Dermatology quiz: Put your skin knowledge to the test
Test your dermatology skills on the following cases. What would you do first? Which diagnostics would yield the most information yet not break your client's wallet? Are you seeing an unusual disease or more commonly, an unusual manifestation of a common disease?
Test your dermatology skills on the following cases. What would you do first? Which diagnostics would yield the most information yet not break your client's wallet? Are you seeing an unusual disease or more commonly, an unusual manifestation of a common disease?
Photo 1.
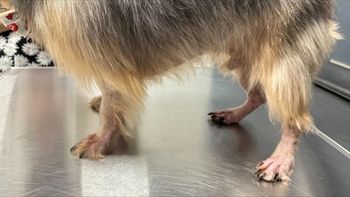
History: The patient is a 5-month-old female Lhasa Apso with generalized pruritus. She is nonresponsive to antibiotic therapy yet antipruritic doses of prednisone help moderately with the itching. The lesions consist of truncal multifocal raised crusty plaques of a two month duration. There is one other dog in the household who is not pruritic. (Photo 1)
Case 1: Pruritus
Which diagnostics would you initially perform?
- 1. Skin scrapings/combings
- 2. Trichogram/hair plucks
- 3. Ear smears/skin cytology
- 4. Fungal cultures
- 5. Skin biopsy
- 6. Serum ELISA for inhalant allergy
- 7. Serum ELISA for food allergy
Skin scrapings, combings, trichogram/hair plucks and ear smears should automatically be performed on EVERY dermatology patient. Skin scrapings, hair plucks, and combings help to rule out ectoparasites; trichograms and fungal cultures to rule out dermatophytes. I usually start with noninvasive diagnostics then move onto more involved procedures such as skin biopsies should the initial diagnostics not prove helpful. Although atopy and food allergy can start at a young age, it is unlikely. Also it is doubtful the patient will provide a valid test for inhalant allergy at this young age. Blood and skin testing for food allergy is not considered reliable and a food elimination test is the diagnostic of choice for diagnosis of food allergy.
Photo 2.
Skin scrapings and hair plucks yielded adult demodex mites. Hair plucks can be helpful in diagnosing demodicosis since the demodex mite will be found adhering to the root of the hair when viewed under low power in a drop of mineral oil. Be sure to examine ear smears in oil for demodicosis of the ear canals. No fungal spores were seen in hair shafts examined in oil under low power and a fungal culture was negative after 10 days.
Therapies for generalized demodicosis include weekly or every two weeks mitaban dips, or milbemycin 0.5-1 mg/kg bid (must be heartworm negative first), or ivermectin 200-800 ug/kg/day orally (must be heartworm negative first and a nonherding breed or mix thereof). Due to the unavailability of Mitaban, we selected ivermectin at 200 ug/kg/day orally. The patient weighed 15 pounds, so she received 0.15 cc orally once daily. We rechecked skin scrapings at monthly intervals adjusting the ivermectin dose as she gained weight. Because demodicosis is accompanied by a bacterial folliculitis, she was started on Cephalexin 250 mg tablet bid and Vitamin E 100iu orally once daily along with weekly benzoyl peroxide shampoos. Steroids are contraindicated. The ivermectin was continued 60 days past a negative skin scraping/hair pluck. The patient continues to do well (Photo 2).
Which therapy would you choose?
The differentials for a young dog with pruritus include:
- 1. Ectoparasites
- 2. Ectoparasites
- 3. Ectoparasites
- 4. Bacterial pyoderma
- 5. Dermatophytosis
- 6. Food allergy
- 7. Early inhalant allergy
The take-home point being ectoparasites, be it demodicosis, sarcoptic mange, lice or Cheyletiella, are the top differentials in a young pruritic dog. Inhalant allergy can start this young as can food allergy but are not as likely. Dermatophytosis affects young immunosuppressed patients and it seems, at least in our practice, to favor young Yorkshire Terriers but should be suspected in any young patient.
Photos 3 and 4.
The lesions seen in this patient are unusual in that generalized demodicosis does not usually take the form of multifocal crusty plaques. When I first examined this patient I truly did not know what this patient's diagnosis was. But as always, if you approach the case systematically and perform your routine dermatology diagnostics, it wasn't long before the demodex mites were viewed.
History: The patient is an 8-year-old female spayed St. Bernard with a one-month duration of progressive skin lesions involving the muzzle and tongue (Photos 3 and 4). The referring veterinarian had already biopsied these lesions and found them to be viral papillomas. The question is why did she develop these lesions and why are more lesions rapidly emerging?
Case 2: Skin lesions
Which diagnostics would you initially perform?
- 1. Skin scrapings/trichogram/hair plucks
- 2. Complete blood count, serum profile, thyroid panel, urinalysis.
- 3. Thorough physical examination
All of the above are certainly indicated since viral papillomas at least in puppies are felt to be a reflection of an immature immune system. If this is true in older patients, what is causing immunosuppression in our patient? There is no history of steroid use, the patient is fed a name brand commercial diet, is current on vaccinations, fecal exams and heartworm prevention. There is no history of weight gain or polyuria, polydipsia or polyphagia. On physical examination the only abnormality is palpation of a possible abdominal mass. Radiographs are negative for any abdominal mass and complete blood count, serum profile and urinalyses are normal. Results of the thyroid panel reveal an elevated TSH, low FT4, and low borderline T4. Thyroid supplementation using Soloxine 0.1mg/10 lbs. body weight bid is started. What is not known is if the early hypothyroidism is the cause of the skin lesions or an incidental finding.
Photos 5 and 6.
Whereas the T4 was low borderline, the TSH and FT4 appear to be the first to change in early hypothyroidism.
Therapies for viral papillomas include administration of an autologous vaccine or Interferon A. Both are anecdotal in their administration and success as are other immune stimulants. Upon communication with the owner after two weeks of Soloxine therapy, the papillomas had regressed by 50 percent and after 30 days of Soloxine, lesions had regressed completely. The owner was reminded to have the thyroid panel rechecked after 60 days of beginning Soloxine, three to four hours after the morning dose.
This patient was presented because of the unusual presentation of hypothyroidism, not to mention the advanced age of onset of what is normally a skin disease of young dogs. Differentials included underlying internal medicine disease such as hypothyroidism, Cushing's disease either iatrogenic or naturally occurring or underlying neoplasia, any of which could produce immunosuppression.
Photo 7.
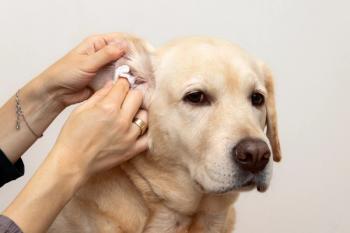
History: The patient is a 6-year-old neutered male Golden Retriever with a six-month history of pruritus of the face and legs (Photos 5 and 6). Antibiotics help somewhat with the skin lesions but not with the pruritus. Steroids have not been used. Upon physical examination the patient's ventral neck, periocular areas and cranial portions of the front legs are alopecic and hyperpigmented. The skin of the neck is edematous. Ear canals are mildly inflamed with moderate brown discharge and the medial pinna inflamed. Overall he has been lethargic, mildly depressed, slow in getting up from a recumbent position, and has "tragic facies." There is no polyuria, polydipsia or polyphagia. The patient is on monthly heartworm preventative, current on vaccinations and on a brand name commercial dog food.
Case 3
Which diagnostics would you initially perform?
- 1. Skin scrapings/combings/hair plucks
- 2. Ear smears/skin cytology
- 3. Fungal culture
- 4. Skin biopsy
Skin scrapings and hair plucks yielded many adult demodex mites. Ear smears in oil yielded adult demodex mites and ear smears for infectious organisms yielded yeast 2+.
Which diagnostics would you perform next?
- 1. Complete blood count, serum profile, urinalysis.
- 2. Thyroid panel
- 3. ACTH stimulation
- 4. Radiographs/ultrasound
In adult onset demodicosis in a patient that had not been administered steroids, an underlying internal medicine disorder that predisposed to the demodicosis needs to be determined. Underlying problems such as hypothyroidism, Cushing's disease, allergy, or neoplasia need to be ruled out. The complete blood count yielded a mild normochromic normocytic nonregenerative anemia and hypercholesterolemia which can be compatible with hypothyroidism. A thyroid panel indicated an elevated TSH and low FT4 and T4. Liver enzymes were normal as was the remainder of the physical examination. Although abdominal radiographs and an ACTH stimulation would aid in ruling out underlying neoplasia and Cushing's disease, respectively, the patient's clinical appearance and blood work were suggestive of hypothyroidism and Soloxine 0.1mg/10 lbs. body weight bid was started. Additional therapy included weekly benzoyl peroxide shampoos, enrofloxacin at 1 mg/lb body wt sid, Vitamin E 400 iu po sid, clotrimazole lotion 2-3 drops AU bid, and ivermectin 0.8 ml po sid (patient weighed 80 lbs.) with a recheck in 30 days. No steroids, including ear medications containing steroids, were used as any further immunosuppression needs to be avoided.
Upon recheck in one month (Photo 7), the patients ventral neck cellulitis had improved and hair growth was beginning. He was feeling much better, the lethargy had subsided as well as the "tragic facies" seen in some patients with hypothyroidism. The treatment plan was to recheck the patient at 30-day intervals for the demodex, continue the ivermectin until 60 days past a negative skin scraping, recheck the thyroid profile in another 30 days, three or four hours post pill, and discontinue antibiotics when the bacterial pyoderma had substantially improved.
Treatment options for this patient with adult onset demodicosis included Mitaban dips weekly, or ivermectin at 200-800ug/kg/day orally until 60 days past a negative scraping (must be heartworm negative first), or milbemycin 0.5-1 mg/kg bid until 60 days past a negative scraping (must be heartworm negative first). Because of the unavailability of mitaban and the expense of milbemycin for a patient this size, ivermectin was selected beginning at the 200 ug/kg/day oral daily dose. Ivermectin should be avoided in herding breeds or mixes thereof and used cautiously in geriatric patients as neurologic side effects have been seen in elderly patients at the low end of the dosage range. The owner must be instructed on how to draw up the correct dose of ivermectin and nothing larger than a 1-cc syringe should be dispensed to minimize the possibility of a dosing error. Unfortunately with the unavailability of Mitaban which is the only FDA-approved drug for demodex, use of either ivermectin or milbemycin for demodicosis is off label. When generalized demodicosis occurs in an adult patient, an underlying etiology needs to be determined. We were fortunate in that our patient turned out to be hypothyroid but had that been normal, an ACTH stimulation test despite the normal liver enzymes and abdominal radiographs would have been the next diagnostics undertaken. Atopy was also a consideration as Golden Retrievers are a predisposed breed but the age of onset was not characteristic.
Treatment
Hope you scored well on the quiz. The take-home message is to start with noninvasive procedures such as scrapings, hair plucks, ear smears and skin cytology then get more invasive as those test results become evident. Remember there are more unusual presentations of common diseases than unusual diseases!