Anesthesia for thoracic surgery (Proceedings)
Goals of this presentation are to identify physiologic and pathologic abnormalities that require attention in order to provide safe anesthesia in dogs and cats that have, or will be undergoing, penetration of the thoracic cavity.
Goals of this presentation are to identify physiologic and pathologic abnormalities that require attention in order to provide safe anesthesia in dogs and cats that have, or will be undergoing, penetration of the thoracic cavity. Conditions that may have specific considerations are traumatic injuries, such as auto collision or big dog-little dog syndrome, congenital abnormalities, such as patent ductus arteriosus (PDA) and persistent right aortic arch (PRAA), and pulmonary disease, such as pulmonary neoplasia, abscess, torsion, or chylothorax. Some of the anesthetic considerations relate to the patients' problems and some are problems resulting from opening the chest. A requirement common to all procedures is the need for adequate artificial ventilation by use of a mechanical ventilator or from a person dedicated to achieving manual ventilation.
Diaphragmatic rupture
All of the considerations of thoracotomy apply to anesthesia for repair of a ruptured diaphragm even though the surgical approach is a laparotomy. Furthermore, other problems are involved when the injury is recent, such as pulmonary contusions, possibility of a full stomach and risk of aspiration pneumonia, and skeletal fractures.
Preanesthetic evaluation must identify other effects of trauma. Thoracic radiographs will be needed to assess presence of pulmonary contusions, pneumothorax, pleural fluid (blood), and to identify the structures in the chest. Physical examination includes search for evidence of head trauma, such as cranial fractures and scleral hemorrhage. Significance of preanesthetic findings are listed in Table 1.
Table 1. Preanesthetic evaluation for anesthesia for ruptured diaphragm.
Specific cautions
There are four areas of concern during anesthesia for repair of ruptured diaphragm (Summary in Table 2). Depth of breathing may severely decrease immediately after induction of anesthesia and the patient will require artificial ventilation. Inspiratory pressure should initially be limited to less than 25 cm H2O to avoid barotrauma. Ventilation with the usual parameters of 12 breaths/min and volume per breath of 15 ml/kg may have to be altered in patients with stiff lungs to 20 breaths/min and 11 ml/kg. Hypoxemia may develop with the animal in one position but resolve when the patient position is changed, for example, to the opposite lateral recumbency or moved from dorsal recumbency to a tilted oblique position.
Hypotension can develop any time after induction of anesthesia but specifically may occur during surgery when the abdominal organs are retrieved from the thoracic cavity. The probable mechanism is vasodilation in the abdominal organs resulting in sequestration of blood. Treatment with a large bolus of crystalloid fluid is not advisable as hypervolemia may later induce pulmonary edema. Management of low blood pressure in this situation is best with an IV infusion of vasoactive agent such as dobutamine or dopamine, 5-7 micrograms/kg/min, or ephedrine, 0.06 mg/kg bolus IV. Dopamine and ephedrine release norepinephrine and may increase the frequency of ventricular premature depolarizations.
Reexpansion pulmonary edema develops when forceful ventilations during anesthesia are used to rapidly expand lung that has been collapsed for 12 hours or more. The local pressure imposed in order to expand totally collapsed alveoli results in cytokine release. These mediators perfuse the lungs and alter capillary permeability resulting in pulmonary edema. In severe cases, the dog or cat will be unable to maintain adequate oxygenation even when breathing 100% oxygen, and the animal dies. Prevention lies in making no specific effort to re-expand the lung. The lung will progressively re-expand with time.
Table 2: Specific cautions during anesthesia for diaphragmatic rupture
Anesthetic protocols
The choice of anesthetic agents must be made after listing the specific problems of the individual patient as agents may have to be ruled out. Although this author most frequently includes an anticholinergic agent in premedication of healthy patients, these agents would most likely be omitted in patients with pulmonary and myocardial contusions to avoid increased heart rates and potentiation of ventricular dysrhythmias.
Premedication should not be heavy because of respiratory depression, unless incorporated into the induction of anesthesia sequence. Buprenorphine, 0.01 mg/kg, or butorphanol, 0.2-0.4 mg/kg, IM are good premedicants for cats, followed by induction of anesthesia with diazepam or midazolam, 0.25 mg/kg, with ketamine, 5 mg/kg, given IV in increments 'to effect' and maintenance of anesthesia with isoflurane or sevoflurane. Duration of action of butorphanol is not much longer than one hour, and a supplement of butorphanol, 0.2 mg/kg, may be needed at that time.
Hydromorphone or oxymorphone, 0.05-0.1 mg/kg IM or IV, are good analgesic agents for dogs but may induce vomiting. Vomition may cause adverse effects when the stomach or intestines are in the thoracic cavity and these opioids are better administered after induction of anesthesia. The patient should not be premedicated with butorphanol or buprenorphine if you plan to use a mu receptor agonist opioid intraoperatively. Buprenorphine will decrease the effectiveness of a pure mu receptor opioid for more than 6 hours after administration. Hydromorphone or oxymorphone can be used in cats but frequently cause dysphoria when heavy sedation is not used simultaneously. Diazepam/midazolam-ketamine is a useful induction agent in dogs with diaphragmatic rupture. Propofol can be used for induction of anesthesia but induces hypotension and increases the irritability of the myocardium particularly in patients with traumatic myocarditis.
Dogs and cats with severe myocardial bruising may be anesthetized with etomidate rather than ketamine. Etomidate causes no cardiac depression and does not increase heart rate, unlike ketamine. Etomidate is used for induction of anesthesia, frequently with diazepam or midazolam (separate syringes, not mixed as with ketamine). The method of administration and clinical signs are similar to use of thiopental and propofol. Dose rate of etomidate in cats and small dogs is 1 – 1.5 mg/kg and less in larger dogs, 0.5-1.0 mg/kg IV. Continuous administration of etomidate is not recommended as dose rates over 2.5 mg/kg are immunosuppressive.
An alternative protocol favored by some for use in sick dogs is induction of anesthesia with fentanyl and diazepam or midazolam, and maintenance of anesthesia with isoflurane or sevoflurane. Fentanyl, 6-10 micrograms/kg, and diazepam or midazolam, 0.25 mg/kg, are drawn up in separate syringes. One-quarter to one-third of each drug is administered IV, flushing the catheter between drugs, and the patient observed for 30-60 sec before an additional increment is administered. The drugs are titrated until there is sufficient jaw relaxation for tracheal intubation to be accomplished. The dogs may responsive to loud noises and swallowing may be observed during intubation. Fentanyl has a short duration of action, 20 minutes after IV administration, and analgesia must be continued by IV infusion of fentanyl, 6 micrograms/kg/hr, or small supplements of hydromorphone or oxymorphone.
Oxygen supplementation
Preoxygenation is recommended for dogs and cats with thoracic disease. This involves administration of oxygen by mask for 2-3 minutes before induction and during induction of anesthesia. The rationale is that induction of anesthesia is accompanied by onset of respiratory depression, occasionally apnea, and increasing the tissue level of oxygen first will avoid hypoxemia.
Oxygen supplementation is recommended for several hours after anesthesia until the residual effects of the inhalant anesthesia are gone. Oxygen can be supplied with an oxygen cage or through a nasal tube(s) placed before recovery from anesthesia and metered at 100 ml O2/kg/min. The effects of laparotomy and thoracic surgery have been demonstrated in humans to result in decreased lung function for 1-2 weeks. Lung vital capacity is decreased 25-50% after abdominal surgery and tidal volume is decreased by 20%, gradually increasing to normal in 2 weeks.
Lidocaine
Lidocaine can be administered to dogs to diminish ventricular dysrhythmias and improve blood pressure when those dysrhythmias are decreasing cardiac output. It is also possible that lidocaine administered during surgery will prevent plasticity of spinal cord neurons in response to nociceptive stimuli and, even though discontinued at the end of anesthesia, improve comfort of the patient in the next 2-3 days. The loading dose of lidocaine is 1-2 mg/kg and can be given before or after induction of anesthesia. Blood levels of lidocaine are maintained by a constant infusion of lidocaine, 0.025-0.05 mg/kg/min. Lidocaine can be administered direct from a syringe using a syringe pump or in diluted form, 1 mg/ml, by adding 500 mg lidocaine to 500 ml 0.9% saline and using a fluid administration set. Continuous IV infusion of lidocaine provides some sedation and may decrease the requirement for isoflurane or sevoflurane by 20-30%. Lidocaine infusion is not usually recommended for cats.
Lateral Chest Thoracotomy
Anesthesia for thoracotomy involves more than just choice of anesthetic agents. Controlled ventilation must be maintained in the face of decreased lung volume from surgical manipulation of lung lobes or intrathoracic space occupying mass or impaired gas exchange from pneumonia. Multimodal analgesia is recommended to ensure patient comfort. Two or more of the following techniques can be combined in the same patient: IM or IV opioid, IV lidocaine, opioid epidural nerve block, intercostal nerve blocks, and interpleural bupivacaine block. Anesthetic considerations of the specific disease or surgical problem may impose further limits on management.
Intercostal nerve blocks are achieved by injection of a bleb of bupivacaine caudal to the heads of the two ribs cranial to the surgical incision site and two ribs caudal to the site. The nerve runs adjacent to blood vessels and therefore aspiration should always precede injection of local anesthetic. The total injected volume should not exceed 2.5 mg/kg in dogs and 1.5-2.0 mg/kg in cats. This volume can be split between the intercostal blocks and interpleural instillation.
Interpleural nerve block is performed at the end of surgery either immediately before closure of the incision or by administration through the chest tube. Bupivacaine, 1.5 mg/kg, is instilled into the pleural cavity. Analgesia of the thoracic wall is most complete when the animal is in dorsal recumbency because the bupivacaine flows by gravity towards the spine and blocks the intercostal nerves near their origins. Instillation of bupivacaine down a chest tube with the surgical side uppermost results in local pleural analgesia and reduces discomfort from friction of the chest tube during breathing.
Tips for anesthesia for thoracotomy
1. Negative pressure in the pleural cavity is abolished when the thorax is surgically incised. Consequently the rib cage enlarges such that the lungs may not reach the surgical excision during inspiration even when inflation is adequate and ventilation is satisfactory.
2. Pressure required for adequate lung inflation will be lower when the thorax is open than before thoracotomy.
3. Lung lobes that have been packed off during the surgical procedure may be gently re-expanded when replaced into the normal position. The duration of lung collapse is short and reinflation does not induce the same problem as encountered with diaphragmatic hernia repair.
4. Trapped air in the thorax during closure of the surgical incision can cause a tension pneumothorax, hypoxia and hypotension. Leaving the chest tube uncapped during closure provides insufficient room for air flow during lung inflation. The chest tube should be plugged and air aspirated before closure of subcutaneous tissue and skin.
5. Circumferential bandages applied to anesthetized patients frequently are too tight and cause hypoxemia during recovery.
6. Lobectomy may result in bleeding into the bronchus and blood clots can occlude the endotracheal tube.
Patent Ductus Arteriosus (PDA)
Specific points about PDA physiology that influence anesthetic management are
1. Mean arterial pressure is low because the diastolic pressure is low.
2. Ligation induces pressure changes that acutely increase diastolic pressure (Fig. 1).
Figure 1
3. Mature dogs with PDA are likely to have left atrial and left ventricular enlargement, pulmonary hypertension and edema.
Anesthesia in animals with a PDA can be expected to be accompanied by hypotension. Consequently, the best combination of agents chosen is one causing least depression of contractility and least impact on peripheral vascular tone and the drugs should be administered incrementally and in small doses. Fluid restriction is practiced to avoid pulmonary edema after ligation. Intraoperative fluid administration is limited to 6 ml/kg/h and hypotension is not treated by fluid boluses. Dobutamine or dopamine, 5-7 micrograms/kg/h, is infused to maintain mean arterial pressure above 60 mm Hg. Patients ≤ 3 months of age should receive 5% dextrose during anesthesia at 3 ml/kg/h with balanced electrolyte solution at 3 ml/kg/h.
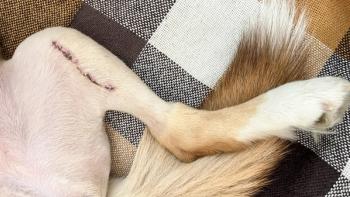
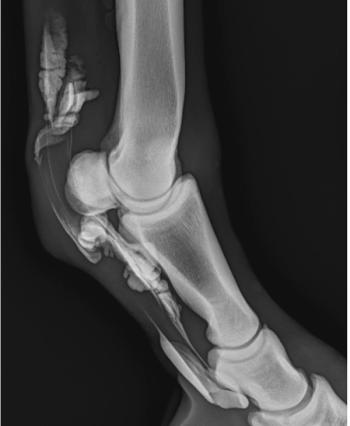
Big dog-Little dog Syndrome
Skin wounds or bruising over the thorax may be external signs of thoracic wall penetration. The potential for pneumothorax should be incorporated into the anesthetic management plan until the wounds have been thoroughly investigated.
Dogs that have been picked up by their necks and shaken may have spinal cord damage and swelling. This not infrequently is accompanied by decreased respiratory muscle function, hypoventilation, and hypoxia when breathing air. The addition of anesthetic agents may result in life-threatening respiratory depression.