Explore the options for dental treatment plans
Creating a dental treatment plan can be frustrating. As with other veterinary disciplines, dental diagnosis and care is one-third recognition of disease, one-third understanding anatomy and medical principles, and the last third performing needed care.
Creating a dental treatment plan can be frustrating. As with other veterinary disciplines, dental diagnosis and care is one-third recognition of disease, one-third understanding anatomy and medical principles, and the last third performing needed care.
Photo 1: Uncomplicated enamel fracture.
Fortunately, the general practitioner or a close referral can manage most dental cases.
Let's review progressive options based on your technician's exam findings:
1. Do nothing with the observed pathology other than future follow-up. No treatment is needed with observed pathology where there is a "functional" abnormality (even though the dentition is not "normal," the animal does not derive adverse effects). Examples of functional abnormalities include an enamel chip that does not penetrate the dentin sufficiently to affect the pulp and where radiographs do not show pathology. Other cases where no treatment is the best course include functional malocclusions, and cases where the root of a tooth shows external resorption that does not extend to the crown (Photos 1, 2, 3).
Photo 2: No endodontic or periapical pathology evident on intraoral radiograph.
Photo 3: Functional malocclusion.
Photo 4: Stage 1 gingivitis in a dog.
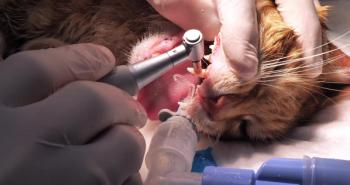
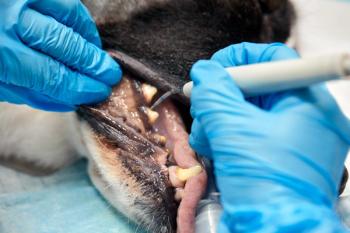
2. Teeth cleaning, irrigation, polishing, application of professional plaque barrier gel in cases where Stage 1 gingivitis (inflamed gingiva without evidence of support loss); and Stage 2 non-pocket periodontal disease (less than 25 percent support loss) as evidenced by gingival recession, non-surgical care is indicated (Photos 4, 5).
Photo 5: Stage 1 gingivitis in a cat.
Photo 6: Stage 2 periodontal disease in a dog.
3. Local antimicrobial administration (LAA) is indicated in Stage 2 (less than 25 percent support loss) and Stage 3 (25 percent to 50 percent support loss) periodontal disease where there are periodontal pockets (in contrast to gingival recession) and where the pet owners can provide home care to control periodontal disease progression (Photos 6, 6a, 7).
Photo 6a: This probe shows less than 25 percent support loss.
Photo 7: Stage 3 periodontal disease in a cat.
Photo 8: Clinically missing mandibular first premolar in a 6-month-old Yorkshire terrier.
Photo 9: Radiograph shows impacted tooth in proper position treatable with operculectomy.
4. Periodontal surgery can save teeth if the tooth and patient are appropriate. Operculectomy (removal of the gingiva over a partially erupted tooth crown) is indicated in a young dog or cat (younger than 8 months old) whose tooth is expected to fully erupt once the obstructing gingiva is excised (Photos 8, 9). Open flap exposure for cleaning and debridement is used to expose a tooth root in selective cases where the periodontal pocket extends greater than 5 mm and the client is committed to saving his pet's teeth despite a guarded prognosis. Apical reposition flap surgery can be performed to decrease periodontal pocket depths (Photo 10).
Photo 10: 12-mm probing depth.
5. Vial pulp therapy can be used where a tooth fracture or planned crown reduction has penetrated enamel and dentin without directly entering the pulp (near pulp exposure) (Photo 11). Treatment depends primarily on the age of the animal and time of the fracture. A young (younger than 9 months old) animal will have an enlarged pulp chamber that would be difficult to adequately seal via conventional endodontics. Vital pulp therapy can be performed in these cases with periodic radiographic reexamination. The older animal with increased dentin width between the fracture and pulp can either have root-canal therapy performed with predictable results, serial radiographs for signs of endodontic involvement before root canal; or extraction. If the fracture is acute (up to two days in the young animal and two weeks in the animal older than 18 weeks, vital pulp therapy can be attempted with a guarded prognosis. Extraction or conventional root-canal therapy should be performed with a more predictable outcome in any traumatically fractured tooth. Vital pulp therapy is also employed in cases where the crown height is reduced to create a functional and comfortable bite in selected cases of malocclusion.
Photo 11: Near pulp exposure.
Photo 12: Discolored mandibular canine tooth secondary to chronic necrotizing pulpitis.
Photo 13: Slab fracture of the maxillary fourth premolar.
6. Conventional root-canal therapy is the treatment of choice for end-stage pulp disease secondary to fracture, chronic pulpitis, caries or ascending periodontal disease (Photo 12). Ideal therapy depends on age of animal, age of pulp exposure, condition of the tooth and periapical structures. If the fracture is acute (up to two days in the young animal and two weeks in the animal older than 18 weeks, or if the fracture is older, conventional or surgical root-canal therapy or extraction are the treatments of choice (Photo 13). If the animal is younger than 9 months old, vital pulp therapy can be performed in the non-infected tooth. If the animal is older than 9 months and the apex closed, conventional or surgical root canal is the more predictable procedure. In the infected young tooth, apexification is the desired outcome.
Photo 14: Type 2 feline odontoclastic resorption of the mandibular canines.
Photo 15: Lingually displaced mandibular canine.
7. Crown reduction with gingival closure can be used to treat Type 2 feline odontoclastic resorption lesions with evidence of ankylosis (Photo 14). Inclined plane made from acrylic or metal can move lingually displaced canines into functional positions (Photo 15). Orthodontic buttons and elastics can be used to reposition teeth into and for maxillary or mandibular fracture stabilization (Photo 16).
Photo 16: Rostrally positioned canine in a young Maltese.
8. Oral surgery is the treatment of choice for many oral masses both benign and malignant. When considering oral surgery, generally a 1-cm margin is indicated for benign masses, 2 cm or greater for malignant tumors (Photos 17, 18).
Photo 17: Benign oral mass.
Photo 18: Malignant oral mass and fractured maxillary fourth premolar.
9. Extraction is often the preferred therapy once the client has been informed and consent granted. Extraction is indicated where Stage 4 periodontal disease is present (the tooth has more than 50 percent support loss based on probing depths; greater than Stage 3 mobility or when gingival recession has progressed past the mucogingival line). Extraction is also the best therapy where the tooth has between 25 percent to 50 percent support loss and the owner and/or the patient will not allow appropriate home care (Photo 19).
Photo 19: Feline molar affected by Stage 3 periodontal disease.
Some fractured teeth are also best extracted, especially those that have pulp exposure and Stage 3 or 4 periodontal disease, marked internal resorption, or where root-canal therapy is not a viable option due to owner's wishes or the practice's capability and lack of referral option (Photo 20).
Photo 20: Periapical lucency secondary to pulpal death.
Feline odontoclastic resorption affected teeth should be extracted via flap exposure where there is visible periodontal ligament on intraoral radiographs (Type 1) (Photo 21). Some feline gingivostomatitis patients that do not respond to home care benefit from extraction of the teeth distal to the canines, those that still do not respond should have all the teeth extracted (Photo 22). Extra (supernumerary) teeth that cause crowding, predisposing the normal teeth to periodontal disease should be extracted. Additionally, persistent primary (deciduous) teeth should be removed at time of diagnosis to prevent potentially harmful location of the adult teeth. Extraction is also the treatment of choice for advanced caries (Photo 23).
Photo 21: Type 1 odontoclastic resorption.
Photo 22: Feline gingivostomatitis.
Consider the valuable dental information our technicians provide with each oral assessment, treatment and prevention visit. An overwhelming majority of conditions affecting our patients' mouths can be treated with one or more of the previously presented options. Not only will your patient benefit, but it's fun to see how well they do and how much your clients appreciate your care.
Photo 23: Carious mandibular first molar in a dog.
Dr. Bellows owns Hometown Animal Hospital and Dental Clinic in Weston, Fla. He is a diplomate of the American Veterinary Dental College and the American Board of Veterinary Practitioners. He can be reached at (954) 349-5800; e-mail: