Diseases of the foot (Proceedings)
Pododermatitis is can be one of the more challenging manifestations of skin disease, both in terms of establishing a definitive diagnosis and providing effective care.
Pododermatitis is can be one of the more challenging manifestations of skin disease, both in terms of establishing a definitive diagnosis and providing effective care. The term pododermatitis is a general term implying inflammation of the feet and is not a specific diagnosis. For these notes and lecture, we will include diseases of the foot, foot pad and claw. The following list includes some of the more common diseases which might involve some aspect of the foot;
Allergy
Atopy
Food allergy
Infectious
Staphylococcus
Malassezia
Dermatophytosis
Gram negative bacteria
Papilloma virus
Parasite
Demodex
Pelodera
Anatrichosoma
Immune mediated
Pemphigus foliaceus
Systemic lupoid onychodystrophy
Plasma cell pododermatitis
Sterile pyogranuloma
Sterile metacarpal fistula
Metabolic
Hepatocutaneous syndrome
Keratinization disorders
Interdigital follicular cyst
Vitamin A or Zinc responsive dermatosis
Primary keratinization disorders
Idiopathic footpad hyperkeratosis
Neoplasia
Foreign Body
Fox Tail
Cactus
When presented with a patient with pododermatitis, the veterinarian should start by assessment of the signalment. Is the patient a breed prone for the development of allergies? A younger dog would be more likely to develop an allergy, demodicosis or a keratinization disorder while an older dog would be more likely to develop pemphigus foliaceous or hepatocutaneous syndrome. Pertinent historical information includes questions of how chronic or acute the condition is, along with any seasonality. If the patient is pruritic then allergies would be the primary consideration but remember many non-pruritic skin diseases may develop a secondary pyoderma which could be pruritic.
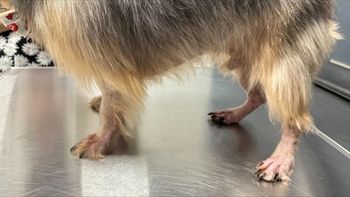
Obviously the physical examination is not limited to the feet, and the presence of skin lesions at other sites may offer clues as to the diagnosis. Inflammation of the ears or inguinal area would suggest allergy. Patchy alopecia would suggest a folliculitis such as Staphylococcus, Demodex or dermatophytosis. Lesion distribution may also be helpful in establishing the differential diagnosis. If lesions are restricted to the interdigital areas of the foot, consider allergy, parasite and infectious causes. If lesions are restricted to the foot pads, consider hepatocutaneous syndrome, keratinization disorders and pemphigus foliaceus. If lesions are restricted to the nail or nail base, consider systemic lupoid onychodystrophy, pemphigus (especially in cats) and Malassezia.
The minimum data base for most cases includes cytology of the affected foot, and usually skin scrapings or pluckings for Demodex. Feet can be a challenging area from which to obtain samples. I usually scrape the interdigital area with a dry blade and then “smear” the contents on a slide which is then heat fixed prior to staining. Applying clear or transparent tape with the sticky side pressed firmly on the interdigital skin can be useful for detecting Malassezia. The tape can be placed directly in the blue (step 3) of a Diff-Quick stain, skipping the first two staining steps and then placing the stained tape sticky side down on a slide. When Demodex is suspected, plucking and placing hairs in oil on the microscope slide can sometimes reveal Demodex when scrapings were negative.
After compiling the signalment, history, physical exam, cytology and scrapings, a shorter list of likely differentials should become apparent. Cytology will possibly have revealed a secondary infection which will need to be treated. Superficial infections can be treated topically with antifungal or antibacterial shampoos, rinses, and medicated wipes. If nodules or draining tracts or alopecia are present, these are indications of a deeper infection requiring systemic therapy, although sterile granulomas and fistulas can mimic infection. Most intermediate or deep infections of the feet require a minimum of three weeks of antimicrobial therapy, and many cases require even longer treatment. Chronic infections of the feet can result in significant secondary scarring and pyogranulation. We have found that using pentoxifylline (20 mg/kg BID) concurrently with antibiotics can “enhance” circulation and penetration of antibiotics into deep scarred areas and shorten the necessary antibiotic regiment. Unfortunately multi-drug resistant bacterial infections are becoming increasingly common. Cultures of deep tissue may be necessary, especially if the patient is failing to respond to appropriate doses of cephalosporins. In such cases we will obtain punch biopsy samples, excise the epidermis, and submit the dermis and subcutaneous tissue for tissue homogenization and culture and sensitivity. If there is a significant (3-5/hpf) number of Malassezia present on cytology, then systemic therapy with fluconazole or itraconazole (both at 5 mg/kg daily) or terbinafine (30 mg/kg daily) would be needed. Pulse dosing of itraconazole at 5 mg/kg for two concurrent days each week has also been proven effective for treating Malassezia dermatitis.
If allergies are the likely diagnosis, then an allergy work-up including a food trial with a novel protein will be indicated. If the food trial fails, then atopy should be considered the primary diagnosis. Allergy testing should be performed if the client is committed to the process of allergen specific immunotherapy (allergy shots). The practitioner should always insure test results correlate with the pruritic pattern of the patient. For example, if skin or serology shows positives only to pollens such as weeds in a patient who is consistently non-seasonal, then something is being missed. The only reason to perform allergy testing is to follow with immunotherapy. Allergen-specific immunotherapy can be one of the more cost-effective and medically effective treatment options for long-term control of atopy in many dogs. The practitioner utilizing immunotherapy should be prepared to modify the volume and frequency of the injections based on how each individual patient is responding. The content of the extract, and levels of each allergen in the extract should be based on the allergy results but also based on degrees of exposure to an allergen, length of pollination season, and of course the pattern or seasonality of the patient. Relying on the a serology company to make these decisions without specific input related to the patient will lead to lower success rates for immunotherapy.
If comedones are seen on the palmar or plantar surface of the interdigital area, and fistulas, granulomas or scar tissue are located dorsal to the comedones then interdigital follicular cyst should be considered. These patients frequently are misdiagnosed as being allergic because the patient will lick the feet. Foxtails will cause similar lesions, but without comedone formation. Antibiotics may help the secondary infection which occurs after the cyst has ruptured, but improvement is usually only partial and temporary. The only effective therapy for interdigital cyst is surgical excision or ablation with a CO2 laser. More aggressive therapy would include ablating the interdigital skin with fusion of the foot pads. Obviously a correct diagnosis is mandatory prior to this procedure. Laser therapy is also useful for viral papillomas of the feet.
Biopsies of the feet are sometimes necessary to establish a definitive diagnosis, especially regarding sterile pyogranuloma, pemphigus, hepatocutaneous syndrome, keratinization disorders, and neoplasia. Indications for biopsy include lesions such as papules, pustules, nodules and or crust present and not responding to proper antimicrobial therapy.
Based on this brief summary it is clear that there are many conditions to consider when presented with a patient with pododermatitis. Keep in mind that allergy will account for the majority of the cases, and then be prepared to biopsy when or if a case does not respond as expected. This approach should result in an accurate diagnosis which should lead to proper and appropriate therapy for most patients.