The CSI approach to pruritic pets: interviewing the witnesses (owners) before assessing a crime scene (skin) (Proceedings)
The skin is the largest organ of the body and, in the view of many practitioners, it often accounts for the largest number of headaches. One would expect that since the skin is so easy to visualize, a diagnosis should be an easy task when compared with other, more hidden body organs. The problem is that many skin conditions have the same clinical presentation.
Overview of the issue
The skin is the largest organ of the body and, in the view of many practitioners, it often accounts for the largest number of headaches. One would expect that since the skin is so easy to visualize, a diagnosis should be an easy task when compared with other, more hidden body organs. The problem is that many skin conditions have the same clinical presentation.
Studies have shown that dermatological disease is the second most common reason for presentation at a small animal practice (preventive health care is number one) and that pruritus is the most common presenting complaint in these patients (Hill et al 2006). Educated owners are becoming more knowledgeable these days of the diagnostic capabilities of the practitioner. They are more concerned about adverse and long-term reactions to symptomatic therapy and want to be sure that the therapy is the most appropriate for the condition. In short, they are in search of a diagnosis.
Veterinary dermatology is largely about detective work. This is, of course, most important in the "repeat offenders". It is important to interview the "witnesses" (caregivers) thoroughly before examining the "crime scene" (patient). Then collect appropriate samples (evidence) for evaluation, and finally follow a logical course of action to come to the right conclusion.
Objectives of the presentation
This presentation is designed as a "back to basics" presentation that is divided into 4 parts through the morning. The goal is to present a logical approach to the pruritic pet and to review diagnostic tests available to us. Some of the "tricks" that dermatologists use to increase the sensitivity of these tests will be presented. Discussion will include recommendations as to the correct timing in performing these tests. If time allows, the hope is to end with an audience participation session in working up these cases. Treatments available for these patients were presented in a previous lecture at this conference; this information is available elsewhere in these proceedings. Space limitations for the proceedings did not allow for inclusion of references. However, they are available upon request. Please feel free to email me at
The threshold theory of pruritus
The threshold theory suggests that an individual may tolerate a certain level of a stimulus without exhibiting clinical signs of pruritus (Reedy et al 1989). Put another way, as long as a patient remains below the critical threshold, it isn't pruritic. For example, a patient with a low-level sensitivity to both house dust mites and fleas may tolerate low levels of exposure to each individually, but may become pruritic when exposed to them concurrently. Allergen specific immunotherapy (ASIT) would not be needed as long as the flea burden is controlled. Therefore, our goal should be to determine the causes of pruritus that keep the pet below the "threshold".
"Interviewing the witnesses"
Our clients tend to tolerate more when it comes to their own health that they do for their pets. When it comes to pruritus, I explain to the owner that it is not my goal that the patient never, ever licks, runs, bites, scratches, chews or in any other way traumatizes itself. It's like asking a human allergist to give me so much medication that I will never ever sneeze or have itchy eyes – it's an unrealistic goal and the treatment will be worse than the disease. Therefore, during the interview process, one should take the time to determine the owner's expectations (and, in general, to set more realistic goals, without appearing to be uncaring), Knowing the client's tolerance to their pets itchiness (one of the most common complaints that I hear is "I can't stand that licking noise at night!") and assessing their capabilities insofar as treatment is concerned will give the experienced interviewer a timeline in which to work!
Therefore, part of the evaluation should include the owner's ability to perform the tasks that are requested (e.g. shampooing twice weekly). It is wise to explain to the owner that, in the beginning, there is a lot of time and expense. Indeed, I believe that one of the reasons that dermatology referral centers are successful is that we have a greater number of compliant caregivers.
The dermatological history often is more valuable than the examination. A good detective will collect all the clues needed, and will be well on the way to solving the pruritus puzzle. Most referral centers have a detailed questionnaire that the client is required to complete before the visit. (One example of a questionnaire can be found at our website -
Logic is the key. What are the most important questions? For the pruritic pet, it may help to remember the acronym:
S-C-R-A-T-C-H:
Severity
The severity of the condition can often give many clues as to the cause. Sarcoptic mange is an extremely itchy, continual condition that often keeps the animal and the owner up all night while the pet continues to scratch incessantly. A non-allergic flea infested pet, on the other hand, may have intermittent biting episodes when on a "search and destroy mission" with long rest periods in between. As mentioned above, one must always take the pet's own threshold to discomfort (and the pet owner's threshold to the pet's discomfort) into consideration. Ask the caregivers about the frequency and duration of the pet's self-trauma to get an idea of the owner's tolerance. Opioid peptides released during stress may potentiate pruritus (Koblenzer 1999, Panconesi 1996). More "intense" or "uptight" pets may seem to be more severely affected. Interestingly, it has been shown in human medicine that, when stressed, symptoms in people with psoriasis and atopic dermatitis tend to worsen (Arndt, 2008). The hypothesis for the pathogenesis of canine atopic dermatitis is that, in the acute phase, an epidermal barrier defect could facilitate the contact of environmental allergens and microbes with epidermal immune cells at skin sites (Olivry, 2004). Interestingly, a link has been found in humans between stress and increased epidermal permeability (Garg, 2001)
Contagion
Have other family members, friends or in-contact pets been affected since the condition was noticed in the pet? (Careful...you may end up with more information than you bargained for! – owners are often very inclined to show their own skin problems). What is the boarding or travel history? (This is generally where the owner pulls out the travel pictures). If multiple pets in the family are affected, it should raise the index of suspicion that they are "sharing" something. On the other hand, if only one pet is affected, it doesn't mean that the problem isn't contagious as some pets are more "sensitive" than others are. I have diagnosed scabies in homes where the owner and multiple pets were affected but the "culprit" was not apparently pruritic.
Response to therapy
This series of questions can often offer the best clues. Chronic pruritus is one of the most common reasons for people to change veterinarians and so a complete history of previous treatment is essential. What treatment worked? This section is a bit of an advertisement for the value of follow-ups, either in person or by telephone. It's important to be clear to the client that the question is "while you were giving the medication"; clearly, if the problem resolved after the treatment stopped, they wouldn't be there.
Assessment of response to therapy may be difficult or even impossible to discover when certain modes of treatment were attempted concurrently (e.g. steroids and antibiotics). It takes a good "salesperson" to explain why it is best to assess individual treatments. Other questions to consider include whether the therapy completely was or incompletely effective? Sarcoptic mange is often incompletely responsive to anti-inflammatory doses of steroids; food intolerances are variably responsive. Most atopic patients will respond to prednisone at a dose of 1 mg/Kg, and so the lack of response may be indicative of a confounding factor such as an adverse food reaction, concurrent microbial or parasitic disease.
If the pruritus totally resolves following antibacterial treatment, you are much more likely to be looking at a pyoderma that is pruritic as opposed to pruritus leading to a pyoderma. Look for the underlying immunosuppressive event in these cases (e.g. endocrinopathies (not pruritic on their own), or perhaps a disorder of cornification). To complicate matters, however, there is the rare patient with adverse food reactions that will present with a pyoderma in which the pruritus totally resolves with antibiotic therapy (Chesney 2002). How long was the pet treated? How soon following treatment did it relapse? One common reason for relapse in pyoderma cases is an incomplete duration of treatment. Be sure to treat the pyoderma for an appropriate period of time; it is important to differentiate a recurrent from a non-responsive condition, especially in these days of bacterial resistance (discussed in more detail later in the presentation). Did the condition worsen following treatment (drug reaction?). What was the response to antiparasitic therapeutic trials?
Affected areas
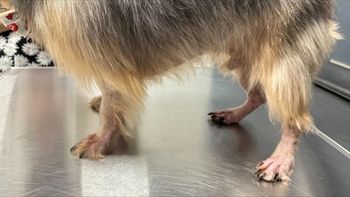
Atopic animals (the new definition includes adverse food reactions) most often present with pinnal, facial and pedal involvement. Fleas like to be in the "Florida" or "Texas" triangle (named according to where you live) - the triangle formed by the centre of the back, moving laterally and distally towards the tail. Scabies affects the ears, ventral abdomen, hocks and elbows. Patients with environmental sensitivities are more commonly front end itchy. Parasites often prefer the hind end. Food allergies can present anywhere but some patients will present with ears, rears and paws as the primary locations. In one paper, 26% of patients with food allergies presented with otitis as the principal presenting sign (Chesney 2002).
Timeline
What is the age of onset? For pets less than 6 months of age, one should consider food intolerance and parasitic hypersensitivity as likely offenders. If more than 6 months but less than 3 - 5 years, one may want to add environmental hypersensitivity to the list as well, but if more than 5 years, environmental allergies is less common in patients that have lived in the same region all of their life (food reactions are less time sensitive). One may wish to consider pruritus secondary to infection, infestation, tumors (some forms of epitheliotropic lymphoma are pruritic) or immune mediated diseases as the more likely candidates in the older dog. How has the disease progressed with time? Is there a seasonal variation (e.g. flea season, atopy)? Adverse food reactions and parasitic hypersensitivities (other than fleas) are unlikely causes of seasonal pruritus, unless a particular diet is fed seasonally.
Conditions (environment/housing/management)
Where does the pet spend most of the time? (Outdoors? If indoor, where indoor?). This will help you to decide of risk of parasites, dermatophytes, etc. (although I have diagnosed ringworm and fleas in strictly indoor apartment cats). What is the diet (including treats)? A record of this information is very critical when choosing an appropriate diet for a food trial (discussed later in this talk). What is the type of bedding? Has there been any exposure to wildlife?
Hereditary predispositions
Remember to take breed predisposition into account but do not let it close your mind to other possibilities. For example, Terriers, Labrador and Golden Retrievers, little white dogs and German shepherd dogs are often presented for allergic dermatitis. Boston Terriers, Bulldogs, Dobermans and others are more commonly diagnosed with demodectic mange but they can all pick up external parasites as easily as any other breed. Indeed, we are seeing many allergic Boston terriers and Bulldogs lately. Are there other pets in the litter affected? Charts of breed predispositions are very useful and can be found in many dermatology and genetic textbooks, and online on sites such as the dermatology FAQs on VIN and the University of Cambridge inherited diseases in dogs website (
"Securing and assessing the scene of the crime"
(Physical and dermatological examination)
The physical examination should start with a full general physical examination, and then proceed to a more specific dermatological examination. One must keep in mind that the skin is often a "window" into more generalized disease and not ignore the possibility of a more sinister underlying etiology. Palpate the lymph nodes. While most conditions that we see have a dermatopathic lymphadenomegaly, we have diagnosed lymphoma in some cases, which can predispose to demodicosis or even a pyoderma. What is the apparent general health of the pet? Does it appear to be in good body condition? Overweight? Distended abdomen? How does its weight compare to the last visit? It is not uncommon for patients with severe itchiness to actually present with weight loss.
The dermatologic exam includes a close exam of the whole skin surface, from the tip of the nose to the tip of the tail and the undercarriage. Concave pinnal erythema with normal ear canals or "peritympanic edema" (swelling just beside the eardrum) is suggestive (but not diagnostic) of an allergy. It may be a challenge to differentiate this from a loose pars flaccida. Palmoplantar dermatitis and caudal metacarpal alopecia is also a classical finding in allergic pets. Typical sites for scabies infestation include the pinnal margins, elbows, hocks and the ventrum. But don't be fooled. I have diagnosed scabies in patients presenting with only ventral abdominal pruritus. A pinnal-pedal reflex can be most informative; ninety five percent of patients with scabies have a positive pinnal pedal reflex but only 80% of patients with a pinnal pedal reflex will have scabies.
Owners will be inclined to show the veterinarian and technicians where he/she thinks are the important sites. These can often be the secondary, more traumatized sites, and offer less information. Shaving a "window" in the coat can help you look for "footprints" of a bacterial infection.
Identify and record the lesions. Dermatologists tend to annoy students by making them memorize terminology (what is a macule? What is a plaque?). There's good reason to do it. If you learn the terminology and can identify lesions, there are charts containing differential diagnoses and the most appropriate diagnostic tests for those lesions. (Ackerman 2008). All that's left is making them better!