Physical rehabilitation: Improving the outcome in dogs with orthopedic problems
After an orthopedic procedure, it is common to have a convalescent period of weeks to months before recovery is attained. Physical rehabilitation may help patients achieve maximum recovery. Physical therapy is also valuable for easing chronic pain in pets.
Advances in small-animal medicine and surgery have led to an improved and sophisticated level of healthcare for pets. Patients with problems that were once considered untreatable can now be evaluated by specialists in a variety of disciplines. For example, in patients with orthopedic problems, diagnostic and treatment options have widely expanded. Orthopedic surgery is unique in that the corrective procedure is completed rapidly relative to the patient's recovery. After an orthopedic procedure, it is common to have a convalescent period of weeks to months before recovery is attained. Physical rehabilitation may help patients achieve maximum recovery. Physical therapy is also valuable for easing chronic pain in pets.
Physical therapy has become more common is small-animal patients, in part, because of its benefits in people. Clients are aware of these benefits because of the importance and ubiquity of physical therapy in human medicine. Many protocols in human physical therapy have been developed by using animal models. Likewise, techniques used in human physical therapy are being adapted for use in small and large animals. As information concerning physical rehabilitation increases in the veterinary literature, additional techniques will be incorporated in veterinary practices to improve the standard of care.
In this article, we introduce a variety of physical rehabilitation modalities available to small-animal practitioners, including their most common indications and their benefits. The benefits of physical rehabilitation are multifaceted, and some may not be intuitive. Depending on the modality used, benefits include pain relief, decreased inflammation and swelling, increased tissue extensibility and flexibility, strengthening, improved balance and proprioception, mobilization of tissues, improved limb and joint biomechanics, improved weightbearing, psychological benefits, weight loss, and improved cardiovascular and respiratory fitness.1-4
POSTOPERATIVE REHABILITATION
Analgesics
Postoperative rehabilitation begins with aggressive analgesia before anesthetic recovery to reduce peripheral and central nervous system sensitization to pain.5-9 Since pain is one of the primary factors limiting mobility, it is paramount that it be eliminated or minimized. Optimal pain relief encourages early mobilization of an affected limb. Untreated pain leads to an increased metabolic rate, cardiovascular stress, impaired immunity, central and peripheral hyperalgesia, pulmonary dysfunction, and guarding of the limb with the joints in a flexed position, a condition referred to as reflex inhibition.8,10
Nonsteroidal anti-inflammatory drugs (NSAIDs) that spare the cyclooxygenase-1 (COX-1) enzyme but inhibit the cyclooxygenase-2 (COX-2) enzyme, such as deracoxib and carprofen, significantly reduce the production of prostaglandins and inflammation associated with injury or surgical trauma.6 Other NSAIDs, such as tepoxalin, etodolac, and meloxicam, are also good anti-inflammatory agents but are not approved for administration before surgery in dogs. They may be given postoperatively if there is no danger of continued hemorrhage or to manage chronic pain. However, different NSAIDs should be not be given concurrently, and an appropriate washout period is necessary when changing NSAIDs. Avoid drugs that selectively inhibit the COX-1 enzyme, such as aspirin, in the perioperative period because they can inhibit platelet function and contribute to intraoperative hemorrhage.11,12
Other medications that may be used alone or in combination with NSAIDs for analgesia in dogs include acetaminophen, codeine (either alone or in combination with acetaminophen), and tramadol. An opioid narcotic, such as buprenorphine, morphine, hydromorphone, or oxymorphone, should also be used to provide multimodal analgesia, which is more effective for pain control than a single agent used alone.13 Ketamine blocks N-methyl-D-aspartate (NMDA) receptors that are at least partly responsible for the wind-up effect of an uncontrolled pain stimulus and may be combined with NSAIDs and opioid drugs in the immediate postoperative period for additional analgesia.7,14,15 Lidocaine may be used as a constant-rate infusion to decrease the amount of narcotics needed for pain control.14 Lidocaine can be combined with ketamine or an opioid, such as fentanyl or morphine, and be given as a constant-rate infusion after trauma, intraoperatively, or postoperatively to combat pain. Epidurals and regional and local nerve blocks should be used when appropriate to further alleviate pain. Intra-articular injections of bupivacaine or lidocaine administered before surgery and again at the end of surgery also provide analgesia.16
Analgesics should be continued through the postoperative period and should include opioids and NSAIDs along with physical therapy for pain relief. Physical rehabilitation is an effective adjunct to traditional anti-inflammatory and analgesic medications. In fact, physical rehabilitation can lower the dose or frequency of medication needed to control pain.2,4,13
Superficial thermal modalities
Cryotherapy
Ice compresses provide an excellent method to help control pain and inflammation in the immediate postoperative period. Not only is cryotherapy beneficial in the acute phase of tissue injury and inflammation, it is also advantageous after exercise and throughout rehabilitation when inflammation occurs. The effects of cryotherapy include vasoconstriction, decreased blood flow, reduced cellular metabolism and permeability, attenuation of traumatic or exercise-induced edema, and decreased muscle spasm.17,18 Another primary effect of cryotherapy is analgesia, which is thought to be a result of decreased sensory and motor nerve conduction velocity that occurs when nerve fibers are cooled.19,20
Cryotherapy can be accomplished with a variety of methods. The simplest way is by placing crushed ice in a sealed plastic bag and then wrapping the bag in a thin cloth, such as a pillowcase or towel. Alternatively, you can prepare a mixture consisting of two parts water and one part alcohol in a double-sealed plastic bag and place it in a freezer. The resulting pack is a frozen slush that conforms to any surface. Apply the cold pack for 15 to 20 minutes immediately after surgery while the patient is still recovering from anesthesia. Be careful when applying cold packs to patients that are already hypothermic postoperatively. Use cryotherapy for the first three or four days after surgery to help minimize inflammation, swelling, and pain from surgery. Apply the cold compress for 15 to 30 minutes three or four times a day.21,22 Monitor the patient for discomfort, and assess the tissues periodically for signs of adverse effects such as white or pale areas. Do not use cryotherapy in patients with poor or absent pain sensation.
Cryotherapy results in significant reductions in intra-articular temperatures of peripheral joints. After 15 minutes of ice application to the canine stifle, the temperature inside the joint can drop 7.4 F (4.1 C). Immersion in ice water can produce a more marked decrease in stifle joint temperatures (36.4 F [20.2 C]) but may produce decreases in rectal temperatures.22 Temperature changes vary depending on the type and depth of tissues cooled.21,23 In one study, ice packs applied to dogs' thighs for 20 minutes resulted in a precipitous drop in temperature of tissues up to a depth of 1 cm, but minimal cooling occurred at tissue depths of 3 cm. However, the tissue temperature remained below normal for 100 minutes.24
Heat therapy
Apply heat to tissues only after the acute phase of inflammation is complete, generally three to five days after surgery or injury. Commercially available hot packs are generally used for heat therapy and may be heated in a microwave until they are warm to the touch. Alternatively, you can make a microwavable hot pack by placing rice in a sock and knotting it closed. Test that the pack is not too hot by placing it on the back of your neck. Use a blanket or towel as an insulating layer between the patient's skin and the heat source to prevent burns. Therapeutic ultrasound also effectively heats tissues up to 5 cm deep.
Superficial heat causes vasodilation, which improves circulation to the superficial tissues, increases tissue oxygenation and transportation of metabolites, and increases the rate of enzymatic and biochemical reactions to facilitate tissue healing.23,25,26 Heating soft tissues before stretching allows for greater extensibility of collagenous tissues. Maximum deformation occurs when tissue temperatures are maintained at 104 to 113 F (40 to 45 C) for a maximum of five to 10 minutes while applying a stretch force.26 Joint stiffness can be reduced and range of motion can be improved immediately after heat is applied.27 Do not apply heat in the early inflammatory phase of healing because swelling and edema may increase and result in further tissue damage.
Range of motion and stretching exercises
Range of motion and stretching exercises are vital activities to help improve joint motion and flexibility in pets after surgery or in patients with chronic orthopedic conditions. These exercises help prevent adhesions between soft tissues and bone, improve muscle extensibility, and prevent further injury to joints, ligaments, tendons, and muscles. True passive range of motion exercise is performed without muscle contraction and is facilitated by a therapist. Complete relaxation is rare in veterinary patients, so most range of motion exercises are active-assisted.
Applying steady pressure for 15 to 30 seconds at the end of flexion and extension results in stretching (Figure 1). Range of motion and stretching exercises are often performed together to help maintain and improve range of motion that is often limited by the soft tissues. It is critical that you do not exceed a range of motion that is comfortable for the patient. If pain is inflicted, active use of the limb and joint may be reduced. Use analgesics to maximize comfort. Keep in mind that when patients are nonambulatory, both the injured area and the other portions of the body become less extensible and can create secondary problems. Be careful to not focus on only one region but consider the entire patient. Additional benefits from range of motion and stretching exercises are pain reduction, enhanced blood and lymphatic flow, and improved synovial fluid production and diffusion of nutrients.25
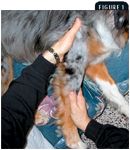
Figure 1. A range of motion exercise of a dog's elbow. While holding the humerus stationary and in a neutral position to isolate the elbow joint, slowly flex and then extend the elbow.
When performing range of motion exercises, make sure to have the patient in a quiet environment with little external stimuli. Use adequate support and padding to ensure patient comfort. Lightly stroke and massage the limb to be manipulated for a few minutes before range of motion exercise. The joint motion should be smooth and controlled, with steady motion through a comfortable range of extension and flexion. Ideally, the range of motion should involve only one joint at a time while the other joints assume a neutral position. The excursive movements should start small and increase until the endpoint of the range of motion is reached and the patient appears to slightly resist, indicated by tensing its limb muscles or turning its head toward the therapist to indicate early discomfort.
As patient comfort allows, encourage incremental increases in range of motion. With repeated range of motion sessions combined with some stretching at the end of motion, gradual increases in joint excursion may be expected over the course of several days to weeks. If much joint capsule fibrosis is present, however, the gains in motion may be less pronounced. Fifteen to 20 repetitions performed two to four times a day is likely sufficient. If you use true stretching, take the joint slightly beyond comfortable flexion, and hold it for at least 15 to 30 seconds. Then take the joint slightly beyond comfortable extension, and hold it for at least 15 to 30 seconds.
Special cases, such as articular fractures, physeal fractures, joint contractures, and immobilized joints, may require adaptations to routine stretching and range of motion protocols. Motions can graduate to a bicycling motion that can simulate or exaggerate a functional range of motion of all joints simultaneously in a limb. You can objectively assess improved range of motion by using a goniometer; be sure to record the angle measurements in the medical record. The unaffected contralateral limb can often be used as a reference. Improvements achieved with range of motion exercises will be slow and gradual. Safety is important, and it is recommended to have a handler restrain the patient during the initial sessions.
Therapeutic exercises
Therapeutic exercises are some of the most beneficial activities in a physical rehabilitation program.2-4,28-31 The degree of activity allowed depends on the surgical procedure performed, the condition of the tissues involved, and the stage of tissue healing.32 Relatively slow and low-impact exercises are initiated early in the postoperative period, and as limb use and patient comfort allow, more advanced exercises should be instituted. In all cases, the stage of healing and the strength of tissues must be considered so that excessive forces are not placed on healing tissues, causing tissue damage.
Common activities include assisted standing or walking, controlled leash exercises, treadmill walking, dancing, and wheelbarrowing, as well as sit-to-stand activities and stair climbing. Jogging, stepping over rails, pulling or carrying weights, playing ball, and exercising with therapy balls are also used.32 If patients are reluctant to use an injured leg, a syringe cap, coin, or marble can be taped to the bottom of the contralateral unaffected limb to help encourage use of the injured limb. Only use this stimulus intermittently because dogs will quickly become desensitized to its presence.
Assisted standing or walking
The ability to perform many of these activities depends on the patient's having adequate strength and flexibility to participate. These exercises are used if the patient is ambulatory or at least able to bear some weight. Patients that may not be able to stand or support their own weight may benefit from assisted standing. Even short periods of standing provide an opportunity to build strength; aid in proprioceptive training; improve circulation, respiration, and elimination efforts; and enhance a patient's psychological well-being.32 Short-term assisted standing and walking can be facilitated by using body slings or towels (Figure 2). The initial goals for walking should be to complete 10 to 15 steps per limb. Allow the patient to rest periodically, if necessary. Repeat this activity two to four times a day or as often as the patient is able. Some patients may progress rapidly. Dogs with conditions such as severe spinal cord injury may require more gradual increments of activity. In these cases, increasing activity 15% to 25% each week may be appropriate. Two- and four-wheel carts are available for extended rehabilitation efforts in patients with severe limitations. Carts are particularly helpful in patients with neurologic disease that have prolonged paresis.
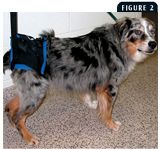
Figure 2. Towel or sling support is beneficial for a patient with a limited ability to stand and support its own body weight.
Exercising with therapy balls
Exercise balls or rolls come in various sizes and can be partially deflated to provide added stability and contour to an animal's body shape and size. These devices can be used for assisted standing exercises or to challenge the patient with various weight-shifting and weightbearing tasks. The exercise rolls are peanut-shaped and provide better lateral stability (Figure 3); they are ideal for larger dogs because patients are physically supported. Exercise balls are excellent for general stretching and to challenge patients' proprioceptive abilities by rolling the ball back and forth. Like most therapy sessions, exercises using therapy balls should be limited to 10 to 15 minutes or less depending on the patient's attention span and endurance. When straddling the ball, the animal should be able to touch the ground with all four feet. Weight and proprioception can be shifted to the hindlimbs by elevating the forelimbs and vice versa. Small movements of the ball challenge proprioception and encourage limb use. Slow movements and patient manipulation also encourage joint motion. Patients may initially be placed on the ball for two to five minutes; as strength and stamina improve, the length of time may be increased.

Figure 3. A peanut-shaped ball (e.g. PhysioRoll-Gymnic) may be used to challenge proprioceptive abilities or increase weightbearing on the forelimbs or hindlimbs.
Controlled leash walks
The main exercise for most patients in the early rehabilitation period is slow, short, controlled leash walks in which the patient is encouraged to achieve the most normal gait possible and use the affected limb to the best of its ability. Unfortunately, this exercise is often performed incorrectly; if a patient is led too quickly, the pet tends to skip with the affected limb or not use the limb at all. Slow walks increase stance time, flexibility, strength, and weightbearing. When an animal has mastered the slow walk, faster walks can further develop endurance, strength, balance, coordination, and proprioception.32
Walking inclines provides a low-impact method to strengthen the gluteal muscles as well as the cranial and caudal thigh muscles. The handler should be able to control the patient's head and may want to have it slightly raised to transfer additional weight to the hindlimbs or slightly lowered to transfer weight to the forelimbs, depending on the desired effect. It is best to start with small inclines and progress as the patient is able. Declines are also beneficial for forelimb muscle strengthening and limb use. Walking downhill may also result in increased hock, stifle, and hip flexion during the stance phase of gait because the limbs are advanced further cranially under the body as the dog walks downhill.32 Although walking results in some joint motion, the joints do not undergo their maximum range of motion.33
Treadmill walking
Most dogs that are accustomed to walking on a leash readily take to treadmill walking with minimal training (Figure 4). The front of the treadmill should face toward the center of the room or a hallway. A person standing in front of the treadmill with treats or words of encouragement often helps with patient compliance. Start the patient on a stationary treadmill, and slowly increase the velocity to the desired setting. Treadmills for dogs are available, but many of the models used by people can be modified for dogs by adding an overhead bar with a support system that can attach to a harness. Harnesses help support the dog in case it stumbles or falls. Variable incline and speed controls are also useful. Joint range of motion is similar in dogs walking on a treadmill or over ground. Normal dogs tend to have an increased stance time and shorter stride length while walking on a treadmill compared with walking on ground.34 Further studies are needed to determine whether patients, particularly those with osteoarthritis, benefit from these alterations in gait. Walking on a ground or underwater treadmill is an unnatural experience for dogs and challenges their balance, proprioception, and coordination. Most animals are more likely to use an affected limb on a treadmill. Inclined treadmill activity may offer additional strength training.

Figure 4. Walking on a treadmill encourages early limb use after surgery and challenges proprioception. A harness can be used for support if needed.
Dancing
Dancing exercises allow additional weight transfer to the patient's hindlimbs. This activity increases weightbearing and challenges balance, coordination, and proprioception. Hip extension is greater with dancing backward as compared with dancing forward, and stance time is slightly increased with dancing. Assess a patient's range of motion before dancing so that a comfortable range of motion is not exceeded. The patient should be consistently using the affected limb at a walk before graduating to dancing. Muzzle the patient during initial sessions for handler safety.35
Wheelbarrowing
Another form of therapeutic exercise, wheelbarrowing, focuses on using the forelimbs. Place your hands under the dog's caudal abdomen and gently lift the dog's hindquarters off the ground a few inches while the dog walks forward. Lifting the animal higher does not seem to increase the peak force placed on the forelimbs. This is likely because of the decreased stride length when wheelbarrowing and the partial hindquarter support. While shoulder extension is increased with wheelbarrowing, the extension and flexion of the other joints are less than achieved with walking.35
Jogging
Jogging may be initiated when weightbearing improves and there is decreasing lameness at a walk. Initially, patients may jog for 30 to 60 seconds two to four times a day. The amount of jogging may be increased 10% to 15% per week as long as lameness does not worsen.
Stepping over rails
Stepping over cavaletti rails and walking in snow, sand, or tall grass increase active range of motion, strengthen muscles, and improve endurance (Figure 5). Cavaletti rails are horizontal poles that are raised off the ground. The orientation, height, and speed of the course can be modified to suit a patient's needs.

Figure 5. Cavaletti rails help improve active range of motion of all joints as a dog negotiates the obstacles. Stride patterns can be altered by placing the rails closer or farther apart.
Pulling or carrying weights
To enhance muscle strength, you can fit patients with a harness to pull weighted sleds to increase power and muscle tone. The amount of weight will vary depending on the animal's size and the design of the sled and harness. Initially, use only light weights. The animal's gait should change only slightly so that the sled is easily pulled over the desired distance. Heavier weights can be added after technique, strength, and endurance have been mastered with lighter weights. Similarly, strap-on weights may be placed on the affected limb to improve muscle strength and stamina. Weights are generally used two or three times a week. Again, it is important that the tissues subjected to increased forces be at the later stages of tissue healing, and patients should experience no pain or lameness after exercise.
Aquatic therapy
Aquatic exercise has many therapeutic benefits in people, and similar benefits have been demonstrated in small-animal orthopedic and neurologic patients (Figure 6).36-39 Buoyancy, hydrostatic pressure, viscosity, resistance, and surface tension are all important physical properties of water to consider when designing an aquatic rehabilitation program; each of these offers specific benefits.40 Buoyancy decreases the amount of weight placed on arthritic joints.41,42 Hydrostatic pressure provides constant pressure to a body or limb submerged in water at a given depth and increases as the depth of the water increases. This pressure may aid venous and lymphatic drainage from an edematous distal limb or swollen joint.41,42 Hydrostatic pressure may also decrease pain by providing a phasic stimulus to the sensory receptors to decrease pain perception. The viscosity of water provides resistance to movement. This resistance may help strengthen muscles and promote cardiovascular fitness. Viscosity may also increase the patient's proprioception underwater and help prevent falling by allowing more time for a patient to correct an error in balance.42
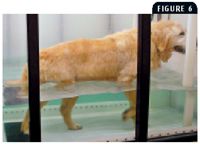
Figure 6. This patient demonstrates increased active flexion of the elbow and carpus while walking on an underwater treadmill.
Surface tension becomes an important factor to overcome if motion occurs at the surface of the water. A joint undergoes increased motion and work to break through the water's surface. In general, activities or motions that occur below or above the surface are easier than those occurring at the surface.32,43 The degree of resistance and buoyancy can be adjusted by changing the water depth. Surface tension is constant regardless of water depth but can be manipulated by changing the water level to the level of specific joints. Joint motion is altered as the height of the water changes because of the force necessary to break through the surface.
The collective benefits of aquatic exercises include assisted weightbearing; improved strength and endurance, cardiovascular fitness, range of motion, agility, balance, and proprioception; as well as decreased joint effusion and peripheral edema.38,42,44,45 Be sure to monitor the patient closely and ensure its safety. Floatation devices may be used, and a handler should be with the patient at all times. A patient that tires suddenly or experiences acute anxiety may require immediate attention.
Water temperature may also affect the cardiovascular response to exercise. Peripheral vasoconstriction occurs in people when they are submerged in cool water. Blood moves centrally, enhancing venous return, which results in increased stroke volume and decreased heart rate, increasing exercise efficiency.46 Blood pressure decreases slightly as well when working in cooler water. Because of these physiological effects of water temperature, it has been recommended that whirlpools and underwater treadmills be kept in the range of 78.8 to 82.4 F (26 to 28 C) to prevent heat-related complications.32 People who exercise in water that exceeds body temperature have higher cardiovascular demands that result in increased blood pressure47; this may hold true for dogs as well. One study suggests that slightly warmer water temperatures ranging from 86 to 94 F (30 to 34.4 C) had negligible influence on heart rate, respiratory rate, and rectal temperature.48
It is recommended to wait until after suture removal in an uncomplicated wound or incision before beginning aquatic therapy. Some clinicians believe that it is only necessary to wait until the wound is sealed by fibrin. The cleanliness of the water, urgency of the therapy, availability, and the patient's overall health may be factors to consider when determining when to initiate aquatic therapy. In conditions that necessitate early aquatic therapy before the wound is sealed, surgical sites can be temporarily covered and protected with water-resistant bandages, dressings, or wound sealants.
Neuromuscular electrical stimulation
NMES is a common modality used in physical rehabilitation. Most NMES units use surface electrodes to excite nerves, which in turn, stimulate muscles to contract. The depolarization of the motor nerve results in skeletal muscle contraction. Three types of currents are commonly used: continuous direct, continuous alternating, and pulsed currents. Most NMES devices are pulsed current, which consists of unidirectional or bidirectional flow of DC or AC electrical current that stops for brief periods. NMES is used in a variety of orthopedic and neurologic conditions, including cranial cruciate ligament pathology, fractures, and spinal cord trauma.49 The benefits of NMES include increased joint mobility, decreased joint contracture, decreased edema, improved circulation, improved muscle strength, and pain relief.2,32,50,51 Patients that should not receive electrical stimulation are those with pacemakers or seizure disorders. It should also not be used over a carotid sinus, a gravid uterus, or areas of thrombosis or neoplasia.
Therapeutic ultrasound
Therapeutic ultrasound is a deep tissue heating modality that may be an effective adjunct when rehabilitating musculoskeletal conditions such as restricted range of motion resulting from joint contracture, pain, and muscle spasm. It also appears to be helpful in stimulating tissue healing at lower intensities. The degree of heat production and penetration depends on the intensity, frequency, and duration of ultrasound and the size of the treatment area. The tissue type being treated is also an important factor. High collagen content tissues (bone, cartilage, and tendons) are affected more than those with less collagen (fat, blood vessels, and muscles).
The temperature of the tissues being treated can be raised 1 to 4 C (1.8 to 7.2 F) through the use of ultrasound. Some treatment protocols have been extrapolated from experimental studies done in people.52-54 One study that looked at the effects of various ultrasound treatments on caudal thigh musculature in dogs showed significant heating during 3.3 MHz ultrasound.26 Another study demonstrated a significant increase in hock flexion and tissue heating with 10 minutes of continuous ultrasound at 1.5 W/cm2 applied to the calcanean tendon.27 The effects were transient and suggest a need to apply other stretching and range of motion exercises immediately after heating. The skin over the target tissue must be clipped so that the ultrasound waves are not attenuated.55
PHYSICAL REHABILITATION FOR ARTHRITIC PATIENTS
Osteoarthritis is the most common cause of chronic pain in dogs, affecting about 20% of the canine population, or 10 to 12 million dogs in the United States.56,57 Sadly, more than half of these animals go untreated. Management of osteoarthritis must be viewed as a lifelong commitment. NSAIDs, used consistently, have markedly decreased the degree of discomfort associated with this debilitating disease.6,58-61 Drug therapy is the cornerstone of pain control. Because of the chronic nature of the disease, however, other interventions such as slow-acting disease-modifying agents, weight reduction, modified exercise programs, and physical rehabilitation should be incorporated into the treatment plan.4,62,63 You can think of the pharmaceutical therapy as an adjunct and a means by which a patient can undergo physical rehabilitation to ultimately reduce the amount and frequency of medication needed to maintain a comfortable lifestyle. NSAIDs alone can provide pain relief, but by themselves, they do not directly increase range of motion, muscle mass, or improve synovial fluid production and turnover. Improvements in these factors can be met through exercise and physical rehabilitation.
Keep in mind that older animals are often afflicted with other systemic conditions that may limit the amount or duration of medications they can tolerate.64-68 These patients require a thorough medical workup, including a complete blood count and serum chemistry profile and complete radiographic, physical, neurologic, and orthopedic examinations. Concurrent medical conditions must be treated to ensure the optimal benefits from physical rehabilitation.
Surgical options to treat, prevent, or delay the onset of osteoarthritis include stifle stabilization for cranial cruciate ligament rupture, surgery to correct patellar luxation surgery, triple pelvic osteotomy, joint arthrodesis, femoral head and neck ostectomy, and removal of a fragmented coronoid process, ununited anconeal process, or osteochondritis dissecans lesion. Physical rehabilitation modalities that often benefit arthritic patients include aquatic exercises; ground treadmill exercise; walking on level, incline, and decline surfaces; jogging; neuromuscular electrical stimulation (NMES); and therapeutic ultrasound; as well as massage and other modalities.
CONCLUSION
A wealth of information exists regarding physical rehabilitation in people, and more information is becoming available regarding its application in small-animal patients. It is important to be well-versed in the various modalities, the benefits associated with each and their indications and contraindications. Tailor rehabilitation programs to the individual because the severity of the condition varies in each patient. Many of the major cities in the United States have physical rehabilitation centers for pets. These facilities work closely with referring veterinarians to design and implement programs appropriate for each patient and its condition. It is not difficult to develop a rehabilitation program as a new service within a clinic or hospital. Therapeutic exercises require little financial investment and equipment. Like all disciplines in medicine and surgery, it is important to have proper training before beginning a rehabilitation program.
Greg Arnold, DVM
Darryl L. Millis, MS, DVM, DACVS
Department of Small Animal Clinical Sciences
College of Veterinary Medicine
The University of Tennessee
Knoxville, TN 37996
REFERENCES
1. Johnson JM, Johnson AL, Pijanowski GJ, et al. Rehabilitation of dogs with surgically treated cranial cruciate ligament-deficient stifles by use of electrical stimulation of muscles. Am J Vet Res 1997;58:1473-1478.
2. Taylor RA. Postsurgical physical therapy: the missing link. Compend Contin Educ Pract Vet 1992;14:1583-1594.
3. Simkin PA, Huang A, Benedict RS. Effects of exercise on blood flow to canine articular tissues. J Orthop Res 1990;8:297-303.
4. Millis DL, Levine D. The role of exercise and physical modalities in the treatment of osteoarthritis. Vet Clin North Am Small Anim Pract 1997;27:913-930.
5. Crandell DE, Mathews KA, Dyson DH. Effect of meloxicam and carprofen on renal function when administered to healthy dogs prior to anesthesia and painful stimulation. Am J Vet Res 2004;65:1384-1390.
6. Millis DL, Weigel JP, Moyers T, et al. Effect of deracoxib, a new COX-2 inhibitor, on the prevention of lameness induced by chemical synovitis in dogs. Vet Ther 2002;3:453-464.
7. Muir WW 3rd, Wiese AJ, March PA. Effects of morphine, lidocaine, ketamine, and morphine-lidocaine-ketamine drug combination on minimum alveolar concentration in dogs anesthetized with isoflurane. Am J Vet Res 2003;64:1155-1160.
8. Muir WW 3rd, Woolf CJ. Mechanisms of pain and their therapeutic implications. J Am Vet Med Assoc 2001;219:1346-1356.
9. Wilder-Smith OH. Pre-emptive analgesia [German]. Anaesthesist 1995;44 Suppl 3:S529-S534.
10. Lamont LA, Tranquilli WJ, Grimm KA. Physiology of pain. Vet Clin North Am Small Anim Pract 2000;30:703-728.
11. Brideau C, Van Staden C, Chan CC. In vitro effects of cyclooxygenase inhibitors in whole blood of horses, dogs, and cats. Am J Vet Res 2001;62:1755-1760.
12. Jones CJ, Streppa HK, Harmon BG, et al. In vivo effects of meloxicam and aspirin on blood, gastric mucosal, and synovial fluid prostanoid synthesis in dogs. Am J Vet Res 2002;63:1527-1531.
13. Shafford HL, Lascelles BDX, Hellyer PW. Preemptive analgesia: managing pain before it begins. Vet Med 2001;96:478-491.
14. Smith LJ, Shih A, Miletic G, et al. Continual systemic infusion of lidocaine provides analgesia in an animal model of neuropathic pain. Pain 2002;97:267-273.
15. Wagner AE, Walton JA, Hellyer PW, et al. Use of low doses of ketamine administered by constant rate infusion as an adjunct for postoperative analgesia in dogs. J Am Vet Med Assoc 2002;221:72-75.
16. Shafford HL, Hellyer PW, Turner AS. Intra-articular lidocaine plus bupivacaine in sheep undergoing stifle arthrotomy. Vet Anaesth Analg 2004;31:20-26.
17. Olson JE, Stravino VD. A review of cryotherapy. Phys Ther 1972;52:840-853.
18. McMaster WC. A literary review on ice therapy in injuries. Am J Sports Med 1977;5:124-126.
19. Lippold OC, Nicholls JG, Redfearn JW. A study of the afferent discharge produced by cooling a mammalian muscle spindle. J Physiol (Paris) 1960;153:218-231.
20. Lowitzsch K, Hopf HC, Galland J. Changes of sensory conduction velocity and refractory periods with decreasing tissue temperature in man. J Neurol 1977;216:181-188.
21. Akgun K, Korpinar MA, Kalkan MT, et al. Temperature changes in superficial and deep tissue layers with respect to time of cold gel pack application in dogs. Yonsei Med J 2004;45:711-718.
22. Bocobo C, Fast A, Kingery W, et al. The effect of ice on intra-articular temperature in the knee of the dog. Am J Phys Med Rehabil 1991;70:181-185.
23. Lehmann JF, Warren CG, Scham SM. Therapeutic heat and cold. Clin Orthop Relat Res 1974;99:207-245.
24. Vannatta ML, Adair S, Schwartz P, et al. Effects of cryotherapy on temperature changes in caudal thigh muscles of dogs, in Proceedings. 31st Annu Conf Vet Orthop Soc 2004;70.
25. Hardy M, Woodall W. Therapeutic effects of heat, cold, and stretch on connective tissue. J Hand Ther 1998;11:148-156.
26. Levine D, Millis DL, Mynatt T. Effects of 3.3-MHz ultrasound on caudal thigh muscle temperature in dogs. Vet Surg 2001;30:170-174.
27. Loonam JE, Evans M, Moyer TL, et al. The effect of therapeutic ultrasound on tendon healing and extensibility, in Proceedings. 30th Annu Conf Vet Orthop Soc 2003.
28. Kiviranta I, Tammi M, Jurvelin J, et al. Moderate running exercise augments glycosaminoglycans and thickness of articular cartilage in the knee joint of young beagle dogs. J Orthop Res 1988;6:188-195.
29. Marsolais GS, Dvorak G, Conzemius MG. Effects of postoperative rehabilitation on limb function after cranial cruciate ligament repair in dogs. J Am Vet Med Assoc 2002;220:1325-1330.
30. Musch TI. Skeletal muscle blood flow in exercising dogs. Med Sci Sports Exerc 1988;20(suppl 5):S104-S108.
31. Millis DL. Getting the dog moving after surgery. J Am Anim Hosp Assoc 2004;40:429-436.
32. Millis DL, Levine D, Taylor RA. Canine rehabilitation & physical therapy. St. Louis, Mo: WB Saunders, 2004.
33. Hottinger HA, DeCamp CE, Olivier NB, et al. Noninvasive kinematic analysis of the walk in healthy large-breed dogs. Am J Vet Res 1996;57:381-388.
34. Schwartz P, Hicks DA, Evans MB. A kinematic comparison of over ground vs. treadmill walking in dogs, in Proceedings. 31st Annu Conf Vet Orthop Soc 2004.
35. Millis DL, Hicks DA, Evans MB. Kinematic assessment of selected therapeutic exercises in dogs, in Proceedings. 3rd Int Symp Rehabil Phys Ther Vet Med 2004;215.
36. Downer AH. Whirlpool therapy for animals. Mod Vet Pract 1977;58:39-42.
37. Hall J, Grant J, Blake D, et al. Cardiorespiratory responses to aquatic treadmill walking in patients with rheumatoid arthritis. Physiother Res Int 2004;9:59-73.
38. Gehlsen GM, Grigsby SA, Winant DM. Effects of an aquatic fitness program on the muscular strength and endurance of patients with multiple sclerosis. Phys Ther 1984;64:653-657.
39. Gandini G, Cizinauskas S, Lang J, et al. Fibrocartilaginous embolism in 75 dogs: clinical findings and factors influencing the recovery rate. J Small Anim Pract 2003;44:76-80.
40. Edlich RF, Towler MA, Goitz RJ, et al. Bioengineering principles of hydrotherapy. J Burn Care Rehabil 1987;8:580-584.
41. Levine D, Millis DL. Percentage of normal weight bearing during partial immersion at various depths in dogs, in Proceedings. 2nd Int Symp Rehabil Phys Ther Vet Med 2002.
42. Richley Geigle P, Cheek WL, Gould ML, et al. Aquatic physical therapy for balance: the interaction of somatosensory and hydrodynamic principles. J Aquatic Phys Ther 1997;5:4-10.
43. Jackson AM, Stevens M, Barnett S. Joint kinematics during underwater treadmill activity, in Proceedings. 2nd Int Symp Rehabil Phys Ther Vet Med 2002;191.
44. Templeton MS, Booth DL, O'Kelly WD. Effects of aquatic therapy on joint flexibility and functional ability in subjects with rheumatic disease. J Orthop Sports Phys Ther 1996;23:376-381.
45. Driver S, O'Connor J, Lox C, et al. Evaluation of an aquatics programme on fitness parameters of individuals with a brain injury. Brain Inj 2004;18:847-859.
46. Avellini BA, Shapiro Y, Pandolf KB. Cardio-respiratory physical training in water and on land. Eur J Appl Physiol Occup Physiol 1983;50:255-263.
47. Thein JM, Brody LT. Aquatic-based rehabilitation and training for the elite athlete. J Orthop Sports Phys Ther 1998:27:32-41.
48. Dunning D, Knap K, Wittek K, et al. Effects of water temperature on heart and respiratory rate, rectal temperature, and perceived exertional score in dogs exercising in and underwater treadmill, in Proceedings. 3rd Int Symp Rehabil Phys Ther Vet Med 2004;217.
49. Johnson JM, Johnson AL, Pijanowski GJ, et al. Rehabilitation with electrical muscle stimulation for dogs with surgically treated cranial cruciate ligament deficient stifles. Vet Surg 1994;23:405.
50. Carroll RE, Bird SF, Brown DJ. Electrical stimulation of the lumbrical muscles in an incomplete quadriplegic patient: case report. Paraplegia 1992;30:223-226.
51. Zupan A, Gregoric M, Valencic V, et al. Effects of electrical stimulation on muscles of children with Duchenne and Becker muscular dystrophy. Neuropediatrics 1993;24:189-192.
52. Lang DC. Ultrasonic treatment of musculoskeletal conditions in the horse, dog and cat. Vet Rec 1980;106:427-431.
53. Draper DO, Castel JC, Castel D. Rate of temperature increase in human muscle during 1 MHz and 3 MHz continuous ultrasound. J Orthop Sports Phys Ther 1995;22:142-159.
54. Gallo JA, Draper DO, Brody LT, et al. A comparison of human muscle temperature increases during 3-MHz continuous and pulsed ultrasound with equivalent temporal average intensities. J Orthop Sports Phys Ther 2004;34:395-401.
55. Steiss JE, Adams CC. Effect of coat on rate of temperature increase in muscle during ultrasound treatment of dogs. Am J Vet Res 1999;60:76-80.
56. Kapatkin AS, Mayhew PD, Smith GK. Canine hip dysplasia: evidence-based treatment. Compend Contin Educ Pract Vet 2002;24:590-599.
57. Roush JK, McLaughlin RM, Radlinsky MAG. Understanding the pathophysiology of osteoarthritis. Vet Med 2002;97:108-117.
58. Fox SM, Johnston SA. Use of carprofen for the treatment of pain and inflammation in dogs. J Am Vet Med Assoc 1997;210:1493-1498.
59. Johnston SA, Budsberg SC. Nonsteroidal anti-inflammatory drugs and corticosteroids for the management of canine osteoarthritis. Vet Clin North Am Small Anim Pract 1997;27:841-862.
60. Moreau M, Dupuis J, Bonneau NH, et al. Clinical evaluation of a nutraceutical, carprofen and meloxicam for the treatment of dogs with osteoarthritis. Vet Rec 2003;152:323-329.
61. Budsberg SC, Johnston SA, Schwarz PD, et al. Efficacy of etodolac for the treatment of osteoarthritis of the hip joints in dogs. J Am Vet Med Assoc 1999;214:206-210.
62. Impellizeri JA, Tetrick MA, Muir P. Effect of weight reduction on clinical signs of lameness in dogs with hip osteoarthritis. J Am Vet Med Assoc 2000;216:1089-1091.
63. Smith GK, Kealy RD, Biery DN, et al. Influence of body condition on canine osteoarthritis. Compend Contin Educ Pract Vet 2002;24:8-12.
64. Boston SE, Moens NM, Kruth SA, et al. Endoscopic evaluation of the gastroduodenal mucosa to determine the safety of short-term concurrent administration of meloxicam and dexamethasone in healthy dogs. Am J Vet Res 2003;64:1369-1375.
65. Reed S. Nonsteroidal anti-inflammatory drug-induced duodenal ulceration and perforation in a mature rottweiler. Can Vet J 2002;43:971-972.
66. McGettigan P, Henry D. Current problems with non-specific COX inhibitors. Curr Pharm Des 2000;6:1693-1724.
67. MacPhail CM, Lappin MR, Meyer DJ, et al. Hepatocellular toxicosis associated with administration of carprofen in 21 dogs. J Am Vet Med Assoc 1998;212:1895-1901.
68. Holazo AA, Chen SS, McMahon FG, et al. The influence of liver dysfunction on the pharmacokinetics of carprofen. J Clin Pharmacol 1985;25:109-114.
Newsletter
From exam room tips to practice management insights, get trusted veterinary news delivered straight to your inbox—subscribe to dvm360.