most animals will demonstrate a seasonal pattern before progressing to a non-seasonal (year around) problem. Eventually, as many as 75% will have year around problems. Hair loss is observed through chronic biting, licking, chewing and scratching or by secondary complications.
Early signs of canine atopy are often times not associated with the disease. These may be subtle and have limited evidence of itchiness. Intermittent bacterial infections may be first evidence of the disease presentation. Likewise, ear infections may be signal of underlying canine atopy. Later on more classical symptoms may be observed. Further progression may lead to the complications of secondary infection often characterized by the presence of lesions, such as papules, pustules and macules. Both bacteria (Staphylococcal sp.) and yeast (Malassezia sp.) infections are commonly observed. Evidence of lichenification and hyperpigmentation may be observed in regional areas with chronic dermatitis. Scaling and crusting are common with the development of chronic atopic dermatitis with complications. Occasionally other complications may be seen including demodicosis or dermatophytosis. Secondary ear infections are frequently observed. The clinical features of canine atopic dermatitis with complications may have mimicking features of other conditions. Occasionally, atopy may be observed with pulmonary disease where sneezing or wheezing/coughing may be observed. Coexisting allergic diseases are seen with canine atopy. Flea allergy is observed in flea infested areas in as many as 80% of the cases. Some of the dogs (15-20% ) may also have coexistent adverse reaction to food (food allergy). The diagnosis of canine atopy is made through the historical and clinical examination findings with rule out of other differentials considered.
TREATMENT FOR ATOPIC DERMATITIS
Atopic dermatitis is typically a life-long disease and characteristically intensifies with age showing less responsiveness to commonly used drugs overtime. In addition, the development of complicating problems becomes more prevalent. Practical therapy may be separated into four categories: 1) symptomatic glucocorticoid, anti-histamine and EFA therapy; 2)allergen specific immunotherapy; and 3) immunomodulating therapy with cyclosporine. Avoidance techniques have selected usefulness for flea control as well as dietary restriction in cases with coexisting adverse reaction to food.
Symptomatic Therapy:
Symptomatic therapy includes the use of antihistamines, essential fatty acids and glucocorticoids and topical therapy including shampoos, rinses, leave-on conditioners and sprays. Symptomatic therapy requires no knowledge of specific allergens causing the allergic condition. Antihistamines are often included in the treatment regimen even though their success in atopic dermatitis is often quite limited. A variety of antihistamines have been adapted with dosages for dogs (Table 1). There is no one particular antihistamine with recognition for supremacy to others. Trial periods are necessary to evaluate the effect of specific antihistamines on the clinical condition and also to determine the tolerance in a specific animal. They are ideal from the aspect that adverse reactions are rarely observed. In general, approximately 30% of the cases placed on antihistamine therapy demonstrate a good response.
Essential fatty acids have been investigated and demonstrate considerable benefit in the atopic dog. Those of most benefit include the Omega 3 fatty acids which contain the chemical eicosapentanoic acid (EPA) usually in combination with docosahexanoic acid (DHA). Omega 3 fatty acids are commonly derived from fish oil or some plant sources. They may have a limited antipruritic effect but are beneficial because of negligible adverse reactions. Integration with antihistamine therapy may produce an enhanced effect. The dosage of eicosapentanoic acid commonly used is approximately 40 mg/kg/day. A variety of commercial products are available.
Glucocorticoid Therapy:
Glucocorticoids are a group of steroid compounds that are also used in the treatment of atopic dermatitis as an anti-inflammatory compound. Glucocorticoid therapy is best used in a restricted manner with administration of the least amount necessary to control clinical signs. While injectable steroids are commonly used in practice, the ideal treatment regimen includes the use of short acting, low potency oral steroids that are typically administered on an alternate day basis for maintenance therapy. The commonly used products are prednisone, prednisolone, and methylprednisolone . Triamcinolone has also been used with modification of the maintenance regimen to every third day administration because of its intermediate duration of effect.
Topical Therapy:
Topical therapy is quite helpful in treating the atopic animal. It not only provides an antipruritic affect, it concurrently assists in the removal of surface allergen on the skin before percutaneous absorption may take place. Shampoos are commonly integrated in this treatment approach. They may contain oatmeal, aloe vera, or other antipruritic chemicals such as pramoxine, diphenhydramine, hydrocortisone or triamcinolone. Shampoo therapy is unfortunately limited due to the removal of the product in the rinsing phase of the bath. Rinses and leave-on conditioners or sprays may be more effective because they provide a residual effect. These products may contain colloidal oatmeal, antipruritic chemicals such analgesics, an antihistamine or glucocorticoids. Their attribute is toward decreasing the need for systemic therapy specifically avoiding increased dependency of glucorticoids. Topical therapy also enhances the targeting of specific regions of pruritus without systemic therapy.
Allergen Specific Immunotherapy:
Allergen specific immunotherapy (ASIT) is commonly known as hyposensitization treatment. The method includes the administration by parenteral therapy using the same proteins to which the animal has known allergic reactivity. The presentation of that protein in an unnatural way circumvents the percutaneous absorption thereby eliciting a different immune effect. This effect results in a down regulation ultimately resulting in less of the IgE antibody and thereby decreased clinical signs. The therapeutic effect of this technique is variable and quite dependent upon the extent and accuracy of identifying specific allergens that are problematic to the given animal. In general, 60-70% of the dogs treated with allergen immunotherapy should demonstrate good to excellent response. These animals classically require integration of antihistamines, essential fatty acids and occasionally glucocorticoid therapy in combination with topical management. Overall, the beneficial effect is significant in those responders making it a very beneficial treatment. This therapy, however, requires identification of offensive allergens causing disease in the respective animal. Treatment is ongoing and is commonly required for the life time of the animal. Allergy testing includes both intradermal testing (IDT) and serum allergy testing (SAT).
Allergy Testing:
Allergy testing is limited to the identification of specific allergens with the anticipation of utilizing this information for allergen immunotherapy. Allergy testing is not used for diagnostic purposes as some normal dogs may show intradermal test reactivity while some atopic dogs may not show reactions to specific testing. There are two types of tests that are utilized. The intradermal test (IDT) is a common diagnostic tool utilized for the assessment of regionally known allergens predominantly by specialists. This technique requires selection and maintenance of allergens which may restrict the application to many practices. Interpretation of the allergy test results need correlation with the historical features of the disease, particularly in reference to seasonal episodes of symptoms. A percentage of animals fail to reveal positive reactivity through intradermal testing, often as a consequence of previous drug therapy, such as antihistamines or glucocorticoids. Usually 40-70 allergens are tested in this investigation. Intradermal testing remains the gold standard for allergen identification. False negative reactions are usually the limitation of this procedure as well as the need for drug withdrawal, sedation, and hair removal to perform the procedure.
Serum allergy testing (SAT) has become more popular over time with reputable laboratories providing service for identification of circulating anti-allergen IgE. Different techniques are used by various laboratories and may affect the results. Selection of allergens respective to a given geography may be quite different from one laboratory to another. Selection of a laboratory should be influenced by the array of allergens used in their respective profile. Some laboratories test allergens in groups rather than singly with limited usefulness for the development of the allergen solution for therapy. Serum allergy tests may have problems with false positive and false negative findings.
The development of the allergen solution for use as therapy is based upon the results of either a serum allergy test, intradermal allergy test or the combination of both. The considerations for allergy testing include the tentative diagnosis of atopy through the historical and clinical signs. This treatment is also recommended for animals whose season of itchiness exceeds three months out of the year. It is also ideal to submit candidates for allergen immunotherapy at or after one year of age although allergen immunotherapy has been used in younger dogs due to the severity of their problems and after rule out of other diseases. The prospect of immunotherapy is the only reason for considering allergy testing. Cost factors may be an issue for the respective pet owner as well as the personality of animal with regard to acceptance of the injection therapy. Allergen immunotherapy is restricted to parenteral administration, conventionally by subcutaneous injection. Due to the excellent safety of this treatment, it is usually administered at home by the pet owner. Oral therapy is being developed for humans but has not been perfected for veterinary administrationThe injection schedule is somewhat variable depending upon the laboratory or dermatologist preparing the allergen solution, but classically starts with a dilute solution or two dilute solutions before reaching the more concentrated maintenance vial. The initial injections are given in increasing amounts and progresses from the least concentrated to the most concentrated vials. Rapid administration of the induction phase of allergen immunotherapy has been developed providing the full induction provided in a 6-8 hours in contrast to 30-40 days. This is known as RUSH allergen immunotherapy. This method requires close observation and preparedness for an allergic emergency although this is unlikely to happen. Maintenance therapy is administered at a dosage and frequency dependent upon the individual response or tolerance of the treatment. Animals administered small amounts more often may respond better than larger amounts with less frequent administration. Injections once weekly or every two weeks or some at a three week interval are also utilized. Decreasing the quantity of allergen administered is necessary when administering more frequently. Animals under 10 kg should be restricted to 0.5 ml. or less at the maximum maintenance dose. Selected animals may require more dilute solution to avoid increased pruritus from the allergen therapy. Modification of the dosage schedules may enhance the response in many cases. Weekly injections of 0.35-0.5 ml of maintenance solution may be preferable to 1.0 ml every 21 days. Injections administered every two weeks may require 0.4 - 0.6 ml and some animals may respond best to a small amount twice weekly (0.15-0.3 ml).
ASIT requires a significant period of time to observe response. This may take as long as 5-7 months but is typically seen between 3-5 months. The attributes of allergen immunotherapy include the development of long term control decreasing the need for adjunctive therapy, in particular glucocorticoids. Complete desensitization has been observed in rare situations. In general, it is perceived that allergen specific immunotherapy has a better chance of being effective if started early in the disease progression. It has become the mainstay of treatment alternatives with its appealing response rate. It does not, however, eliminate the need for adjunctive therapy in most cases but decreases the intensity of concurrent medication. Allergen specific immunotherapy is not utilized for the treatment of flea allergy where aggressive and persistent flea control is advised. Likewise, dietary allergy is controlled exclusively through the process of avoidance with limited ingredient diets or hypoallergenic diets. Failure to respond to specific allergen immunotherapy may be relevant to coexisting problems that have not been identified and treated. These may include dietary allergy, canine scabies or complicating infections such as bacterial pyoderma, cutaneous malassezia, dermatophytosis, or demodicosis. Incomplete recognition of offensive allergens may require repeat allergy testing to identify other allergens that may be problematic in a given animal. Inconsistent treatment or treatment regimens that are not optimal may also lead toward failure. The duration of treatment necessary for full assessment would require a full year. Non-responders may represent as many as 25-35% of the animals placed on therapy. Dogs with a large number of allergen reactions may be good responders and should not be perceived as non-candidates for treatment with allergen. Some of the better responders are dogs that have >20-30 allergens identified in their profile. The maximum number of allergens included in a single vial is limited and ranges from 10-17 depending on the individual preparing the solution. Animals with larger number of reactions are often placed on multiple vials to include the relevant allergens but remain within the maximum per vial number of allergens.
Modification of immunotherapy should be integrated with intermittent evaluations and modification of the treatment interval and the volume of allergen administered. Integrated adjunctive therapy should be utilized as part of the maintenance regimen. Repetitive bathing with ongoing parasiticidal treatment is also necessary.
Specific Immune-modulating Therapy - Cyclosporine A
Cyclosporine A (CsA) (Atopica®, Novartis Animal Health) is a chemical that is used in the treatment of humans after receiving organ transplantation. It is a potent immunosuppressant compound that specifically affects the portion of the immune system in which the pathology of atopic dermatitis occurs including the TH2 cells. Cyclosporine is a polypeptide product from a fungus Tolypoladium inflatum. The immunological effects include inhibition of lymphocytes, in particular T-helper lymphocytes. It depresses induction of cytotoxic T-lymphocytes and exhibits suppression of IL-1 & IL-2, macrophage activating factor & gamma interferon. T-lymphocyte proliferation is blocked while there is less effect on B-lymphocytes
As many as 65-70% of atopic dogs treated with CsA may demonstrate appreciable control. CsA is also used in the cat. Typically the drug is administered daily for 30 days then modified to alternate day treatment for the next month with maintenance therapy based upon clinical response and attempt to reduce to the lowest amount necessary to control the clinical signs (e.g. 3 days per week). The dosage is critical for optimal response and should be close to 5 mg/kg/d. Reduced dosage has been achieved with successful response in dogs by integrating ketoconazole at 2.5 mg/kg/day which interferes with the excretory pathway of the CsA. The limitations of this therapy include the cost and adverse effects most often representing Gl problems (vomiting and/or diarrhea). Cyclosporine A is used in selective cases typically representing those demonstrating difficult control.
SUMMARY
Atopic dermatitis is common cause of skin disease in the dog particularly in geographic areas with high parasite and allergen exposure. Other conditions need to be evaluated with observation of complicating problems to achieve ultimate success. Diagnosis is based on history, clinical signs, and elimination of other diseases while allergy testing is used predominantly for the identification of allergens to include in the allergen specific immunotherapy. Feline atopy appears to be more common than previously recognized and has options for diagnosis and treatment.