
Platelets are essential for normal hemostasis and serve three main functions. They maintain vascular integrity by forming platelet plugs and promoting endothelial vasoconstriction in areas of disrupted endothelium.

Platelets are essential for normal hemostasis and serve three main functions. They maintain vascular integrity by forming platelet plugs and promoting endothelial vasoconstriction in areas of disrupted endothelium.
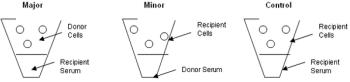
Common transfusion types include fresh whole blood, stored whole blood, packed red blood cells, fresh frozen plasma, and frozen plasma. Other, less common transfusion products include cryoprecipitate, cryo-poor plasma, platelet-rich plasma, platelet concentrate, lyophilized albumin, and lyophilized platelets.

The patient with multi-trauma can present a challenging case for a clinician.Damage to the respiratory system, cardiovascular system, or neurologic system can all be fatal by themselves, and a combination of these injuries can present as a resuscitation nightmare.

The primary hemostatic system alone is not sufficient to provide hemostasis if a large vessel is injured, or if there is significant vascular wall injury. Fibrin needs to be generated in order to form a stable clot, and this occurs through secondary hemostasis, or the coagulation cascade.

Patients presenting with severe respiratory distress have minimal respiratory reserves, so stress during physical evaluation and treatment must be minimized. Quick evaluation of the patient with minimal additional stress (i.e. radiographs, blood draws) is ideal so that accurate therapy can be instituted without delay.

Cardiopulmonary arrest (CPA) is defined as the cessation of functional ventilation and effective circulation. Factors predisposing to CPA may include respiratory or cardiovascular abnormalities (hypoxia, hypercarbia, hypotension, cardiac arrhythmias, or severe anemia); acid-base, electrolyte, or metabolic abnormalities (acidosis, hyperkalemia, hypoglycemia); or hypothermia.

Adequate nutrition is essential for the critically ill patient. Nutrients are necessary to provide substrates for normal cellular functions, protein synthesis, and daily metabolic processes. The critical patient is often in a hypercatabolic state, so early nutrition is essential to prevent glycogen depletion, immune dysfunction, and loss of body mass, and to provide substrates for wound healing.

August 1st 2010
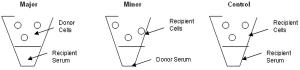
August 1st 2010

August 1st 2010

August 1st 2010

August 1st 2010