Diagnosing cranial cruciate ligament pathology
Recent advances in diagnostic visualization and surgical treatments have stimulated an increased emphasis on early clinical recognition of cranial cruciate ligament pathology. This article describes characteristics of normal and pathologic cranial cruciate ligaments and details clinical techniques to help you diagnose cranial cruciate ligament pathology earlier.
Cranial cruciate ligament pathology is a leading cause of lameness in dogs.1 Recent advances in diagnostic visualization and surgical treatments have stimulated an increased emphasis on early clinical recognition of cranial cruciate ligament pathology. This article describes characteristics of normal and pathologic cranial cruciate ligaments and details clinical techniques to help you diagnose cranial cruciate ligament pathology earlier.
ANATOMY
Four ligaments passively stabilize the canine stifle joint: the cranial cruciate, caudal cruciate, medial collateral, and lateral collateral ligaments. The cranial cruciate ligament originates from the caudomedial aspect of the lateral femoral condyle and courses in a craniomedial direction to insert on the cranial intercondyloid area of the tibia immediately caudal to the intermeniscal ligament (Figure 1).2 The cranial cruciate ligament is functionally composed of a craniomedial band and a caudolateral band.3 While the craniomedial band remains taut throughout a full range of extension and flexion, the caudolateral band becomes lax during flexion. The caudal cruciate ligament arises from the lateral surface of the medial femoral condyle and passes caudodistally to insert on the lateral aspect of the popliteal notch of the tibia (Figure 1). The cranial and caudal cruciate ligaments spiral around one another as they course distally. The orientation of the cranial cruciate ligament prevents cranial tibial translation through a full range of motion, excessive internal rotation during flexion, and stifle hyperextension.
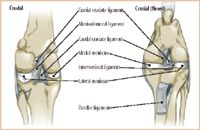
Figure 1 The ligaments and menisci of the canine stifle joint.
The medial collateral ligament passes distally from the medial femoral epicondyle, sharing a firm attachment to the abaxial margin of the medial meniscus, to insert along a rectangular footprint on the medial aspect of the tibia. Portions of the medial collateral ligament remain taut throughout a full range of extension and flexion. The lateral collateral ligament originates on the lateral femoral epicondyle and passes distally before inserting primarily on the fibular head. The lateral collateral ligament is taut in extension, but its laxity during flexion permits a physiologic internal rotation of the stifle joint. Conversely, during stifle extension, the lateral collateral ligament draws taut and causes external rotation of the tibial plateau with respect to the femur in what is called the screw-home mechanism.4
The medial and lateral menisci are semilunar fibrocartilage structures positioned between the articular surfaces of the femoral and tibial condyles (Figure 2). The menisci have several important functions, including energy absorption and stress transfer across the femorotibial joint, joint stabilization, prevention of synovial membrane impingement between the femur and tibia, and joint proprioception.5 The menisci stabilize the joint by functionally deepening the articular surface of the tibial plateau—much like a chock behind a tire. In cross section, the menisci are wedge-shaped, and the peripheral circumference is thick and white while the axial margins are thin and almost translucent. The femoral surface of each meniscus is concave to receive the curved surface of the femoral condyle. The tibial surface is relatively flat. Cranial and caudal tibial ligaments of the medial and lateral menisci anchor each meniscus to the tibial plateau. The cranial meniscal horns are united by the intermeniscal, or transverse, ligament (Figure 2). This ligament is an important landmark because it borders the cranial margin of the tibial insertion of the cranial cruciate ligament.
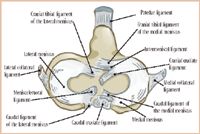
Figure 2 The medial and lateral menisci; dorsal view. Note the caudal margin of the lateral meniscus is attached to the femur by way of the meniscofemoral ligament.
The periphery of each meniscus is attached to the joint capsule. The attachment of the lateral meniscus differs from that of the medial meniscus in three distinct ways: 1) the caudal margin of the lateral meniscus is less firmly attached to the joint capsule; 2) the lateral meniscus is not attached to the lateral collateral ligament, but the medial meniscus is attached to the medial collateral ligament; and 3) the caudal margin of the lateral meniscus is also attached to the femur with the meniscofemoral ligament. Only the peripheral 10% to 25% of each meniscus is supplied by a vascular network and innervated. The axial majority of the menisci is avascular and aneural and is nourished by diffusion of synovial fluid.
The femoral condyle is shaped similar to a rounded-off L that produces motion like a cam would as the stifle is fully extended.6 This shape varies among breeds; for example, a Welsh corgi has a considerably different distal femoral conformation than a Shetland sheepdog has. The proximal tibia consists of an articular plateau and a tibial tubercle. The tibial plateau has a natural caudal and distal slope that also varies.6
BIOMECHANICS
During weightbearing in the hindlimbs, ground reaction forces are resisted by contracting the extensor, or antigravity, muscles (quadriceps and gastrocnemius muscles). These combined forces across the stifle compress the femur against the caudal- and distal-sloped proximal tibial plateau. The slope of the tibial plateau converts this femorotibial compression into a cranially directed shear force called cranial tibial thrust.6 This shear force does not normally induce cranial tibial translation in healthy canine stifles because it is constrained by the intact cranial cruciate ligament with probable contribution by the pull of the hamstring muscles on the proximal tibia. The magnitude of the cranial tibial thrust is a function of external ground reaction forces, internal muscular forces, and the slope of the tibial plateau. When cranial tibial thrust exceeds the tensile strength of a healthy cranial cruciate ligament or a weakened, degenerative cranial cruciate ligament, the ligament completely or partially ruptures.
PATHOPHYSIOLOGY
Rupturing or stretching the cranial cruciate ligament permits cranial tibial translation (classically evaluated with the cranial drawer test) and excessive internal rotation.3 The pathogenesis of cranial cruciate ligament tearing is typically the result of a complex interplay of pathologic processes. Essentially, a healthy cranial cruciate ligament ruptures if the ligament's breaking strength is exceeded, usually in association with traumatic or athletic injury. Because the cranial cruciate ligament is the primary constraint against stifle extension and internal rotation, events causing excessive internal rotation and hyperextension are probable mechanisms for pure traumatic rupture.7 However, such cases represent a minority of patients with cranial cruciate ligament pathology. More commonly, cranial cruciate ligament pathology is related to degenerative changes within the ligament that occur with age and disuse.8,9
During aging, a dog loses fibroblasts, converts surviving fibroblasts into chondrocytes, and loses collagenous matrix within the cranial cruciate ligament.8 These aging changes develop at younger ages in larger breeds compared with smaller breeds. Ruptured cranial cruciate ligaments harvested from medium- and large-breed dogs within 24 hours of the acute onset of lameness showed degenerative changes and unsuccessful attempts at repair.8 These changes predispose the cranial cruciate ligament to tearing, and this mechanism is called cranial cruciate disease.10 Such pathophysiologic understanding explains the relatively high frequency of dogs with unilateral cranial cruciate ligament pathology that eventually develop similar changes in the contralateral stifle. Immune-mediated and septic arthritis of the stifle may also predispose the cranial cruciate ligament to rupture.
It is commonly theorized that abnormal biomechanics associated with medial patellar luxation, malaligned skeletal conformations, or both predispose a dog to cranial cruciate ligament rupture. While scientific evidence for a causal relationship is lacking, clinical observations suggest the conditions may be associated. When patellar luxation and cranial cruciate ligament rupture coexist, surgical correction of each problem is typically indicated. Regardless of the underlying mechanism of the cranial cruciate ligament pathology, unchecked instability induces synovitis, cartilage degeneration, periarticular osteophytosis, and meniscal injury. Interestingly, in an experimental setting, when the stifle was stabilized immediately after cranial cruciate ligament excision, no gross or radiographic evidence of degenerative joint disease was noted.11 This observation suggests that early diagnosis and treatment may benefit patients.
SIGNALMENT
Dogs of any breed, sex, or age can present for lameness resulting from cranial cruciate ligament pathology; however, a breed predisposition has been reported in Labrador retrievers, Chesapeake Bay retrievers, rottweilers, mastiffs, American Staffordshire terriers, Neopolitan mastiffs, Akitas, and Saint Bernards.12,13 Neutered males and spayed females are at increased risk compared with their intact counterparts.10,12,13 Larger breeds and obese dogs have an increased risk of cranial cruciate ligament disease.10 Cranial cruciate ligament rupture can occur at any age, but larger breeds tend to present at younger ages than do smaller breeds.13
HISTORY
The presenting history of patients with cranial cruciate ligament pathology is varied. The onset varies from peracute after a traumatic or athletic injury to slow and insidious, typical of cranial cruciate ligament disease. Dogs with an acute onset of nonweightbearing lameness often improve over several weeks as the inflammation subsides, particularly with rest and nonsteroidal anti-inflammatory drugs (NSAIDs). But point out to pet owners that this initial improvement does not indicate a resolution of the condition. Commonly, dogs with early or minor cranial cruciate ligament pathology will initially return to near normal function with time, rest, and NSAIDs only to present several weeks or months later with a more severe and persistent lameness. In many cases, this history indicates progression to a complete cranial cruciate ligament rupture or the development of a secondary meniscal injury.
GAIT EVALUATION
Gait evaluation is used to detect lameness and confirm the limbs involved. In some instances, it can strongly direct you toward a specific joint as the source of the lameness. Closely observing dogs standing still, walking, trotting, running, and sitting and rising gives you a great deal of information regarding cranial cruciate ligament function and whether a problem is unilateral or bilateral. Have a trained assistant lead the patient through the gait evaluation so you can see the appropriate gaits.
Dogs with even subtle lameness often lean away from the affected limb while standing. The degree of lameness noted at a walk varies from no lameness to nonweightbearing. Often, lameness that is absent at a walk is evident when the dog is trotting or running. Additionally, circling the dog around you may expose a subtle lameness because weightbearing is shifted toward the inside leg. For example, subtle left pelvic limb lameness may be exposed when circling the patient around you counterclockwise.
Perform a sit test by having the patient sit and rise while facing away from you.14 Dogs with stifle or tarsal pathology will often abduct the affected limb while sitting to avoid the discomfort of the full tarsal and stifle flexion necessary for normal sitting. Alternatively, some dogs will shift the affected limb slightly cranially to diminish flexion of these joints. While you still must perform a complete orthopedic examination, this finding directs you toward stifle or tarsal pathology as one source of the pelvic limb lameness. Dogs presented for bilateral pelvic limb lameness often shift their weight to the thoracic limbs while sitting and rising. In fact, many dogs originally presented for unilateral pelvic limb lameness will shift their weight similarly, which should make you highly suspicious of bilateral pelvic limb involvement.

Figure 3 Palpate both stifles simultaneously to compare muscle mass and determine whether periarticular fibrosis, joint effusion, and warmth are present.
STANDING EXAMINATION
The purpose of the standing examination is to begin to localize the source of the lameness by detecting muscle mass asymmetry, joint swelling, tissue warmth, decreased joint range of motion, and joint instability. Stand behind the dog and encourage it to assume a symmetric stance while you simultaneously palpate each limb to compare muscle mass and determine whether periarticular fibrosis, stifle and tarsal joint effusion, and warmth are present (Figure 3). Closing your eyes may help you focus all sensory input to your fingers. Specifically note the presence or absence of fibrosis and swelling at the medial aspect of the stifle, often called a medial buttress. A normal stifle does not have a palpable medial buttress. A normal stifle has a discretely palpable patellar ligament that feels similar to a pencil with small indentations on each side that have a consistency similar to a bruise on an apple. Palpable loss of the indentations and discrete patellar ligament indicates joint effusion, periarticular fibrosis, or both. If the cranial cruciate ligament is completely ruptured, you may also note a cranial shift of the tibia. Finally, evaluate the patient for a pain response to full stifle extension by placing one hand around the cranial surface of the distal thigh while pushing the other hand forward on the distal tibia or foot (Figure 4). Compare the dog's response to full stifle extension with a similar maneuver performed on the contralateral stifle.

Figure 4 Assess the dog's response to full stifle extension, and compare it to full extension of the contralateral stifle.
Some dogs are more relaxed in the standing position than when restrained in lateral recumbency. For this reason, I prefer to perform a tibial compression test to evaluate for cranial tibial thrust instability at the conclusion of my standing examination (Figures 5A & 5B).15 With practice, the tibial compression test is a reliable method to test for gross stifle instability, especially in larger breeds in which the cranial drawer test is difficult because of muscular strength or sheer size.
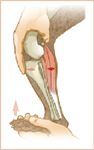
Figure 5A To perform the tibial compression test on the left stifle, place your right index finger on the tibial tuberosity, and squeeze toward the right thumb, which is secured behind the lateral fabella. This maneuver shifts the tibia of the cranial cruciate ligament-deficient stifle caudally into its normal anatomic position under the femur. With your right hand, hold the stifle in a standing angle (neither fully flexed nor fully extended) while you flex the hock with your left hand to simulate weightbearing. This maneuver tenses the gastrocnemius muscle, creating cranial tibial thrust force. In a cranial cruciate ligament-deficient stifle this cranially directed shear force palpably shifts the tibia cranial relative to the femur.
RECUMBENT EXAMINATION
The purpose of the recumbent examination is to continue localizing lameness by detecting a pain response, joint swelling, a limited range of motion, or joint instability. Some form of sedation may be needed in anxious or tense dogs, but heavy sedation may abolish responses to painful stimuli.

Figure 5B A dog undergoing a tibial compression test.
Examine the unaffected pelvic limb first to establish a baseline, and palpate from the digits toward the pelvis. Examine the upper-most limb of the laterally recumbent patient. Evaluate patellar stability, and perform tibial compression and cranial drawer tests, all stifle-specific procedures. For example, imagine you are evaluating the left pelvic limb of a dog in right lateral recumbency. Position yourself behind your patient's pelvic limbs. To test lateral patellar stability of the left stifle, apply firm lateral pressure on the patella with your right hand while holding the extended stifle in external rotation with your left hand, and then slowly flex the stifle. Conversely, to test medial patellar stability, apply firm medial pressure on the patella with your right hand while holding the extended stifle in internal rotation with your left hand, and then slowly flex the stifle. Luxation is detected as a popping or snapping sensation of the patella. Bony crepitus and an indistinct transition between luxation and reduction may indicate a loss of articular cartilage and subchondral bone suggestive of chronicity. Perform the tibial compression test as described previously.
To test for cranial tibial translation, perform the cranial drawer test (Figure 6). In a mature dog, a healthy, intact cranial cruciate ligament will not permit cranial tibial translation with the stifle held in extension or in flexion.3 In an immature dog, puppy laxity may permit a few millimeters of cranial and caudal tibial translation, but the endpoints are crisp and distinct (similar to reaching the end of a taut rope). In a dog with complete cranial cruciate ligament rupture, cranial tibial translation is obvious and an indistinct, ill-defined endpoint exists.
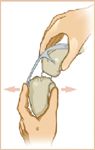
Figure 6 To perform the cranial drawer test on the left stifle of a patient in right lateral recumbency, place your right index finger firmly on the patella and right thumb behind the lateral fabella to secure the distal femur. Place your left index finger on the tibial crest and left thumb behind the fibular head to secure the proximal tibia. Slowly rolling tissues away from the fibular head with your thumb and using a gentle grip will prevent patient discomfort associated with squeezing the peroneal nerve against the fibular head (a painful response from the patient is most often associated with the examiner's grip on the limb and does not indicate cranial cruciate ligament pathology). While holding the femur in place with your right hand, apply a firm cranially directed force to the tibia with your left hand.
Next, apply a firm caudally directed translational force to the tibia while holding the distal femur stable. Caudal cruciate ligament integrity is confirmed by a distinct endpoint to caudal tibial translation. Perform the drawer test with the stifle in extension, flexion, and a standing angle. Partial tears of the cranial cruciate ligament often produce cranial drawer instability only when the stifle is flexed. Such a finding implies tearing primarily in the craniomedial band of the cranial cruciate ligament because the remaining caudolateral band relaxes in flexion and permits drawer movement.
It is important to realize that periarticular fibrosis or early-stage cranial cruciate ligament pathology may prevent the detection of palpable instability. Thus, the absence of palpable instability does not necessarily preclude the clinical diagnosis of cranial cruciate ligament pathology or its surgical treatment.
During the recumbent and standing examinations, remain alert for the clicks typical of meniscal injury. Gross injury to the medial meniscus is common in conjunction with cranial cruciate ligament pathology, especially in large-breed dogs with chronic cranial cruciate ligament pathology or gross stifle instability.5,16
RADIOGRAPHY
Caudocranial and mediolateral radiographs are used to stage any associated osteoarthritis, lend support to a cranial cruciate ligament pathology diagnosis, and screen for complicating or coincident pathology, such as osteochondrosis or neoplasia. The cranial cruciate ligament cannot be visualized radiographically—a fact worth pointing out when discussing radiographic findings with pet owners. With many dogs, sedation is required for high-quality radiographs. Joint effusion, osteophytosis, or cranial tibial displacement lends support to a diagnosis of cranial cruciate ligament rupture. The findings vary depending on the chronicity of the disease.
On the mediolateral view, joint effusion is seen as a gray halo surrounding the distal femur that compresses a radiolucent infrapatellar fat pad within the cranial joint space and distends the caudal joint capsule to varying degrees (Figure 7). Osteophytes along the margins of the medial and lateral femoral trochlear ridges and the distal pole of the patella are seen with chronic disease. Cranial tibial displacement can be seen in selected instances of acute, complete cranial cruciate ligament rupture and is more commonly noted in small-breed dogs.
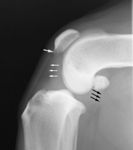
Figure 7 A mediolateral radiograph of the stifle of a dog with cranial cruciate ligament pathology. Joint effusion is the gray halo surrounding the distal femur that compresses the infrapatellar fat pad (white arrows) within the cranial joint space and distends the caudal joint capsule (black arrows). An osteophyte is present on the distal pole of the patella (single gray arrow). In more chronic cases, osteophytes may be seen along the margins of the medial and lateral femoral trochlear ridges.
SYNOVIAL FLUID ANALYSIS
Synovial fluid analysis can be helpful in assessing the more subtle presentations of lameness. Synovial fluid analysis helps distinguish acute from chronic cranial cruciate ligament pathology and detect septic or immune-mediated joint disease. Diagnosing septic or immune-mediated joint disease greatly affects the treatment and possibly the prognosis.
Technique
Follow strict aseptic technique, and prepare a small sample site by clipping the coat and scrubbing the space medial or lateral to the patellar ligament with an antiseptic. Analgesia and sedation are indicated and facilitate patient restraint. Wear sterile gloves, and advance a sterile 20- or 22-ga 1- to 1-½-in needle and 3-ml syringe toward the center of the stifle from a point immediately medial or lateral to the ligament. Apply gentle suction to the syringe. Ideally, you should retrieve 1 ml or more of synovial fluid from the joint. Considerably larger volumes can be removed and may provide some temporary pain relief in patients with marked joint effusion.
Divide aliquots of aspirated joint fluid among an EDTA-tube, a red-top clot tube, and two slides (to make air-dried smears). Synovial fluid analysis performed by most commercial laboratories includes evaluating the fluid color, volume, and viscosity and performing a mucin clot test, cell counts, and cytology. If septic arthritis is suspected, an aliquot of joint fluid can be placed in blood culture medium as an enrichment broth for subsequent bacterial culture and sensitivity testing.
Findings
Normal joint
Normal joint fluid is clear and colorless to straw-colored with high viscosity and a good mucin clot test result. Obtaining sample volumes in excess of 1 ml may not be possible in some normal joints. The nucleated cell count should range from 0 to 2,900/mm3 with 88% to 100% monocytes and 0% to 12% neutrophils.17
Acute cranial cruciate ligament rupture
Acute cranial cruciate ligament rupture associated with trauma or high-energy athletic activity may cause hemarthrosis. The joint fluid is typically turbid and homogeneously bloody with decreased viscosity and a fair to poor mucin clot test result. The number of nucleated cells and the differential counts are highly variable. The presence of hemosiderin-laden macrophages and erythrophagocytosis suggests the blood is not from iatrogenic contamination.
Septic arthritis
Joint sepsis can contribute to a great deal of joint pathology, including cranial cruciate ligament rupture. The aspirated joint fluid is turbid and may appear grossly purulent but more often is red- or gray-tinged. The joint fluid viscosity is reduced, and the mucin clot test result is poor to very poor. Nucleated cell counts typically range from 110,000 to more than 267,000 cells/mm3 with 90% to 99% neutrophils and 1% to 10% monocytes. Bacteria may be seen intracellularly or extracellularly. Joint fluid culture is warranted whenever the nucleated cell count is elevated and is predominantly neutrophilic because bacteria are not seen microscopically in many cases of septic arthritis.
Immune-mediated joint disease
Immune-mediated joint disease may also contribute to enzymatic degradation of the cranial cruciate ligament. The joint fluid is typically turbid and may be yellow-tinged or bloody. The fluid viscosity is usually reduced, and the mucin clot test result may be good to poor. The nucleated cell count can range from 3,000 to more than 350,000 cells/mm3. The differential count may vary from predominantly neutrophils to predominantly monocytes.
Degenerative joint disease
Most commonly, findings of the the synovial fluid analysis will be typical of degenerative joint disease. Such fluid is clear and colorless to yellow-tinged. The viscosity is normal to decreased, and the mucin clot test result is good to fair. The nucleated cell count ranges from 0 to 3,500 cells/mm3 with 88% to 100% monocytes and 0% to 12% neutrophils. Cartilage cells and synoviocytes may also be noted.
FINAL DIAGNOSIS OR FURTHER TESTS
Diagnosing cranial cruciate ligament pathology is easy when a supportive history, signalment, gait evaluation, and radiographic appearance are combined with positive results on tibial compression or cranial drawer tests. However, some dogs with cranial cruciate ligament pathology do not have palpable stifle instability. In these dogs, a compatible history and lameness evaluation in conjunction with a palpable medial buttress, pain on full stifle extension, radiographic joint effusion, and synovial fluid indicative of degenerative joint disease support a diagnosis of cranial cruciate ligament pathology even in the absence of palpable stifle instability.
If you suspect a dog has cranial cruciate ligament pathology but the diagnostic findings do not warrant exploratory arthrotomy, consider magnetic resonance imaging (MRI) or arthroscopic evaluation vs. a conservative watchful-waiting approach. With a conservative approach, the dog is reevaluated in four to eight weeks or at the first sign of symptomatic progression, whichever is sooner.
MRI
Unlike radiography, MRI allows visualization of the cruciate ligaments and menisci, so it may be used to detect more subtle pathology.18,19 However, because MRI accessibility is limited, it has not been an integral part of the diagnosis for most patients with cranial cruciate ligament pathology.
Arthroscopy
Arthroscopic assessment and treatment of the intra-articular structures of the stifle are performed at many specialty practices. The illumination and magnification allow direct visualization of the cranial cruciate ligament and surrounding structures.20 Arthroscopic techniques for cranial cruciate ligament and medial meniscal tear débridement, medial meniscal release, and meniscectomy have been developed.
TREATMENT
Surgically stabilizing the stifle is indicated in most patients with cranial cruciate ligament pathology. Combinations of small patient size, adequate locomotor function and comfort, the presence of concurrent disease, and advanced age may preclude surgical stabilization in isolated instances. Traditionally, surgical treatments have sought to passively constrain the stifle joint by substituting the cranial cruciate ligament with autologous tissues or synthetic materials. These techniques have been exhaustively described elsewhere. More recently, the tibial plateau leveling osteotomy (TPLO) and tibial tuberosity advancement procedures have been described, which render the cranial cruciate ligament unnecessary by altering the mechanical forces acting on the stifle. The TPLO procedure is described in the next article.
Ross H. Palmer, DVM, MS, DACVS
Department of Clinical Sciences
College of Veterinary Medicine and Biomedical Science
Colorado State University
Fort Collins, CO 80523
REFERENCES
1. Vasseur PB. Stifle joint. In: Slatter D, ed. Textbook of small animal surgery. 2nd ed. Philadelphia, Pa: WB Saunders, 1993;1817-1865.
2. Evans HE, Christensen GC. Joints and ligaments of the pelvic limb. In: Evans HE, Christensen GC, eds. Miller's anatomy of the dog. 2nd ed. Philadelphia, Pa: WB Saunders, 1979;254-268.
3. Arnoczky SP, Marshall JL. The cruciate ligaments of the canine stifle: an anatomical and functional analysis. Am J Vet Res 1977;38:1807-1814.
4. Vasseur PB, Arnoczky SP. Collateral ligaments of the canine stifle joint: anatomic and functional analysis. Am J Vet Res 1981;42:1133-1137.
5. Briggs KK. The canine meniscus: injury and treatment. Compend Contin Educ Pract Vet 2004;26:687-697.
6. Slocum B, Slocum TD. Tibial plateau leveling osteotomy for repair of cranial cruciate ligament rupture in the canine. Vet Clin North Am Small Anim Pract 1993;23:777-795.
7. Arnoczky SP. Surgery of the stifle—the cruciate ligaments (part I). Compend Contin Educ Pract Vet 1980;2:106-115.
8. Vasseur PB, Pool RR, Arnoczky SP, et al. Correlative biomechanical and histologic study of the cranial cruciate ligament in dogs. Am J Vet Res 1985;46:1842-1854.
9. Paatsama S. Ligament injuries in the canine stifle joint. J Small Anim Med 1953;1:329-334.
10. Lampman TJ, Lund EM, Lipowitz AJ. Cranial cruciate disease: current status of diagnosis, surgery and risk for disease. Vet Comp Orthop Traumatol 2003;16:122-126.
11. Smith GK, Torg JS. Fibular head transposition for repair of cruciate-deficient stifle in the dog. J Am Vet Med Assoc 1985;187:375-383.
12. Duval JM, Budsberg SC, Flo GL, et al. Breed, sex, and body weight as risk factors for rupture of the cranial cruciate ligament in young dogs. J Am Vet Med Assoc 1999;215:811-814.
13. Whitehair JG, Vasseur PB, Willits NH. Epidemiology of cranial cruciate ligament rupture in dogs. J Am Vet Med Assoc 1993;203:1016-1019.
14. Slocum B, Slocum TD. Knee. In: Bojrab MJ, Ellison GW, Slocum B, eds. Current techniques in small animal surgery. 4th ed. Baltimore, Md: Williams & Wilkins, 1998;1187.
15. Henderson RA, Milton JL. The tibial compression mechanism: a diagnostic aid in stifle injuries. J Am Anim Hosp Assoc 1978;14:474-479.
16. Flo GL. Meniscal injuries. Vet Clin North AmSmall Anim Pract 1993;23:831-843.
17. Fernandez FR, Grinden CB, Lipowitz AJ. Synovial fluid analysis: preparation of smears for cytologic examination of canine synovial fluid. J Am Anim Hosp Assoc 1983;19:727.
18. Gonzalo-Orden JM, Altonaga JR, Gonzalo-Cordero JM, et al. Magnetic resonance imaging in 50 dogs with stifle lameness. Euro J Comp Anim Pract 2001;11:115-118.
19. Banfield CM, Morrsion WB. Magnetic resonance arthrography of the canine stifle joint: technique and applications in eleven military dogs. Vet Radiol Ultrasound 2000;41:200-213.
20. Whitney WO. Arthroscopically assisted surgery of the stifle joint. In: Beale B, Hulse D, Schulz K, et al., eds. Small animal arthroscopy. Philadelphia, Pa: WB Saunders, 2003;116-157.
Newsletter
From exam room tips to practice management insights, get trusted veterinary news delivered straight to your inbox—subscribe to dvm360.