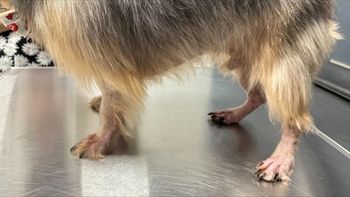
Alopecia in cats–Is it on their heads or on their skin? (Proceedings)
Behavior and medicine (or physiology) are not mutually exclusive; there is a complex interaction between the two. Studies published recently in the British Journal of Dermatology concluded that human patients subjected to brief psychological stress (PS) developed an increase in Psoriasis Area and Severity Index (PASI) and itch 4 weeks later(Verhoeven, 2009).
The connection between the brain and the skin
Behavior and medicine (or physiology) are not mutually exclusive; there is a complex interaction between the two. Studies published recently in the British Journal of Dermatology concluded that human patients subjected to brief psychological stress (PS) developed an increase in Psoriasis Area and Severity Index (PASI) and itch 4 weeks later(Verhoeven, 2009). There was a significant psychological-stress induced increase in cytotoxic CD8+ T lymphocytes in patients with psoriasis when compared to healthy volunteers (Schmid-Ott, 2009). Stress is also believed to exacerbate atopic dermatitis in humans. Psychological stress decreases epidermal proliferation and differentiation. It impairs epidermal permeability barrier homeostasis, and decreases stratum corneum return to integrity, as measured by trans epidermal water loss (TEWL), in much the same way as exogenous glucocorticoids (Denda 1998, 2000). This is an interesting finding, given the role that barrier function plays in the pathomechanism of atopic dermatitis.
In mice, stress induces nerve growth factor and substance P-dependent neurogenic inflammation. Sound stress induced dendritic cell (DC) maturation and up-regulated intercellular adhesion molecule-1 (ICAM-1) expression. Blocking of ICAM-1/leukocyte function-associated antigen-1 interactions significantly abrogated the stress-induced numeric increase, maturation, and migration of dermal DCs in vivo and also reduced stress induced keratinocyte apoptosis and endothelial cell expression of ICAM-1 (Joachim 2008)
Alopecia in cats may be a result of an array of medical disorders. Medical problems can turn into behavioral conditions; regardless of the underlying cause, self-induced alopecia may progress to a compulsive disorder in cats. On the other hand, feline self-trauma leading to hair loss may be a consequence of displacement behavior that may arise from environmental and social stressors or situations causing conflict, frustration, or anxiety. It is easy to find some environmental stressor that could serve as the "trigger" that initiated a behavior in virtually any patient, but the mere presence of an event does not make for a diagnosis.
Behavior and medical diseases may have different underlying etiologies and yet coexist; there is no rule that an individual with a compulsive disorder can't also suffer from environmental allergies.
And so the challenge is in deciding whether any skin condition is medical leading to behavioral, behavioral leading to medical, primarily behavioral or primarily medical. The diagnosis in the feline patient that is self-traumatizing can therefore be a daunting task.
Feline alopecia – is it on their skin or in their head?
The medical approach
A comprehensive medical approach is required to make a definitive diagnosis before diagnosing virtually any behavioral condition. Cost concerns (especially in the current economic environment) and owner compliance may limit testing in some instances so that a presumptive, rather than a definitive, diagnosis is made. While this is especially true for the family veterinarian, referral practitioners can also fall into the trap of leaping to a diagnosis. Because of this, veterinarians may accidentally misdiagnose some cats as having a behavioral etiology, when in fact there is a medical cause.
The study
Psychogenic alopecia is a diagnosis of exclusion. A clinical trial was performed in our dermatology and behavior referral practice on cats that were suspected of having psychogenic alopecia by their family veterinarian (Waisglass 2006). Although the incidence of psychogenic alopecia in cats is unknown, we hypothesized that the condition is over-diagnosed.
Cats were only entered into the trial if there was hair loss in the absence of any primary lesions (other than self-excoriation), if the problem was continually present for at least 6 months, and if there was no obvious evidence of parasites. Cats with head and neck lesions were excluded due to the high prevalence of adverse food reactions in these patients. Each cat was first assessed by a veterinary behaviorist (GML), to determine whether the pet had behaviors that were consistent with psychogenic alopecia. Then the cats were transferred to the author for dermatological evaluation. Each cat was first examined and photographed and anal sacs were expressed (not the most fun part of the study!). For each cat, a trichogram, CBC, biochemical profile with thyroid, FELV/FIV testing, urinalysis, fungal culture and skin scraping were performed. Skin biopsy specimens were collected and submitted (blindly – i.e. without history) to a dermatohistopathologist. If there were no abnormal findings at the first visit, each cat was treated with selamectin (Revolution™) and a food trial of minimum 8 weeks duration was performed (Hills prescription diet Z/D low allergen™). If the cat improved significantly, it was challenged with its regular food. If there was no or partial improvement, the cat was then treated with steroids (a "steroid response trial") to rule out an unidentified pruritus (such as environmental hypersensitivity). We chose up to 2 injections of Depomedrol to ensure client (and patient) compliance. Allergy tests were not performed as the goal of the study was to determine whether the cats were self-traumatizing due to pruritus; a positive allergy test does not prove that the self-trauma is a result of allergies.
One might wonder about a potential "calming" effect of steroids on behavior? We considered this possibility but were unable to find good documentation to support this contention. Indeed, a recent study looked at the effects of corticosteroids in dogs. Dogs that were treated with either methylprednisolone, prednisolone, or dexamethasone were reported to have nervousness, restlessness, an increase in startle responses, food guarding, decreased activity, irritation related aggression, increased avoidance response and increased barking.(Notari 2009). Steroids would be unlikely to ameliorate an anxiety or compulsive disorder. Indeed, one might expect that if steroids affected compulsive or anxiety related disorders in people, psychiatrists would be treating their patients with steroids rather than anti-obsessional or anxiolytic drugs.
Using this protocol, of 21 cases, 16 (76.2%) had a medical etiology, 2 (9.5%) were psychogenic alopecia and 3 (14.3%) were combined medical and behavioral. If we assume that the steroid responsive patients were environmentally allergic, then of the medical problems, a combination of environment and adverse food reactions were most common, followed by adverse food reactions alone, environment alone, and parasitic hypersensitivity.
In their skin
Specifically, medical conditions identified in these cats were concurrent adverse food reaction plus environmental hypersensitivity (5), adverse food reaction (4), hypersensitivity of undetermined cause (2), concurrent adverse food reaction, environmental hypersensitivity and flea allergy dermatitis (1), environmental hypersensitivity alone (1), parasitic dermatosis (i.e., clinical response to parasiticide administration (1), parasitic dermatosis and bacterial dermatitis (1), and parasitic dermatosis and hyperthyroidism (1). Fifty-two percent of the patients had more than one factor that was contributing to the self trauma. Skin biopsy specimens were obtained from 20 of the 21 cats, and 14 of the 20 (70%) had inflammatory skin lesions. There was no indication in any of the specimens of an endocrinopathy. All cats with histological evidence of inflammation had a medical condition associated with pruritus. No histological abnormalities were seen in skin biopsy specimens from 6 cats. Of these cats, 2 had a compulsive disorder and 4 had an adverse food reaction, environmental hypersensitivity, or both. Therefore, while biopsy results were helpful (in that an inflammatory response was found in most medical cases), there were a number of cats with histologically normal skin that also had a medical cause.
In their head?
A diagnosis of psychogenic alopecia should made only if primary dermatologic and other medical conditions have first been thoroughly ruled out. Hair loss was determined to be entirely psychogenic in only 2 of the 21 cats in our study. These were considered to be a result of a compulsive disorder whereby behaviors are exhibited independent of the original context and have no apparent goal. They can be repetitive, exaggerated, sustained, or so intense that they might be difficult to interrupt. The rationale for identifying these behaviors as compulsive or obsessive-compulsive is that they resemble compulsive disorders identified in humans such as repetitive hand washing, in regard to clinical appearance and response to neuropharmacologic agents. Although the pathophysiology of compulsive disorders is not entirely understood, an underlying alteration in neurotransmitters is a likely factor, and pharmacologic intervention is often needed. Alterations in β-endorphins, dopamine, and serotonin have all been implicated in compulsive disorders, primarily on the basis of response to treatment, but abnormal serotonin metabolism has been suggested to be the primary mechanism by which these disorders are induced(Landsberg 2003). In fact, drugs that inhibit serotonin reuptake (e.g., clomipramine and fluoxetine) have been shown to be most effective in the treatment of cats and dogs with compulsive disorders, and direct evidence of serotonin involvement has been identified. (Luescher 2003, Wynchank 1998, Rapaport 1992, Hewson1998; Vanderbroek 1995). Trichotillomania in humans is an impulse control disorder and could be an alternative explanation for these behaviors in pets.
In their head and in their skin
In 3 of the 21 cats, a behavioral component was identified in addition to a medical condition (environmental hypersensitivity in 1 cat, adverse food reaction in 1 cat, and concurrent environment and adverse food reaction in 1 cat). Medical conditions can lead to stress and anxiety and associated behavior problems (e.g. self-trauma, predisposition to development of a compulsive disorder). In fact, anxiety might contribute to pruritus in humans, since stress can lead to an increase in cytokines, release of opioids, serotonin and other vasoactive peptides, especially in atopic individuals (Raap 2003, Buske-Kirschbaum 2002, Koblenzer 1999, Panconesi1996)
The hypothesis for the pathogenesis of canine (and human) atopic dermatitis is that an epidermal barrier defect could facilitate the contact of environmental allergens and microbes with epidermal immune cells at skin sites. As mentioned above, a link has also been found between stress and an impairment of epidermal barrier homeostasis. One might hypothesize that stress could therefore exacerbate atopy. Put another way, might the "uptight atopic pet" have a lower threshold to the discomfort, a barrier defect and a stress induced barrier recovery defect that exacerbates or extends the duration of the condition? Opioid peptides released during stress may even further potentiate pruritus.
Genetics
Genetics may play a role in the expression of displacement and compulsive behaviors in certain cats. For example, psychogenic alopecia has been reported to be more common in the Oriental breeds. Interestingly, 3 of the 5 cats with psychogenic alopecia in the present study were Oriental breeds or their crosses. Alternatively, Siamese and their crosses may also be predisposed to adverse food reactions, which might have a similar pattern of hair loss, further complicating the diagnostic process (Scott 2001)
Key clinical diagnostic points
• Many cats presented with feline alopecia have an adverse food reaction as part of their condition
• In many cases, the underlying causes are multifactorial
• A normal skin biopsy does not rule out a medical cause of the self trauma
• It is possible to have both a medical and behavioral problem, and both need to be addressed for successful management
• Psychogenic alopecia is over diagnosed (cost playing a role?)
• Minimal diagnostic tests for self induced alopecia should include:
o skin scraping
o fungal culture
o anal sac expression
o trichogram (will help confirm that the hairs are broken, and "fuzzy" hairs are suspicious of dermatophytosis)
o CBC, FELV/FIV
o parasiticide response trial
o food trial
o steroid treatment response trial
• Additional diagnostic tests could include, if warranted
o biochemical profile with thyroid
o urinalysis
o scoping (IBD?)
o skin biopsy (particularly useful to differentiate alopecia secondary to hair loss as opposed to self-trauma)
Therapy
Medical therapy
Medical therapy should be directed against the underlying etiology, of course. Fungal disease should be eliminated. Parasites must be well controlled. When an adverse food reaction is identified, the ideal treatment would include identification of the particular offending ingredient(s) and its avoidance. As multiple etiologies often play a role, one may need to control the environmental component while concurrently managing the diet. If the patient suffers from "catopy", allergy testing can be considered. Allergen specific immunotherapy, steroids and cyclosporine are the mainstay treatments for many of these patients. Whenever possible, I use oral steroids in lieu of injectable steroids in the treatment of pruritus. I believe that I get a better response to prednisolone when compared to prednisone in cats. Indeed, better bioavailability has been reported. I have found that antihistamines have a role to play in some patients with "catopy". Like fatty acids, they can help to decrease doses of the more offensive therapies. However, I don't find that antihistamines do a good job of "putting out the fire", and I use these products to hold the patients once steroids are on board or to help reduce the steroid dose or frequency.
Behavioral therapy
Patients with true psychogenic alopecia need behavioral therapy. As is the case for all behavioral conditions it isn't only about drugs. One needs to consider the possibility of an underlying stressor as an initiating or perpetuating factor and so it is important to decrease stress. As with zoo animals, enrichment leads to decreased stress and decreased stereotypic behaviors. Further information can be found in the Feline Behavior Guidelines from the American Association of Feline Practitioners:
(
Important behavioral therapy concepts:
• Working for food – multiple canned meals, hiding dry food in toys, higher protein diets to more simulate "canned mouse"
• Increase playing opportunities
• Household enrichment – perches, places to explore, provide a regular sleeping area
• Feliway (cat facial pheromones)
Drugs should be a last resort but may be needed if the condition has progressed to a compulsive disorder (where a "loop is set-up"), at least in the beginning. Clomipramine is a good option in most cases. Once all the hair is back (and if all abnormal licking seems to have ceased), continue the environmental treatment and the Feliway and then (if you do sufficient behavior therapy and treat any concurrent medical) try to get the cats off medication. Anxiety induced alopecia and those where the initiating factors are under control might stay improved, but a compulsive disorder (especially if there is a genetic component) may need long term drugs. Clomipramine should be avoided in cardiac cases or cats with potential for urinary tract obstructions. Fluoxetine may be preferred in this cases.
In our study, the alopecia improved dramatically in the 2 PA cats with a combination of behavioral management (primarily consisting of a more predictable daily routine with attention to increasing enrichment through social play sessions and introduction of new play toys) and clomipramine treatment. One of the cats also had hyperesthesia, which improved dramatically with treatment. Of the 3 cats with partial psychogenic alopecia, 1 responded to behavioral management, 1 was lost to follow-up, and 1 was not treated.
Space limitations for the proceedings did not allow for inclusion of references. However, they are available upon request. Please feel free to email me at