- dvm360 June 2023
- Volume 54
- Issue 6
- Pages: 36
Honeybee vaccination: How does it work, and what does it mean?
Now that the FDA has conditionally approved the first-ever insect vaccine for the prevention of American foulbrood, what does it mean for the future of sick colonies?
As a veterinarian, I have administered thousands of vaccinations to everything from tiny kittens to towering draft horses. Although the species are very different, the way vaccines are administered and how they work have been fundamentally the same— until now. In early January of this year, the United States Department of Agriculture announced it had conditionally approved the first-ever insect vaccine for the prevention of American foulbrood (AFB) in honeybees.
Honeybees are food animals: firstly, because they produce honey, which we harvest for human consumption; and secondly, because of the role they play in crop pollination (which is often underappreciated). Approximately 70% of crops grown for human consumption are dependent on animal pollination, of which honeybees are the predominant managed species.1 Their importance in human food security places huge demands on the apiculture industry to supply healthy colonies, at times based on crop phenology rather than honeybee biology. Yet honeybee health is not great right now. As an agricultural species, we breed honeybees and can maintain the national population to meet demand. However, beekeepers have been dealing with elevated annual loss rates since epidemiological data started to be collected in annual surveys by the Bee Informed Partnership (BIP) in 2008.2 Over the 15-year period, BIP has found that beekeepers are losing an average of one-third to one-half of their colonies every year, which is much higher than the historical loss rate of 10% to 15%.3
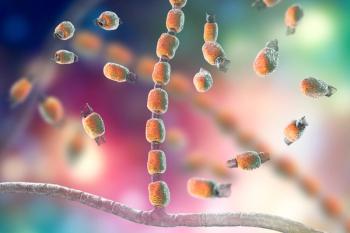
AFB is caused by the spore-forming bacteria Paenibacillus larvae and is considered the most devastating brood disease of honeybees.4 Only young larvae (< 48 hours old) are susceptible to infection. Nurse bees spread the disease by inadvertently contaminating the brood food. The infectious dose is as little as 8 to 9 spores. Once ingested, the spores germinate, followed by rapid multiplication within the midgut of the larvae.5,6 The bacteria then breach the epithelial layer and invade the haemocoel, leading to sepsis and subsequent death of the larvae.6 The larval remnant dries into a hard scale that contains billions of infectious spores that are extremely resistant and persistent, remaining infectious under normal environmental conditions for decades. The disease is not only fatal to the individual larvae, but as more and more young larvae die, the colony can also collapse. Spores are easily transmitted between colonies, most often through beekeeper activity and the bees’ robbing behavior. The high virulence of the bacteria, the massive number of persistent spores produced, and the ease with which the disease can spread give AFB the potential to be devastating to beekeeping operations. Because of this, the industry relies on significant mitigation strategies to prevent large-scale outbreaks.
It is best practice, and often mandated under state and provincial regulations, to cull clinical cases and destroy the bees and associated equipment by fire. Although this is the best way to eliminate the infectious spores, it can have significant economic consequences for the beekeeper. Some beekeepers in the United States and Canada instead rely on routine administration of antimicrobials once or twice yearly to prevent the clinical stage of AFB. However, because of concerns of resistance,7 the potential for antimicrobial residues in a food of animal origin, detrimental health impacts such as dysbiosis of the microbiome, and barriers to access, there is interest in finding alternative prevention strategies.8
Enter the honeybee vaccine. There are 2 main differences between vaccinating honeybees and vaccinating all the other animals that veterinary profes- sionals normally work with. Firstly, honeybees lack an acquired immune system and therefore cannot produce antibodies. Secondly, depending on the time of year, a colony may contain thousands of suscep- tible larvae, and the individual life span of a honeybee can be as short as 4 to 6 weeks, making individual administration impractical. So how does the vaccine work? Within every colony, there is a queen—the single reproductive female bee who lays all the eggs that give rise to the thousands of worker and drone bees. Unlike the other adult bees that have a short life span, a healthy queen within a healthy colony can live and reproduce for multiple years. The AFB vaccine targets only the queen and relies on her to pass the immunity on to her offspring through transgenerational immune priming (TGIP).9 Inactivated P larvae is mixed into sugar syrup and then fed to the queen bee over the period of approximately 1 week. The proposed mechanism of action is that as she ingests the bacterin, the protein vitellogenin picks up immune elicitors, such as components of the bacteria, that she has been exposed to. The queen is then placed into a queenless colony where, if she is accepted, she will begin to lay eggs.
One function of vitellogenin is as an egg yolk protein that is consumed during development, and therefore the vitellogenin with the immune elicitors can potentially be incorporated into the egg. Once hatched, the larvae would then be primed to recognize and respond to P larvae, making them resistant to infection. A vaccine challenge study reported a protective association between queen vaccination and larval death, with the vaccinated group having a reduction in larval death by 30% to 50% following a short-term challenge with infectious P larvae spores. Furthermore, there were no statistically significant differences in the occurrence of negative events, such as queen failure, between the vaccinated and placebo groups.9 It is worth noting that the treatment groups were small and clustered data were analyzed at the individual larval level. A recent longitudinal field study by Leponiemi et al similarly found no negative effects on productivity parameters, pathogen loads, or gene expression.10 However, the study also found no effect of treatment on AFB occurrence and did not see a difference in gene expression associated with immune response and with P larvae exposure between vaccinated and control groups.10
It is unknown whether this vaccine will make a long-term difference
to honeybee health in the United States. Will beekeepers be interested in purchasing vaccinated queens? Is the cost of vaccination worth implementation within their operations? Could vaccination potentially reduce the reliance on routine antimicrobial administration? How long will the TGIP be effective following acceptance of a vaccinated queen? Is the vaccine protective under field conditions over the long term? Can this technology be used to develop vaccinations against other honeybee pathogens? This vaccine may be a major step forward in how we manage disease in invertebrate populations but more data are needed, and these questions can only be answered over time.
Britteny Kyle, DVM, MSc, graduated from the Ontario Veterinary College in 2009. Upon graduation she entered small animal practice in Toronto, where she worked as an associate for several years before switching her focus to honeybee medicine. She was elected to the board of the Honey Bee Veterinary Consortium in 2019 and served as president of the organization in 2020. Her projects for the consortium have included chairing the annual conference and developing a certification program for veterinarians interested in working with honeybees. In the fall of 2020, she returned to Ontario Veterinary College to earn her master’s degree in epidemiology with a focus on American foulbrood. In 2021, she began her doctoral degree in epidemiology with a collaborative specialization in One Health to continue studying American foulbrood in honeybee populations. When she is not studying bees, Kyle is busy maintaining her small zoo of 3 boys, 2 cats, 1 dog, and a handful of honeybee colonies.
References
- Gallai N, Salles JM, Settele J, Vaissière BE. Economic valuation of the vulnerability of world agriculture confronted with pollinator decline. Ecol Econ. 2009;68(3):810-821. doi:10.1016/j.ecolecon.2008.06.014
- Aizen MA, Harder LD. The global stock of domesticated honey bees is growing slower than agricultural demand for pollination. Curr Biol. 2009;19(11):915-918. doi:10.1016/j. cub.2009.03.071
- Management survey. Bee Informed Partnership. Accessed May 12, 2023. https://research.beeinformed.org/survey/
- Genersch E, Forsgren E, Pentikäinen J, et al. Reclassification of Paenibacillus larvae subsp. pulvifaciens and Paenibacillus larvae subsp. larvae as Paenibacillus larvae without subspecies differentiation. Int J Syst Evol Microbiol. 2006;56(pt 3):501-511. doi:10.1099/ijs.0.63928-0
- Brødsgaard CJ, Ritter W, Hansen H. Response of in vitro reared honey bee larvae to various doses of Paenibacillus larvae larvae spores. Apidologie (Celle). 1998;29(6):569- 578. doi:10.1051/apido:19980609
- Yue D, Nordhoff M, Wieler LH, Genersch E. Fluorescence in situ hybridization (FISH) analysis of the interactions between honeybee larvae and Paenibacillus larvae, the causative agent of American foulbrood of honeybees (Apis mellifera). Environ Microbiol. 2008;10(6):1612-1620. doi:10.1111/j.1462-2920.2008.01579.x
- Krongdang S, Evans JD, Pettis JS, Chantawannakul P. Multilocus sequence typing, biochemical and antibiotic resistance characterizations reveal diversity of North American strains of the honey bee pathogen Paenibacillus larvae. PLoS One. 2017;12(5):e0176831. doi:10.1371/journal. pone.0176831
- Raymann K, Shaffer Z, Moran NA. Antibiotic exposure perturbs the gut microbiota and elevates mortality in honeybees. PLoS Biol. 2017;15(3):e2001861. doi:10.1371/ journal.pbio.2001861
- Dickel F, Bos NMP, Hughes H, et al. The oral vaccina- tion with Paenibacillus larvae bacterin can decrease susceptibility to American Foulbrood infection in honey bees—a safety and efficacy study. Front Vet Sci. 2022;9:946237. doi:10.3389/fvets.2022.946237
- Leponiemi M, Wirta H, Freitak D. Trans-generational immune priming against American foulbrood does not affect the performance of honeybee colonies. Front Vet Sci. 2023;10:1129701. doi:10.3389/fvets.2023.1129701
Articles in this issue
over 2 years ago
Diagnosing and stabilizing hemoabdomenover 2 years ago
Creating Dr. Donita’s Veterinary Concierge Servicesover 2 years ago
Offensive body art & political discussions in the workplaceover 2 years ago
Treating inappetence in dogsover 2 years ago
Renal transplants in catsover 2 years ago
Does veterinary medicine need a midlevel professional?over 2 years ago
Common skin conditions in petsover 2 years ago
Career advice for new graduatesNewsletter
From exam room tips to practice management insights, get trusted veterinary news delivered straight to your inbox—subscribe to dvm360.