Equine neonatology (Proceedings)
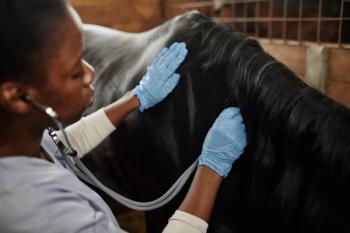
"07 Slow to go" is a 48 hour old Thoroughbred filly that was born to a 15 year old Thoroughbred mare.
"07 Slow to go" is a 48 hour old Thoroughbred filly that was born to a 15 year old Thoroughbred mare. The foal was found in the stall with the mare at 6 am on day 355 of gestation and was standing but was wet to the touch. The foal was first seen to nurse about 1 hour later. The foal passed meconium within 30 minutes. The owner checked the foal at 4PM that day and she was following the mare and nursed immediately after he approached the stall and again about 15 minutes later.
The mare has had 4 uncomplicated pregnancies previously with healthy foals delivered between 350 and 357 days of gestation. The mare foaled in the stall and that the mare and the placenta appeared normal when discovered.
The owner again checked on the pair at around 11PM on the night of delivery and all appeared well. However, at 6 am the following morning, the foal was recumbent in the stall and did not get up when first approached. The owner walked next to the foal and the foal got up but did not nurse. The owner went back out to check the foal before leaving for work and the foal nursed for a short time. When the owner returned from work at 5:30 PM, the foal was recumbent and did not rise until he assisted the foal to stand. At this time the foal did not nurse at all, so a veterinarian was called. The foal is now 24 to 36 hours old.
Examination reveals injected sclera, petechiation in the pinna of the ear, hyperemia of the oral mucous membranes and hyperemia of the coronet. Body temperature is 102.6 degrees F, heart rate is 100 beats/minute, and respiratory rate is 36 breaths per minute. The umbilicus and joints palpate normally and thoracic auscultation is normal. Loose yellow feces are adhered to the perineum and tail.
This foal exhibits clinical signs of sepsis causing bacteremia from bacterial infection via the intestinal tract, lungs, or umbilicus. The prodromal signs of sepsis are subtle and are often not recognized by caretakers. Knowledge of normal foal behavior and frequent monitoring are paramount for early identification of illness. During the first week of life, healthy foals suckle for 2 minutes 5 to 7 times an hour. Healthy foals nearly always suckle when approached by humans. Therefore, it is very unlikely that a healthy foal will not nurse each time they are observed by caretakers. Failure to nurse during checks should alert caretakers to a problem a veterinary examination is warranted. Complete blood count and immunoglobulin concentrations should be assessed during this examination.
Sepsis rapidly progresses as the bacterial infection stimulates production of inflammatory mediators in an exaggerated fashion resulting in the systemic inflammatory response syndrome (SIRS). As the inflammatory response intensifies, changes in blood pressure, vascular resistance, cardiac output, vascular permeability, clotting function, and body temperature occur that manifest as altered mental status, hypo- or hyperthermia, shivering, cold extremities, mucous membrane pallor, hyperemia, or cyanosis, bradycardia or tachycardia, poor pulse quality, poor capillary refill, and petechiation. Further progression can result in complete loss of suckle, recumbency with inability to rise, coma and death due to septic shock. Because the SIRS usually results from progression of bacteremia in the early stages of sepsis, clinical signs of localization of infection (nasal discharge, coughing, joint swelling, umbilical swelling) are rarely identified in this stage. Identification of secondary sites of infection is usually delayed by 1 to several days if the foal survives the septic shock. In some cases, localization to secondary sites occurs without development of septic shock. Pneumonia, omphalophlebitis, and septic arthritis are the most common sites of secondary infection. Meningitis, nephritis, endocarditis, and hepatic abscesses occur much less frequently.
Diagnosis of sepsis involves identifying foals in the early stages when treatment is most successful. Early intervention is essential but diagnosis in this stage is often not definitive. Proof positive requires identification of organisms in blood culture and false negatives commonly occur. Blood culture results are not available for 5-7 days which is well into treatment. Regardless, blood culture is a useful diagnostic test to confirm sepsis retrospectively and to guide antimicrobial therapy for secondary sites of infection. Historical facts, examination findings, and laboratory tests are used to make a presumptive diagnosis of sepsis on an emergency basis in order to guide life saving therapy. These findings are tabulated in a scoring system (sepsis score)1 to identify results that are statistically associated with sepsis.
When the total points for the case are > 12 the score is positive for sepsis. In the absence of complete laboratory data, a modified sepsis score eliminates arterial oxygen and metabolic acidosis and uses a cutoff of 11 for positive sepsis score. In the absence of other data, fibrinogen, blood glucose, abnormalities such as petechiation and sclera injection, leucopenia, and neutrophil toxic changes in a foal that is not suckling well should be considered highly suggestive. Because foals can progress through SIRS very rapidly and develop fatal septic shock in hours and because treatment of foals that develop severe hypotonia and coma is very labor intensive and expensive, err on the side of presumed sepsis in the early stages of neonatal disease is advised. Performance of complete blood count in the first 12-48 hours on foals that are not satisfactorily vigorous can lead to early treatment and prevent advancement to severe SIRS. Concurrent chemistry evaluation is helpful to rule out concurrent diseases such as rupture bladder in foals with more severe signs. IgG and glucose determinations are helpful stall side tests that can aide in diagnosis and treatment. Laboratory data results on "07 Slow to go" are tabulated below:
The total sepsis score for "07 Slow to go" is positive at 20 leading to a diagnosis of sepsis. Blood collected at the time of admission was later positive on blood culture for E. coli.
Early recognition and appropriate antimicrobial therapy for sepsis are paramount for successful treatment of septicemia. However, antimicrobial therapy facilitates the immune system in resolving infection so other factors influence the ability of the immune system to mount a response and are equally a important for success. These are treatment of hypoxemia if present with intranasal oxygen, maintenance of nutrition by tube feeding or assisting the foal to stand and nurse, maintenance of appropriate blood glucose, fluid, electrolyte, and IgG concentrations, and maintenance of cleanliness and body temperature. Until culture results are available, antimicrobial therapy should be broad spectrum, intravenous therapy aimed at the most common pathogens isolated in neonatal sepsis. Amikacin (21 mg/kg once daily) and ceftiofur (10 mg/kg IV every 6 hours) is the combination most often used in our hospital and was administered to "07 Slow to go". Side effects of these medications include renal compromise (amikacin) and diarrhea. Fluid balance and creatinine (measured every 3 days throughout amikacin therapy) are closely monitored during amikacin therapy. Monitoring for secondary cites of infection involve thoracic auscultation, ultrasound, and radiography, ultrasound of umbilical structures, and palpation of joints. Antimicrobial therapy should be considered should be continued for a week post resolution of all signs and a normal complete blood count and fibrinogen. Duration of therapy is generally 14 days to 30 days depending on blood culture results and signs of localization of infection.
"07 Slow to go" was treated with Amikacin (21 mg/kg IV once daily) and ceftiofur (10 mg/kg IV every 6 hours) for 7 days. A nasogastric feeding tube was placed and the foal fed milk replacer at 15% body weight for the first day increased daily to reach 20% of body weight daily. Intravenous fluids and plasma were administered to restore fluid balance and IgG. The foal responded and began nursing within 12 hours and feeding tube was removed 36 hours after initiation of treatment. The toxic changes and left shift resolved and the neutropenia improved. On Day 3 umbilical structures appeared normal with normal diameters of the urachus, umbilical arteries, and umbilical vein. Thoracic ultrasound revealed comet tails and small cavitations in the ventral thorax bilaterally. Intravenous antimicrobial therapy was continued for 7 days and then changed to cefuroxime 15 mg/kg PO twice daily. Recheck on day 10 revealed resolution of the pulmonary ultrasound changes and a normal complete blood count and fibrinogen. Cefuroxime therapy was continued for 7 more days.
Brewer B, Koterba A. Development of a scoring system for the early diagnosis of equine neonatal sepsis. Equine Vet J 20:18-22, 1988.