Derm Jeopardy: "I'll take annoying parasites for $400, Bob" (Proceedings)
Despite the advent of newer demodicidal therapeutics, management of the chronic relapsing or refractory demodicosis cases remains a frustration. Conservative therapy continues to represent the preferred approach to localized demodicosis in the juvenile. Benzoyl peroxide gel or cream is often selected as an initial choice.
Canine demodicosis - current therapeutic trends
Despite the advent of newer demodicidal therapeutics, management of the chronic relapsing or refractory demodicosis cases remains a frustration. Conservative therapy continues to represent the preferred approach to localized demodicosis in the juvenile. Benzoyl peroxide gel or cream is often selected as an initial choice. Application is performed daily for 30 days then reassessed. Total body acaricidal therapy is not warranted or recommended for the localized form in most cases. Providing adequate opportunity for spontaneous remission should be encouraged. Use of benzoyl peroxide shampoos is recommended. The majority of localized cases will self limit, while others may progress to a generalized form.
Treatment of the generalized case often necessitates total body demodicidal therapy, although spontaneous recovery is observed. This is more likely in young dogs with multifocal lesions than those with diffuse generalized areas of involvement. Initiation of systemic or generalized demodicidal therapy is accompanied by the recommendation for neutering since spontaneous remission cannot be evaluated. Treatment options are influenced by previous therapy and response.
Juvenile onset demodicosis
The mechanism of this disease occurs as a cosequence of immunological deficiency primarily affecting T-Lymphocyte activity allowing for the proliferation of Demodex canis. There are different manifestations of the disease depending upon the extent of involvement (localized vs. generalized) and whether accompanied by complication of bacterial infection.
Localized demodicosis
Localized demodicosis is relatively common in young dogs and has a high tendency of spontaneous resolution. The face and forelimbs are most frequently involved and often accompanied by hyperpigmentation or comedone formation. Stress factors may potentiate the problem. Dogs between 3 and 6 months are most represented in this group. Lesions may be variable but limited to multifocal circumscribed areas of alopecia, erythema and scaling. Conservative therapy may be considered including the use of benzoyl peroxide gel or topical acaricidal ointment (Goodwinol Ointment (R)) daily. Abstinence of systemic or generalized total body topical therapy allows the identification of those cases that will progress to generalized pattern. This distinction becomes important when consideration of the genetic potential for propagation of the disease if breeding were to be considered.
Generalized demodicosis
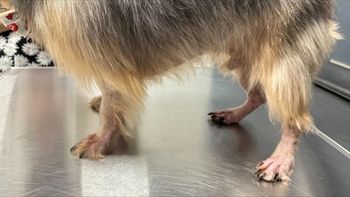
The progression of localized demodicosis is less likely since the vast majority of localized cases will resolve with or without therapy. Generalized case usually occur between 3-18 months although adult onset generalized demodicosis is observed. Lesions may be multifocal but are more commonly regionalized or generalized. Again the distribution includes the face, forelimbs, feet, or generalized over a large percentage of the body. This form is accompanied by secondary pyoderma further complicating the condition. In addition to the typical alopecia, erythema, scaling and hyperpigmentation, papules, pustules, furuncles, draining tracts and fistulous pedal lesions may be observed. Pruitus may be observed in these cases and inappropriate steroid therapy may have been used prior to the diagnosis. Demodectic pododermatitis with secondary infection may be associated with discomfort and represents a problem that may take protracted time to resolve. Diagnosis is made by deep skin scraping with the identification of the mite population. Occasionally the diagnosis is made through skin biopsy in breeds with unusually thick skin (e.g. Shar Pei).
Therapy
Acaricidal treatment of uncomplicated generalized demodicosis in the juvenile is amitraz (Mitaban(R) - Upjohn) applied very two weeks at a concentration of 250 ppm with evaluation following 3-6 applications.
Agricultural amitraz pour-on products have been used as a less expensive amitraz source with demonstrable efficacy but is not recommended if the small animal licensed product Mitaban (R) is available. Tactik is a brand used at a dilution of 10cc/gal providing 0.125 % solution. This is an extra label use on dogs. Treatment should be continued as long as positive skin scrapings are found. Removal of hair from medium to long coated dogs should be performed intermittently during the treatment process. Treatment should not be discontinued following a specific number of applications but through monitoring the regression of clinical signs and the mite population. The animal should be kept dry between treatments with a benzoyl peroxide shampoo applied before the subsequent treatment, Two treatments should be used following the evaluation with multiple negative skin scrapings obtained from previously affected areas. Adverse reactions to amitraz includes CNS signs with depression, sedation, weakness, ataxia, vomiting, hypothermia, pruritus, skin irritancy and allergic reactions. The animal should be bathed to remove as much residual amitraz as possible and provided closely monitored systemic treatment for support. Yohimbine has demonstrated effectiveness in reversing the intoxicating signs of amitraz should they be observed. It is used at one half the dosage recommended for tranquilization reversal. Usually .25 ml/20lbs. or less is effective. This may be used as a pretreatment in animals of know sensitivity to amitraz.
Treatment of Complicated Generalized Demodicosis
The most common complications of demodicosis are pyoderma, scales/crusts and suppressed thyroid function. Recognition and treatment of the pyoderma is suggested prior to or during acaricidal treatment. Anti-seborrheic shampoos (benzoyl peroxide) should also be used and hair removal of breeds with medium to long coats. Hydrotherapy may include whirlpool agitation or warm water soaks prior to bathing. Antibiotics should be continued for as long as necessary depending on the response. Acaricidal treatment can be started following an initial response, but should be postponed if topical demodicidal therapy is being used and the dog is aggressively being bathed or treated with hydrotherapy. Systemic therapy is definitely ideal under these circumstances since both effective acaricidal therapy can be used in combination with bathing. Topical acaricidal treatment in the presence of excessive scale, crust or pyoderma limits the response and is not practical. Early demodicidal therapy before complete resolution of the pyoderma is often helpful
Treatment of the Refractory Case
Evaluation of the case with chronic persistent demodicosis should include a check list to review factor(s) associated with poor response. The following items are the major considerations for failure:
1. Inadequate control of coexisting or complicating dermatoses (pyoderma, scaling/crusting).
2. Coexisting treatment with glucocorticoids.
3. Deteriorated demodicidal potency. (Outdated amitraz, reopened vials and solutions recently diluted/outdated ivermectin or ivermectin kept in clear containers).
4. Bathing or getting wet between treatments.
5. Not removing hair from long coated dogs
6. Inadequate contact time with acaricide.
Optimizing acaricidal therapy is the most logical approach in the relapsing case. All of the check list items for failure should be corrected or modified. Principles of treatment should include the following:
1. Application to dry skin may optimize absorption. Have the owners bathe 12-24 hours before scheduled topical demodicidal treatment.
2. Allow adequate contact time. Continue applying solution for at least 15-20 minutes.
3. Use manufacturer's recommended dilution for amitraz.
4. Apply at weekly intervals.
Regular monitoring of the relapsing case is necessary to provide an adequate treatment schedule. Skin scrapings should be performed after every 3-4 treatments. Following the evaluation with no mites observed, 2-3 additional treatments should be performed. Following the last treatment, a period of 4-8 weeks should be allowed before reassessing by performing multiple skin scrapings.
The cases that cannot be resolved sufficiently to stop therapy will require additional or different acaricidal therapy or be placed on a maintenance regimen:
Spot therapy:
Localized treatment is usually restricted to feet and facial areas where persistent demodicosis is likely to be found. Mitaban(R) and mineral oil may be used daily or every other day. Mitaban(R) 0.5-1.0 ml is mixed with 1 oz. of mineral oil. Stability of this combination is unknown. It is best to place the mixture in a dark or amber bottle and place in a protective bag in the refrigerator. An optional treatment approach for more rapid recovery in cases with heavy infestation or in cases with refractory demodicosis is the application of amitraz to ONE HALF the body daily.
Another option for regional treatment is using an aqueous preparation which should be made fresh with each application. Smaller volume of solution can be made by proportional dilution. Remaining Mitaban(R) can be stored in the freezer in a protective bag (Zip Loc(R)). Affected feet can be soaked daily or every other day as required. Tactik can be used at the dilution of 1 ml/100ml water for regional therapy or 1.5 ml added to 8.5 ml of mineral oil for spot therapy or treatment of the ears.
Promeris® (Fort Dodge)
The addition of amitraz for the dog formulation in addition to the metaflumizone enhances the application in tick infested environments with some potential application as a demodicide or scabicide. The usage of metaflumizone and amitraz every 14 days resulted in 99 % reduction of demodex mites in a 3 month treatment program. Monthly application resulted in 94% reduction in three months and success rate based on zero mite counts was observed on day 84 were 43% for dogs treated monthly and 62.5 % for those treated every two weeks.
Systemic therapy:
1. Ivermectin has shown efficacy when used daily by oral administration at a dosage of 300 - 600 ug/kg. (0.3 – 0.6 mg/kg) but has not demonstrated efficacy when used intermittently (weekly). Duration of therapy is to effect. The treatment protocol used most commonly is a maintenance dosage of 400 ug/kg (0.4 mg/kg) orally daily. This dose is not administered without the use of multiple increasing incremental doses as a trial to detect sensitivity and adverse side effects is necessary. After calculating the maintenance dose at 0.4 mg/kg, the initial trial dose is calculated at 10-25 % of the maintenance dose. The dose is then gradually increased daily (or after a two day treatment at each dose) until the maintenance dosage is achieved. Ivermectin is then administered orally daily throughout the treatment regimen unless there are complications requiring the modification or discontinuation of therapy. If the response is minimal the dosage may be increased to 600 ug/kg (0.6 mg/kg). Signs of toxicity include depression, ataxia, mental dullness, seizures, vomiting, diarrhea, collapse. This drug should only be used in non-sensitive breeds and after the animal has been tested for heartworms. The owner should be instructed to discontinue if signs of toxicity occur. Therapy should be continued until at least two sets of negative scrapings two weeks apart have been acquired. Treatment for two weeks beyond this point is then performed with a reevaluation 4-6 weeks following the final treatment. Reevaluation every 3-4 weeks is usually performed at the beginning of treatment with more closely acquired evaluations every 2 weeks as the end point is reached. The concurrent use of antibiotics may be necessary and if there is evidence of pruritus therapy may include non-steroidal medication but the use of steroids should be eliminated from the treatment regimen. Treatment may take as long as 6-7 months. Animals that do not resolve the infestation with this therapy become candidates for maintenance therapy (see below).
2. Milbemycin (Interceptor) therapy has shown variable efficacy for demodicosis but is decidedly more expensive than ivermectin and probably not as efficacious. The dosage required is 1.0 - 2.0 mg/kg and must be administered daily. Observations suggest that a dosage closer to the 2.0 mg/kg/day is necessary to achieve optimal response. This drug has been used in the treatment of sensitive breeds where ivermectin has not been acceptable. The methodology is the same as that used for ivermectin treatment in so far as the duration and monitoring of the case is involved. Follow through with therapy is important with termination of therapy dependent upon achieving at least two sets of negative skin scrapings
Maintenance therapy:
Maintenance therapy is customized to each animal. The objective is to suppress the proliferation of mites to a minimum and to attain an asymptomatic state. This therapy is not satisfactory if a substantial population of mites is present. It is necessary to treat more aggressively in the initial phase then modify to a maintenance regimen based upon the individual response. Topical applications are typically performed on a 2-4 week interval. The manufacturer's recommendation of dilution is followed although the animal is allowed to maintain a normal coat. Systemic therapy may also be used in a maintenance program and more desirable. This is accomplished by the administration of ivermectin or milbemycin on a schedule sufficient to control clinical signs. This may be an alternate day or every third day dose. Less frequent treatment will unlikely be effective in controlling the refractory or frequent relapsing case. Most cases are managed with therapy three times per week such as a Monday, Wednesday and Friday schedule. The avoidance of immunosuppressive drugs is imperative and the routine monitoring essential. Coexisting diseases may play an important role in the persistence of controlling progressive demodicosis. Canine atopy has been recognized in the Southeastern US as a problem commonly observed in the young dog with a history of demodicosis where the persistence of the infestation is interrelated to the hypersensitivity. The control of both diseases without the use of glucocorticoids may be very challenging. Adverse reaction to food is another juvenile disease that may be encountered with demodicidal refractoriness.
Feline demodicosis
Feline demodicosis may be caused by different species of mites. Demodex cati and Demodex gatoi are identified in feline demodicosis.
Demodex cati
Demodex cati is an intrafollicular mite similar to demodex canis and is a relatively rare condition which is frequently observed in coexistence with other underlying disease. It is seen more commonly in older cats with conditions such as diabetes mellitus, FeLV or FIV infection, autoimmune disease, chronic upper respiratory disease or chronic glucocorticoid therapy. Skin lesions include alopecia, hyperpigmentation, erythema scale, crusts, ceruminous otitis, papules, comedones and excoriations if pruritus is involved. Treatment has been successful with Ivomec 1% at 250-300 mg/kg (.25-.3 mg/kg) three times weekly. Lime sulfur has also been used weekly for 4-6 weeks but is messy and can stain white or light coated cats. Vomiting may be observed if the cat is allowed to lick the residual lime sulfur from the hair. E-collars may be helpful to avoid the systemic effect of the lime sulfur ingestation, Amitraz has been used in cats but with serious side effects observed and therefore should be avoided.
Demodex gatoi
Demodex gatoi is a new comer with the first report in the early 80's. This mite lives in the superficial stratum corneum. It is easily distinguished from D. cati by its short, blunt tail and abdomen. Unlike D.cati, D. gatoi is contagious to other in-contact cats requiring different strategy for identification of coexisting infected cats and a therapeutic plan. D. gatoi is typically observed with excessive pruitus producing lesion of alopecia, papule, scale, crusts and erythema with excoriations. The presenting clinical signs are consistent with allergic dermatoses. The head, neck, elbows and trunk are most often affected. Diagnosis may be challenging and require both skin scrapings and acetate tape examination to find the mite. The therapy of choice for Demodex gatoi is lime sulfur 2% applied weekly for 6-8 weeks. Two sets of negative skin scrapings should be acquired before discontinuation of therapy. Ivermectin at 250 -300 ug/kg may be considered if lime sulfur is intolerated. The ivermectin is administereddaily or every other day as an oral therapy. The dosage of 300 ug/kg is equal to 0.15 ml of 1% solution per 10 lb body weight. The standard dosage for the cat is between 0.1 – 0.15 ml.
Recognition and Treatment of Canine Scabies
Canine scabies is most often confused with either canine atopy or food allergy +/- flea allergy. Distribution patterns may be comparable. The facial area, ears, ventrum, and extremities are classical involved although early cases may have generalized pruritus without a classical pattern. Response to glucocorticoid is typically partial, much like the responsiveness of food allergy. Complicating superficial pyoderma is a common factor. The characteristic scaling and crusting may resemble cutaneous malassezia which may also be a complicating disease and therefore should be evaluated, Treatment with typical flea control products may modify the disease features but not be sufficient to eliminate the scabies mite. From an historical perspective, not all in-contact dogs or humans will develop lesions or clinical signs restricting the interpretation of this information in leading to disease confirmation. Skin scrapings are the most reliable method of diagnosis but are only positive in 50% of the clinical cases where multiple skin scrapings are performed. Ear margins and extremities are the most yielding areas to scrape particularly in heavily crusted regions. Identification of a single mite or egg is diagnostic. The standard pinnal-pedal reflex has been estimated to have 82% sensitivity and 94 % specificity. The only confirmation is by demonstration of either adult or immature forms of the parasite.
Relevant clinical points concerning Sarcoptes scabei infestation are:
1. Clinical features resembling other pruritic dermatopathies particularly atopy and food allergy.
2. Limited reliability of diagnostic testing for disease confirmation;
3. Variable dependability of acaricidal products;
4. Contagiousness/asymptomatic carrier state and zoonotic significance of the disease.
Topical acaricidal treatment:
If scabies is suspected, treatment should be instituted. This is a curable disease unlike so many dermatoses that are only controllable. All topical therapy should be applied at a regular interval (weekly) for a minimum of 4-6 weeks. The dog should be kept dry between applications with exception of a cleansing or anti-seborrheic bath just prior to the next treatment. The acaricidal product should not be rinsed from the dog following the treatment. All medium to long haired dogs should be clipped with a #10 or #40 clipper if topical treatment is elected. This procedure should be repeated every 2 weeks during the treatment regimen.
5. Lime sulfur is a smelly but an effective scabicide at 3- 4% concentration for topical application. Scented products are commercially available (Lym Dyp, DVM Inc.) although horticultural lime sulfur may be substituted if a veterinary product is not available. Weekly application is sufficient but should be continued for a minimum of 4 -6 weeks. Sulfur is quite soothing, antibacterial, and antifungal. A complicated case of canine atopy with secondary pyoderma will improve with this treatment, thereby leading to a false conclusion when diagnostic confirmation has not been attained. Monitoring lesions and intensity of pruritus is essential. Lime sulfur may stain materials (porcelean tubs) and tarnish metal (particularly gold) in addition to having a pungent odor thereby restricting its use.
6. Amitraz diluted to 250ppm has shown regional efficacy but is not totally reliable. The effectiveness is variable with respect to different geographical regions. There are minimal side effects and the cost is reasonable. It is also approved for canine application nut not labeled for scabicidal activity. Multiple treatments are necessary. Application weekly for 4-6 weeks should be curative if there is no mite resistance and the provisional diagnosis was totally correct. Limitations include long hair coats and poor client compliance.
7. Fipronil (FrontlineR) spray has been shown effective as a scabicide when applied uniformly and at label dosage weekly for 4-6 weeks. Clinical trials have been conducted but not reported.
8. Organophosphates may be effective but are variable depending upon region of the country (parasite susceptibility) and type of organophosphate used. Phosmet has regional effectiveness as a scabicide although it is not as popular as a consequence of f organophoshate concerns. Some veterinarians still utilize stock piled Paramite.
Systemic acaricidal products:
Systemic scabicidal therapy is most ideal because it assures more complete mite kill and has more reliable outcome for ruling out scabies. It also allows concurrent therapy with shampoos for antimicrobial, anti-seborrheic or antipruritic effect. In contact animals may also be treated more easily if systemic therapy is instituted. The use of a registered product with label indications for the treatment of scabies is certainly considered the best because of potential legal implications. Selamectin is the only systemic scabicide for use in the dog; all others are extra-label. Ivermectin is still popular in the non-sensitive breeds due to efficacy and expense. Evaluation for heartworms is necessary for dogs without consistent preventative therapy.
1. Ivermectin is highly efficacious, inexpensive, convenient to use BUT NOT APPROVED for small animal application: It is nearly 100% effective with 2-3 treatments and may be administered parenterally (S.Q. injection) or orally. Adverse reactions have been observed, particularly collies or shelties and other related breeds where ivermectin therapy should be avoided. ("White feet....Don't treat"). The dosage is 250 - 300 ug/kg (0.25 – 0.3 mg/kg) S.Q. or P.O. and repeated weekly for three treatments or administered every 2 weeks for 2-3 treatments.
2. Milbemycin (InterceptorR) may be used in breeds with suspected sensitivity to ivermectin. The dosage is 1-2 mg/kg body weight. Milbemycin is also extralabel use at this dosage in dogs and for scabicidal therapy as well as being much more expensive. It can be used in sensitive breeds. There are several regimens. The use of one dosage every 7 days for three treatments has been associated with results varying from 71% to 100%. The extended use of two more treatments increases the efficacy to nearly 100 %. Another approach is to administer the drug for three consecutive days per week for 4 weeks.
3. Selamectin (RevolutionR) is an avermectin with label indications for scabicidal therapy and has the benefit of systemic activity. It has been reported to be over 95% effective with one treatment and 100% after two treatments according to Pfizer. Treatment failures have been reported by anecdotal observation and may require more protracted therapy. Administration every two weeks for three treatments then every 3-4 weeks for three more treatments has been successful.
4. Moxidectin: CydectinR is available for injection at the dose of 0.25 mg/kg SQ every seven days for 3 treatments. Another regimen is 0.4 mg/kg orally every 3-4 days for 3-6 weeks. The author has no experience with this therapy.