Identifying and treating anal sac adenocarcinoma in dogs
Early detection and aggressive treatment are essential in the successful management of this tumor.
Anal sac adenocarcinoma is reported to represent 2% of all skin tumors and 17% of perianal tumors in dogs.1,2 So although it is an uncommon tumor, it is locally invasive and has a high rate of metastasis to the draining iliac lymph nodes, making early diagnosis and treatment essential for long-term control. Hypercalcemia of malignancy is seen in some cases as a paraneoplastic syndrome and may contribute to presenting clinical signs.
Early detection and aggressive treatment are essential in the successful management of this tumor, which emphasizes the importance of a rectal examination as part of a routine physical examination in all animals. Treatment typically requires a multimodal approach involving surgery, radiation, and, potentially, chemotherapy.
SIGNALMENT AND CLINICAL PRESENTATION
Anal sac adenocarcinoma occurs primarily in older dogs, with an average age of 10.5 years.2 Historically, female dogs were reported to be predisposed to anal sac adenocarcinoma.3 However, most recent retrospective studies have shown an equal sex distribution between spayed females and castrated males.2,4-8 Interestingly, a study of 810 British dogs with anal sac adenocarcinoma found that intact males were less likely to develop this tumor, suggesting a possible protective effect of testosterone.9 Several breeds have been reported as overrepresented, including cocker spaniels, springer spaniels, German shepherds, dachshunds, and Alaskan malamutes.2
Owners or groomers may be the first to notice perineal swelling or discomfort. The primary anal sac mass or enlarged iliac lymph nodes may cause constipation, obstipation, tenesmus, dyschezia, or ribbonlike stools. Earlier clinical signs are not always noticed by owners but can include scooting and excessive licking of the perineal area. Polyuria, polydipsia, anorexia, and lethargy can be seen secondary to hypercalcemia of malignancy, a common sequela of anal sac adenocarcinoma, although not all dogs with hypercalcemia will display such clinical signs. Anal sac adenocarcinoma can also be an incidental finding on rectal examination in a high proportion of affected dogs.8 On occasion, the anal sac mass may be small compared with the size of the metastatic iliac lymph nodes, so an abdominal ultrasonographic examination with careful attention to the sublumbar area is recommended when an anal sac mass is palpated or in cases of hypercalcemia of unknown origin.8
In most cases, a physical examination will reveal a perianal mass associated with one or both anal sacs. Occasionally, a mass may not be appreciated externally, so a thorough digital rectal examination is advised in all dogs. Enlarged iliac lymph nodes may be palpable on rectal examination in cases of metastatic or reactive lymphadenopathy, but this enlargement can be difficult to detect in larger dogs or in cases in which the enlargement is subtle.
DIAGNOSTIC TESTING AND STAGING
The recommended work-up for a dog with an anal sac mass includes a minimum database (complete blood count, serum chemistry profile, urinalysis) to assess the animal's overall health and identify whether paraneoplastic hypercalcemia is present. Hypercalcemia, caused by tumor secretion of parathyroid hormone-related protein (PTH-rP), is seen in 26% to 53% of cases.4,7,8 Anal sac adenocarcinoma is the second most common neoplastic cause of hypercalcemia, so a thorough digital rectal examination is indicated in all dogs in which hypercalcemia is noted.10
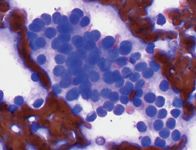
1A. Cytologic examination of a fine-needle aspirate of an anal sac adenocarcinoma reveals clustering of the cuboidal cells and indistinct cellular borders. Anal sac adenocarcinoma cells typically lack overt criteria of malignancy (Wright's-Giemsa; 50x). (Photo courtesy of Joyce Knoll, VMD, PhD, DACVP.)
A fine-needle aspirate and cytologic examination of an anal sac mass can differentiate anal sac adenocarcinoma from other tumor types that may occur in this area (i.e. mast cell tumor, melanoma, lymphoma). Typically, sheets of clumped cuboidal epithelial cells with indistinct cellular borders are seen (Figure 1A). Despite this tumor's aggressive biologic behavior, the cytologic appearance of the cells can be benign, with few criteria of malignancy apparent. Suppurative inflammation or necrosis identified in cytologic specimens can be misleading since tumors can be secondarily infected. In such cases, obtain a biopsy after appropriate antibiotic therapy.1 Biopsy may also be needed to distinguish between epithelial tumors involving the circumanal glands and apocrine glands of the anal sacs (Figure 1B). However, a lesion at the site of an anal sac often increases clinical suspicion of the tumor type.
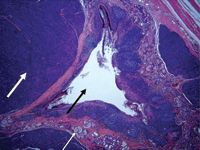
1B. Histologic section of adenocarcinoma of the apocrine gland of the anal sac. The lumen of the anal sac is in the center (black arrow), immediately surrounded by lymphocytic inflammation and clusters of normal apocrine glands (thin white arrow). Normal architecture to the left and far right is effaced by the lobulated adenocarcinoma (thick white arrow) (hematoxylin-eosin; 20x). (Photo courtesy of John H. Keating, DVM, DACVP.)
Staging tests include abdominal ultrasonographic and three-view thoracic radiographic examinations. Evidence of local spread to the iliac lymph nodes is common, occurring in 40% to 72% of cases at presentation.3-8 This metastasis to the iliac lymph nodes can occur early in the course of disease while the anal sac tumor is still quite small.8 Lateral abdominal radiographic findings can suggest a soft tissue opacity in the sublumbar region, causing ventral deviation of the colon. Abdominal ultrasonography has higher sensitivity than does radiography in detecting iliac lymphadenopathy and can better characterize the number and size of lymph nodes and evaluate the remainder of the abdomen for evidence of distant metastatic disease (Figure 2).1 Pulmonary metastatic disease occurs less commonly and can be identified as a nodular or diffuse pattern on thoracic radiographs.1 Other uncommon sites of metastasis include the spleen, liver, and lumbar spine.4 The information gathered during staging will help guide treatment and formulate a prognosis.
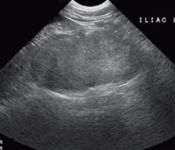
2. The ultrasonographic appearance of iliac lymphadenopathy due to metastatic anal sac adenocarcinoma in a dog.
TREATMENT
Because anal sac adenocarcinoma has a high rate of local metastasis and a locally invasive nature, a multimodal approach to treatment is typically recommended. The benefit of surgery and radiation has been shown in retrospective studies, while the role of chemotherapy is less clearly defined.
Medical management of hypercalcemia
The clinical significance of hypercalcemia related to anal sac adenocarcinoma is not well-characterized. In most cases, this paraneoplastic syndrome resolves once the tumor is surgically removed.3 However, long-term complications of persistent hypercalcemia in dogs with unresectable disease are not well-established, and, in our experience, these dogs have not developed evidence of renal compromise. Nevertheless, judicious monitoring of blood urea nitrogen and creatinine concentrations and urine specific gravity in hypercalcemic dogs with anal sac adenocarcinoma is warranted, and treatment of hypercalcemia should be instituted at the discretion of the attending veterinarian. Immediate care may include sodium chloride diuresis along with furosemide. Bisphosphonate therapy may also be considered. Corticosteroids may be used once lymphoma has been ruled out as a cause of hypercalcemia.1
Surgery
When technically feasible, surgery is the initial treatment of choice for anal sac adenocarcinoma limited to the primary tumor and local lymph nodes. Surgery may also be indicated in dogs with distant metastatic disease as a palliative measure if the tumor is causing clinical signs. The primary mass should be surgically resected with the intent of complete excision. Because of the tumor's local infiltration, location, and large size at presentation, an aggressive surgery with wide margins often is not possible. Fecal incontinence is a potential complication, which can be temporary or permanent. Other postoperative complications include wound infection, which can result in dehiscence or sepsis, hypocalcemia, and perianal fistula formation.3,8 Early surgical intervention is important, as the masses can be fast-growing, and a window of opportunity may be missed if the mass becomes inoperable. In dogs with hypercalcemia, even incomplete resection can lead to normalization of calcium concentrations postoperatively.3
If the iliac lymph nodes are enlarged, an exploratory laparotomy should be performed for assessment and resection if possible. In cases of hypercalcemia, the tumor cells within the lymph node can secrete PTH-rP, so primary tumor resection alone may not result in normocalcemia. Additionally, enlarged lymph nodes that are not surgically removed will continue to grow and eventually will likely result in obstipation and tenesmus.
Two small case series reported lymphadenectomy and excision of the primary tumor in four and five dogs, with a mean survival of three years in the first series and a median survival of 20.6 months in the second series; two dogs were still alive at 19 and 54 months.11,12 No surgical complications were noted in any of the cases. Another retrospective study found a significant survival advantage in dogs with anal sac gland carcinoma that underwent primary tumor removal and lymph node removal compared with dogs whose metastatic lymph nodes were not removed.6 The lymph nodes may be easily resected in some cases, but they can also be friable and invade the large blood vessels that surround them. Referral to a board-certified surgeon is advised for lymphadenectomy because of the difficult location and potential complications. Fatal hemorrhage is possible, and neurologic damage can lead to transient or irreversible urinary incontinence.3,4 In a few cases in which complete resection is possible, adjuvant treatment may not be required to attain long-term survival, but more data are needed to determine whether recurrence or metastasis develops in dogs treated with surgery alone.6
Routine postoperative management includes patient-appropriate analgesia with opiates and nonsteroidal anti-inflammatory drugs. Hypercalcemia usually resolves within 24 hours. Food can be introduced within eight to 12 hours of surgery, and a stool softener can be added to the food for two or three weeks. The dog should wear an Elizabethan collar to prevent self-trauma to the surgical site and be rechecked two weeks after surgery for fecal incontinence or anal stricture.
Because of the difficult location of the tumor and local invasiveness, marginal resection is often performed, and recurrence is common, reported in 45% to 50% of dogs.3,4 Adjuvant treatment is recommended in cases of marginal excision to increase local control and decrease the risk of recurrence.
Radiation therapy
Radiation therapy can be used preoperatively or postoperatively or palliatively as the sole method of treatment.
Preoperative. The goal of preoperative radiation is to kill tumor cells existing as microscopic extensions at the tumor periphery, which increases a surgeon's ability to obtain clean margins. Radiation may also shrink the tumor, thereby increasing the ease of surgical resection. The total dose delivered to the region is decreased in preoperative radiation to prevent healing complications with the intended future surgery. At our hospital, preoperative megavoltage radiation therapy consists of 22 daily fractions of 2.5 Gy, compared with 24 daily fractions of 2.5 Gy for postoperative radiation. Surgery can be performed when the acute radiation side effects have healed, typically within two to four weeks.
Postoperative. Postoperative radiation is used in cases in which clean margins are not obtained with surgery. Radiation is started at suture removal, when the surgical incision has healed, and is administered over a course of three to five weeks. Radiation to the lymph node bed should also be considered after iliac lymph node resection in which disease breaches the capsule since a margin of normal tissue cannot be obtained in this location. The lymph node bed may also be radiated prophylactically in patients that did not have enlarged lymph nodes at presentation since that is the most common location for the development of future metastatic disease.7
Definitive radiation can also be used to treat metastatic lymph nodes that could not be resected at surgery in hopes of decreasing their size and slowing growth for an extended period. In one study, three dogs with anal sac adenocarcinoma had 15 daily fractions of 3.2 Gy of megavoltage radiation therapy to enlarged iliac lymph nodes.7 Two dogs were reevaluated with abdominal ultrasonography: one had complete resolution of the enlarged lymph nodes for two years, and the other dog had one enlarged lymph node that completely responded and another node that reduced in size by more than 50%.7
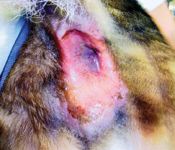
3A. Typical radiation-induced moist desquamation two weeks after completion of 24 fractions of 2.5 Gy to the perineum after incomplete resection of anal sac adenocarcinoma.
Complications. Because of the location of anal sac adenocarcinoma and the iliac lymph nodes, many sensitive normal tissues, including the perineal skin, anus, rectum, and colon, may receive unavoidable radiation, and, consequently, side effects can be severe preoperatively and postoperatively. Acute complications that occur during and several weeks after treatment include colitis, tenesmus, moist desquamation of the perineal skin, and perineal discomfort (Figure 3A).7,8 Topical treatments (vitamin E, aloe, commercially available radiation creams), Elizabethan collars, and intensive pain management are required in most cases. Antibiotics may be required to treat secondary skin infections in some patients. Colitis can be managed with fiber supplementation and metronidazole. The side effects are typically self-limiting and resolve several weeks after radiation is finished (Figure 3B).
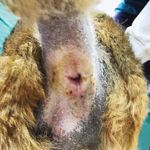
3B. The same dog as in Figure 3A one month later showing resolution of the erythema and moist desquamation.
Late complications occur months to years after radiation therapy and may present as chronic problems such as chronic diarrhea, chronic tenesmus, rectal stricture, fecal incontinence, and colonic perforation.13 The use of smaller fractions of radiation per dose is associated with a lower risk of these complications.13
Treatment failure is another complication, defined as regrowth of a tumor or lymph node in the area of previous radiation. In a study of 15 dogs with anal sac adenocarcinoma treated with surgery, radiation, and mitoxantrone chemotherapy, four dogs developed recurrence within the radiation field.7
Palliative. Radiation can also be used as a palliative treatment in dogs that are not candidates for definitive treatment with surgery and radiation. Palliative or hypofractionated radiation therapy typically consists of larger doses (6 to 8 Gy) of radiation given weekly for three or four weeks. The goal of this therapy is to provide a good quality of life by relieving clinical signs associated with the anal sac mass or enlarged iliac lymph nodes for a limited amount of time. Palliative radiation therapy is often used in patients with a guarded prognosis due to distant metastatic disease, extensive local disease, or concurrent illnesses. Also, some owners may decline definitive treatment because of cost, time commitment, or concerns about morbidity. In our experience, partial regression or stabilization of tumor size with alleviation of clinical signs is achieved in about three quarters of cases treated with hypofractionated megavoltage radiation therapy (Figures 4A & 4B).

4A. A lateral caudal abdominal radiograph of a dog with anal sac adenocarcinoma and metastatic iliac lymphadenopathy. The enlarged iliac lymph nodes can be seen and are causing ventral deviation and partial obstruction of the colon. (The pellet was an incidental finding.) Surgical resection of the iliac lymph nodes was attempted but aborted because of a high risk of hemorrhage. The primary anal sac tumor was resected. Palliative radiation therapy (three weekly doses of 8 Gy) to the iliac lymph nodes resulted in resolution of clinical signs.
Chemotherapy
Chemotherapy has been used for anal sac adenocarcinoma because of the high rates of local metastatic disease and recurrence. The information in retrospective studies can be difficult to interpret because chemotherapy is often administered along with surgery and radiation or is only administered in dogs with advanced disease, which limits the conclusions that can be drawn about the effect of the chemotherapy. Drugs that have been used include mitoxantrone, doxorubicin, melphalan, cisplatin, carboplatin, 5-fluorouracil, mithramycin, vincristine and cyclophosphamide, epirubicin, and actinomycin-D.4-8
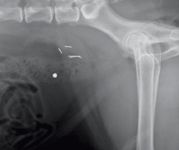
4B. A lateral caudal abdominal radiograph taken of the same dog as in Figure 4A three months after palliative radiation therapy, showing a partial reduction in the size of the iliac lymph nodes and less compression of the colon as it enters the pelvic canal. (The staples were placed during surgery to aid in radiation planning.)
In one study, two of four dogs with unresectable anal sac gland carcinomas that received carboplatin exhibited decreased mass size sufficient to permit surgical resection.6 In the same study, 12 of 40 dogs with iliac lymphadenopathy had relief of fecal obstipation after carboplatin treatment.6 A different study reported a partial reduction in tumor size in four out of 13 dogs with anal sac adenocarcinoma treated with cisplatin alone and in one out of three dogs treated with carboplatin alone.4 Favorable survival times have been reported in dogs treated with radiation, surgery, and mitoxantrone (n = 15) and surgery with oral daily melphalan (n = 19); however, the individual role of chemotherapy in those studies cannot be determined as there were no control groups.5,7
Given the reported partial responses, the platinum agents appear to have some efficacy against anal sac adenocarcinoma and may be appropriate for adjuvant or neoadjuvant (preliminary) therapy.
PROGNOSIS
The survival time for dogs with anal sac adenocarcinoma varies, and retrospective studies have attempted to identify significant prognostic factors. The overall median survival time in two larger studies evaluating 80 and 113 dogs was 479 and 544 days, respectively.6,8 The dogs in these studies received a wide variation in treatments, including surgery, radiation therapy, and chemotherapy, making it difficult to draw conclusions about the effect of individual treatment modalities or effective chemotherapy protocols. In the larger study, dogs that underwent surgery as a part of their treatment had an improved survival time compared with dogs that received chemotherapy alone.8 Larger tumors, the presence of distant metastatic disease, and hypercalcemia have been variably associated with a significantly decreased survival time.3,6,8 The median survival time was higher at 956 days in a study of 15 dogs that were all treated in the same manner with surgery, radiation, and mitoxantrone chemotherapy.7 None of the tumors in the dogs in this study had spread beyond the iliac lymph nodes, which may have contributed to the lengthy survival time.7
Because of the prognostic significance of tumor size at diagnosis and the presence of metastatic disease, the most favorable prognosis can be expected with early detection and aggressive treatment. Although hypercalcemia has been associated with a decreased survival time in some studies, it has not been a consistent finding.4,7,11 The presence of hypercalcemia should not warrant a more conservative approach, given that favorable responses and prolonged survival times with appropriate treatment have been reported.7,11
SUMMARY
Anal sac adenocarcinoma is a locally invasive tumor with a high rate of metastasis to the local lymph nodes. Clinical signs may be associated with partial obstruction of the colon or rectum by the primary tumor or enlarged metastatic lymph nodes. In many cases, the tumor is an incidental finding on routine physical examination. Hypercalcemia is present in up to half of cases and may contribute to the presenting clinical signs; it typically resolves with surgical removal of the tumor. Routine staging includes a complete blood count, a serum chemistry profile, a urinalysis, thoracic radiography, and abdominal ultrasonography. A multimodal treatment approach is recommended, with surgery and radiation therapy providing local control. The ideal chemotherapy protocol for preventing or delaying recurrence or the development of metastatic disease is still undefined. Early detection and treatment are imperative to achieving the most favorable outcome.
Meredith Gauthier, DVM, DACVIM (oncology)*
Lisa G. Barber, DVM, DACVIM (oncology)
Kristine E. Burgess, MS, DVM, DACVIM (oncology)
Department of Clinical Sciences
Cummings School of Veterinary Medicine
Tufts University
North Grafton, MA 01536
*Current address:
Mississauga Oakville Veterinary Emergency Hospital and Referral Group
2285 Bristol Circle
Oakville, ON L6H 6P8
REFERENCES
1. Turek MM, Withrow SJ. Tumors of the gastrointestinal tract. H. Perianal tumors. In: Small animal clinical oncology. 4th ed. St. Louis, Mo: Saunders Elsevier, 2007;503-510.
2. Goldschmidt MH, Shofer FS. Anal sac gland tumors. In: Skin tumors of the dog and cat. 1st ed. Oxford, UK: Pergamon Press, 1992;103-108.
3. Ross JT, Scavelli TD, Matthiesen DT, et al. Adenocarcinoma of the apocrine glands of the anal sac in dogs: a review of 32 cases. J Am Anim Hosp Assoc 1991;27:349-355.
4. Bennett PF, DeNicola DB, Bonney P, et al. Canine anal sac adenocarcinomas: clinical presentation and response to therapy. J Vet Intern Med 2002;16(1):100-104.
5. Emms SG. Anal sac tumours of the dog and their response to cytoreductive surgery and chemotherapy. Aust Vet J 2005;83(6):340-343.
6. Polton GA, Brearly MJ. Clinical stage, therapy, and prognosis in canine anal sac gland carcinoma. J Vet Intern Med 2007;21(2):274-280.
7. Turek MM, Forrest LJ, Adams WM, et al. Postoperative radiotherapy and mitoxantrone for anal sac adenocarcinoma in the dog: 15 cases (1991–2001). Vet Comp Oncol 2003;1(2):94-104.
8. Williams LE, Gliatto JM, Dodge RK, et al. Carcinoma of the apocrine glands of the anal sac in dogs: 113 cases (1985-1995). J Am Vet Med Assoc 2003;223(6):825-831.
9. Polton GA, Mowat V, Lee HC, et al. Breed, gender and neutering status of British dogs with anal sac gland carcinoma. Vet Comp Oncol 2006;4(3):125-131.
10. Elliott J, Dobson JM, Dunn JK, et al. Hypercalcaemia in the dog: a study of 40 cases. J Small Anim Pract 1991;32:564-571.
11. Hobson HP, Brown MR, Rogers KS. Surgery of metastatic anal sac adenocarcinoma in five dogs. Vet Surg 2006;35(3):267-270.
12. Jeffery N, Phillips SM, Brearly MJ. Surgical management of metastasis from anal sac apocrine gland adenocarcinoma of dogs. J Small Anim Pract 2000;41:390.
13. Anderson CR, McNiel EA, Gillette EL, et al. Late complications of pelvic irradiation in 16 dogs. Vet Radiol Ultrasound 2002;43(2):187-192.
Newsletter
From exam room tips to practice management insights, get trusted veterinary news delivered straight to your inbox—subscribe to dvm360.