How veterinary medicine can save the world, Part 3: Serving the public
Natural disasters. Disease outbreaks. Terrorist bombings. When crisis hits, these veterinarians are on the scene.
Scott Mason found his passion in the bombed-out shadow of the Alfred P. Murrah Federal Building in Oklahoma City in 1995. Lorna Lanman heard her passion in the eerie silence of small family farms stripped bare of livestock by foot-and-mouth disease in northern England in 2001. Carrie McNeil found a way to harness her activist spirit through investigating everything from rabies to malnutrition with the Epidemiological Intelligence Service (EIS), part of the U.S. Centers for Disease Control (CDC).
Veterinarians all, Mason and Lanman spend most of their time in private practice, seeing dogs and cats, taking histories, treating disease and behavior problems, working the traditional front lines of veterinary medicine. McNeil has worked in private practice but now does public service work full time. When disaster strikes, when public health is threatened, they're all three packed up and ready to roll. But recently, between crises and disasters, they had a break—and time to talk with dvm360 about how public service had brought a new passion into the trajectory of their veterinary careers.
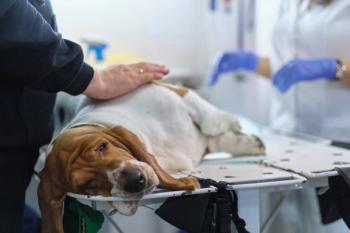
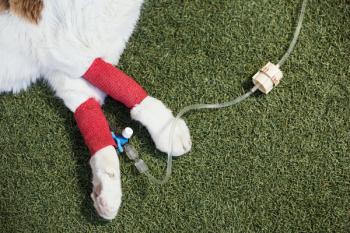
Dr. Scott Mason (right) and two task force members work on an injured search-and-rescue dog during disaster aid operations after the Moore, Okla., tornado this year.
Sign me up
When Scott Mason, DVM, EMT, tries to remember all the deployments across his 18 years of crisis response, he can't do it. He rifles through the names of hurricanes and tornadoes when he realizes they are all starting to blur together. The first, however, is stamped uncomfortably in his mind—so much so that he thinks he suffered a mild case of posttraumatic stress from it.
On April 19, 1995, Mason had just begun seeing clients in his small animal clinic about 10 miles from downtown Oklahoma City. At 9:02 a.m., the front windows rumbled. He stepped outside and looked to the sky, thinking a sonic boom may have caused his building to shake. It wasn't a sonic boom. It was the work of a domestic terrorist who had parked a rented Ryder truck in front of the Alfred P. Murrah Federal Building and set off a fertilizer bomb that ripped the concrete and steel structure into the street, killing 168 people, including 19 children.
In minutes the story broke on television. The news reporters were asking residents to stay away from the site where rescue crews were busy searching mountains of concrete for survivors. "I'm a guy who always follows the rules," Mason says. "So I stayed away."
But two days later the state veterinary association issued a call for volunteers. "Boy, I was like, 'Sign me up,'" Mason says. "I grabbed tons of stuff off my shelves and rushed down there. We had to go through some processing and we got some makeshift badges and we went onto the site to connect with the search and rescue groups. I only remember treating one laceration while I was down there and one case of dehydration—I gave some fluids.
"But it was an eye-opening event," he continues. "It grabbed that passion in me to help. Maybe some of it was a little rush of adrenalin, I don't know. But it sparked something."
It also slapped him in the face. Mason was walking back from the ruins of the federal building to one of the peripheral work sites at about 2 a.m. during one of his night shifts. He had, of course, noticed the orange spray paint investigators used to mark places where evidence had been found.
"I was walking back in the eerie glow of the building, which was lit up, and I looked down and saw a spray painted area where they had found just a part of somebody," he says. "You just break down at a moment like that because the impact suddenly smacks you in the face. The whole thing just seemed incredibly sad."
Since that night in 1995, Mason has observed plenty more disaster. "I've been through enough now that most of this stuff I've seen before," he says. He compares the experience to veterinary practice, where doctors perform euthanasia regularly but learn to bury their heads and keep going. That doesn't mean he's immune.
On May 20 this year, an EF5 tornado whirled into Moore, Okla., with winds up to 210 mph, and, of course, Mason and his National Veterinary Response Team (NVRT) were deployed in the search and recovery effort. On their second day in Moore they were dispatched to the Plaza Towers Elementary School site. They had worked all night Monday and all day Tuesday and were exhausted when they walked through the shattered walls of the school where seven children had died.
"As we entered into where it was pretty much obliterated, I looked off to my left," Mason recalls. "One wall of this one classroom was still standing. It still had the hooks on the wall and some of the kids' backpacks were still hanging up there.
"It was one of those moments where—bang!—it just hits you upside the head," he says. "It was the hardest I'd been hit mentally since the Murrah bombing. I've got two daughters. You know what's happened right where you are and it just breaks your heart. It breaks your heart."
But it didn't slow him down. Mason is a passionate advocate for the place of veterinarians in disaster preparedness and response. "Sometimes people say, 'We've got to focus on saving people … don't worry about the animals,'" he says. "What I explain to them is that animal issues become people issues. There have been several studies showing that people will put themselves in harm's way readily for their animals. I saw a television clip of a roadblock during a California wildfire where a ranch owner pulled up with his truck. The officers told him he couldn't go in. He said, 'Well, you'll have to shoot me then,' and got back in his truck and went in after his horses."
Silence of the lambs
Lorna Lanman, DVM, discovered her passion for public service after she retired to Sun City, Ariz., in 1995. Actually, "retired" isn't the right word, although that's how she describes her life since selling the three practices she owned in Illinois for more than two decades. Four years after "retiring," she was on a Veterinary Medical Assistance Team—a program run by the American Veterinary Medical Association—and deployed to Houston for Hurricane Floyd. That was followed by hurricanes Katrina and Rita, several wildfires in the Southwest, the World Special Olympic Games in Alaska, the Democratic National Convention in Los Angeles, an avian influenza outbreak in the Shenandoah Valley of Virginia, and Sept. 11, 2001, in New York City.
Dr. Lorna Lanman rescues a dog from a home after Hurricane Katrina hit the Gulf Coast.
On April 25, 2001, foot-and-mouth disease (FMD) brought Lanman across the sea to the north of England—the source of a world outbreak. The USDA didn't just send her to help manage FMD in livestock, though she did plenty of that. They also wanted her to report on the effects on people: farmers, volunteers, public health workers, veterinarians. Should an outbreak occur in the United States, they wanted to be ready.
"I grew up on a farm in Illinois and I know how attached we were to our animals," Lanman says. "One farmer told us he milked his cows and turned them out, and one cow came back and stuck her head in the door and bellowed at him. He wondered what was wrong with her, so he let her come back in and she went to her stanchion. He got his thermometer out and stuck it up her rectum and she had an elevated temperature. He got scared. He went around to look in her mouth and he said it felt like he was walking a mile to get around her. When he opened her mouth and saw that lesion, he told us he just cried."
According to her written account, Lanman and the other veterinary volunteers were issued Tyvek suits, waterproof rubber suits to wear over the Tyvek, rubber gloves, rubber boots, cell phones, GPS units, surgical supplies and waterproof notebooks, all fitting the highly contagious nature of the disease that paralyzed the nation. The British government was so worried about the spread of FMD that roads were cut off through the north, causing the Lake District to lose its entire tourist season.
In fact, the economic damage from the U.K. outbreak was estimated at $12 billion, according to a University of Newcastle study. The tourism industry alone lost $390 million, according to the BBC. The economic role of veterinarians in a foot-and-mouth disease crisis can't be underestimated. A 2001 article in Science suggested that during the first two months of the outbreak, a one-week delay in diagnosing the disease can cost a nation $1.7 billion dollars.
As staggering as they are, the numbers don't capture the nature of Lanman's work in England. "One day I helped them put a thousand lambs to sleep and 200 ewes," she says. "Then we went to another farm and put 200 head of cattle to sleep. They had 10 million animals total killed off. That's a lot of carcasses. There was blood in the water supply. The pyres on the farms put toxic smoke in the air."
The human toll was devastating as well. The farmer Lanman described who cried after finding his first lesion was racked with guilt, she says. He knew he had to call and report what he'd found, so he did. The authorities came and killed all his livestock. Then they visited his neighbors as well.
"One guy hanged himself," Lanman recalls. "He felt guilty that he had brought the virus home to his family's farm and then all the farms around their farm got taken out. He was guilt-ridden and he hung himself. And he was a young guy.
"One farmer told me what they hated most was the silence when all the lambs were gone," she continues. "You drove through that northern area where all those farms were and there was just nothing out in the field."
The month Lanman spent in England, she says, helped prepare her for the 9/11 deployment. She thinks the foot-and-mouth outbreak made her a stronger person—but not a hardened person. "As veterinarians, we deal with life and death every day," she says. "We do our job as best we can."
Her job in New York after 9/11 was to care for search dogs sifting through a landfill full of debris from the World Trade Center. She set up a veterinary clinic on the site to care for and decontaminate the teams of recovery dogs busy searching the rubble for human body parts. The parts those dogs found resulted in the identification of 300 people.
As if all that action—and more—weren't enough, Lanman started a mobile practice in 2004 in Arizona, then moved into a building in 2007. "I actually did retire in 1994," she contends. "I planned to play a lot of golf." Instead, she's doing things like trapping cats after the Moore, Okla., tornado this summer. One family came through looking for their cat during the day and she trapped it that night. "People who lose their home also lose their pets," she says. "It's a great feeling when you can reunite them."
"There's no problem too big if you get the right people together"
This summer Carrie McNeil, DVM, MPH, found herself at a big-city grocery store where the aisles were bursting with fresh fruit and vegetables, fresh meat and chicken—healthy food everywhere. It may not have seemed unusual to the average U.S. shopper, but McNeil was brought up short.
Dr. Carrie McNeil, MPH, in New Mexico with the family dog, Joe Friday.
She had just completed a visit to the Navajo Nation as part of a CDC team addressing tribal leaders' concerns about the rising tide of obesity and diabetes among the Navajo population. "We literally went to every convenience store and trading post in every tiny town around the Navajo Nation and looked at the food options," McNeil says. What she and the other researchers found was a lack of options for healthy food.
"[Navajo leaders] recognized the need and I don't think there was any trouble getting evidence," McNeil says. But solutions are more difficult than gathering proof of a problem. "Sometimes the easiest way to get healthy food is for people to just grow their own, raise their own livestock to eat and their own vegetables. I'm not sure what their policies will include, but it will be interesting to see."
McNeil says the CDC's Epidemic Intelligence Service teams are invited by cities, tribes and even countries to investigate potential health problems. She was deployed with this team because she'd worked with other tribes in New Mexico and also because she's a veterinarian, even though the trip involved no specific veterinary medicine.
"We have expertise in food availability, food security and food safety," she says. "Those are areas where veterinarians can play a huge role. We're trained in this. Even if you're a small animal practitioner, you receive some training in the food animal production world. We all took food safety training. It's something that impacts every person and every animal. In this case it was partly a matter of understanding how the food system works and how the agriculture system works. Hopefully that helped me supply some additional insight into the project."
Currently McNeil is transitioning to a new position with Sandia National Laboratories' International Biological Threat Reducation program, which focuses on global biosecurity. Before joining the EIS, she spent four years working as an emergency veterinarian in New Mexico, California and Georgia. "You see so much in emergency medicine where you say, 'This is something I could be preventing,'" she says. "I was really interested in preparedness, and much of that is really a public health focus. So I went back to get my public health degree."
The public health arena actually helps McNeil close the loop on her longstanding interest in public policy, a thread woven throughout her veterinary education and her career. In 1997 she was a Jesse Marvin Unruh fellow in the California State Assembly working for one of her mentors, Assemblywoman Shiela Kuehl. Her undergraduate biology degree distinguished her from the attorneys in the legislature when it came to science and health issues. She worked on women's health, environmental health and animal health issues, among others. During veterinary school at the University of California-Davis, she took a yearlong hiatus from her studies to work with Kuehl again, this time in the California State Senate.
In veterinary school she was smitten by the work students and faculty were doing at UC-Davis in the Wildlife Health Center. The idea of ecosystem management fit well with the policy work she'd been doing legislatively.
"I was always interested in the One Health aspect of veterinary medicine and after graduation I worked on some water quality, environmental health, and ecosystem health issues from a nonprofit perspective," she says. "But I really missed working one-on-one with animals and clients. So I went back and did an internship at VCA in West LA, which is where I got my training in small animal medicine and my interest in emergency medicine."
McNeil sees a connection between working with animals in veterinary practice and ecosystem management. "Water-quality testing is similar to testing the blood of an animal," she explains. "It's your diagnostic tool to look at the health of the waterway." The major connection for McNeil is the role public policy plays, which brings together her veterinary training and her desire to work on problems at their political source. Her EIS work is like a river fed by all the streams of her working life.
"I feel really fortunate that I've had these opportunities," she says. "Public health has been a great way personally for me to bring together my policy interest and human health interests and animal and environmental health interests. And, just like in clinical practice, you don't know what you're going to see day to day."
McNeil has been called to investigate foodborne illness outbreaks, respiratory disease outbreaks and norovirus outbreaks. She's investigated the prevalence of whooping cough in New Mexico. She's presented a paper on the diversion of controlled substances in New Mexico and the potential connection to prescription overdose deaths. She's helped investigate and manage a rabies outbreak in southern New Mexico in which more than 100 unvaccinated exposed pets had to be euthanized and 29 people had to receive post-exposure prophylaxis.
"At the most basic level of diseases, all of our Class A bioterrorism agents, except for smallpox, are agents that affect people and animals, and many of our infectious diseases affect people and animals," she says. "So that's always been an obvious connection to me. Once you get into the food system, food availability, general public health and well-being, you find a lot of areas where veterinary medicine can play a role in improving human health."
Preparedness policy, for example, requires the combined efforts of experts in human hospitals, veterinary hospitals, transportation, food access and a plethora of other areas. And while many people are cynical about the possibility that today's divisive policymakers can work together for effective solutions, McNeil says with a chuckle that she is not.
"The policy work I did taught me the importance of bringing different players together," she says. "At the end of the day, more often than not, you really can get people to come to the table and work together. I've seen it work. The problems are too big for people not to work together and figure things out. There's no problem too big if you get the right people together."
John Lofflin is a freelance writer in Kansas City, Mo., with extensive experience writing about the veterinary profession.