Toxicology Brief: Mushroom poisoning in dogs
Mushroom poisoning of companion animals, particularly dogs, is a potentially underestimated problem in North America.
Mushroom poisoning of companion animals, particularly dogs, is a potentially underestimated problem in North America. Because of their wandering and scavenging nature, dogs seem particularly prone to mushroom poisoning.1-8 While there have been sporadic reports of mushroom poisoning in dogs in the veterinary literature,1-8 anecdotal experience in the Pacific Northwest suggests it is more prevalent than the literature indicates.
This article summarizes the clinical effects of the toxicologically important mushrooms in North America. Spring, summer, and fall are the principal seasons for mushroom poisoning in most of North America.9
IDENTIFICATION AND TREATMENT
Toxic mushrooms are divisible into eight groups based on their toxin type (Table 1).9 Six of these groups are of potential veterinary significance, and representative members of these groups are common throughout North America.9 In line with the adage, "There are old mushroom hunters, there are bold mushroom hunters, but there are no old, bold mushroom hunters," all wild-growing mushrooms should be regarded as toxic until proven otherwise.
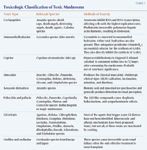
Table 1. Toxicologic Classification of Toxic Mushrooms
Ideally, samples of the ingested mushrooms should be brought in to the clinic along with the affected animal. Do not place mushrooms for identification in a plastic bag; instead, wrap them in a moist paper towel or wax paper or place them in a paper bag. Identifying mushroom species is often complex, so consult a human poison information center with experience in mushroom identification (e.g. the Oregon Poison Center [(800) 222-1222]) or a mycologist as needed.9,10
Cyclopeptides
Amanita, Galerina, and Lepiota species mushrooms contain toxic cyclopeptides. Amanita species are the most commonly documented cause of fatal mushroom poisoning in dogs,1,2,4-8 and they account for 95% of mushroom-related fatalities in people.9 Amanita phalloides, the death cap mushroom (Figure 1), accounts for more than 50% of all mushroom-associated deaths in people and most of the reported fatal cases in dogs.1,2,6,9

Amanita phalloides, the death cap mushroom, is the most common cause of potentially fatal mushroom poisoning in people and dogs.
The toxic cyclopeptides in these mushrooms are amatoxins, phallotoxins, and virotoxins.8,9 These peptides are rapidly absorbed from the gut, and their duration of action is increased by enterohepatic circulation and active resorption of amatoxins from the renal glomerular filtrate. Amatoxins and phallotoxins are responsible for most of the pathologic effects.9 Amatoxins interfere with DNA and RNA transcription and, thus, selectively affect the rapidly replicating cells of the gastrointestinal (GI) and renal tubular epithelium and liver. Phallotoxins irreversibly polymerize hepatic actin filaments, triggering hepatic cholestasis.9
Typically, 10 to 12 hours pass between consumption and the onset of clinical signs.9 This delay is an important differential diagnostic feature of cyclopeptide ingestion and is probably due to the time required for amatoxins to bind to intranuclear RNA polymerase II.9
There are three distinct sequential phases of cyclopeptide poisoning. The initial gastroenteritis phase is characterized by profuse bloody diarrhea, vomiting, nausea, abdominal pain, dehydration, electrolyte imbalance, fever, tachycardia, and hyperglycemia.9 This phase typically lasts about 24 hours. The resolution of clinical signs and subclinical elevations of serum alanine transaminase and aspartate transaminase activities characterize the onset of the 12- to 24-hour latent phase.9 The final—and often terminal—hepatorenal phase of poisoning begins three to four days after ingestion.9 Severe hepatic dysfunction, severe renal failure, cerebral edema, icterus, elevated serum hepatic enzyme activities, hypoglycemia, coagulopathies and hemorrhage, azotemia, metabolic acidosis, and sepsis characterize the hepatorenal phase. In addition, neurologic dysfunction including hepatic encephalopathy and coma can occur.9 Typically, the animal dies three to seven days after ingestion.9
Treatment. Early aggressive decontamination and enhanced elimination are critical.6,8,9 Performing emergency upper GI decontamination (inducing emesis or gastric lavage) is probably not beneficial more than four hours after ingestion since phallotoxins and amatoxins are rapidly absorbed from the GI tract and do not form gastric concretions or delay gastric emptying.9 Induce emesis only in asymptomatic animals because of the risks associated with this procedure.
The effectiveness of activated charcoal is unknown, but its use has been recommended.9 Administer an activated charcoal slurry (1 g/5 ml water) orally at a dose of 2 to 5 ml/kg in combination with a mild cathartic (sorbitol 3 mg/kg orally).11 Repeated doses of activated charcoal may be administered every four to six hours in an attempt to reduce the enterohepatic circulation of amatoxins and may be of value up to 48 hours after ingestion.9 Adequately hydrate patients treated with multiple doses of activated charcoal to prevent constipation.11 Repeated doses of sorbitol may cause marked hypotension or hypovolemic shock, particularly in patients with underlying cardiovascular problems or in small patients, so monitoring is required if repeated doses of activated charcoal and sorbitol are administered.11
Enhanced elimination using peritoneal dialysis and other methods of extracorporeal elimination has yielded occasional therapeutic successes in people.6,9 Administering parenteral penicillin G benzathine at doses greater than 4,300 U/kg, which displaces amatoxins from plasma protein-binding sites making them more available for renal excretion, has been claimed to improve survival in people.9 However, a recent 20-year retrospective analysis has demonstrated that this treatment, alone or in combination with other agents, has little efficacy.12
Supportive care involves administering intravenous crystalloids, glucose, fresh frozen plasma, GI protectants (e.g. kaolin/pectin 1 to 2 ml/kg orally every six to 12 hours), and broad-spectrum parenteral antibiotics to reduce the risk of sepsis. Oral supplementation or parenteral treatment with vitamin K1 (2.5 to 5 mg/kg daily) and packed red blood cell or whole blood transfusions may be required if bleeding is severe.
Silibinin dihydrogen disuccinate disodium and acetylcysteine have been suggested as antidotes for cyclopeptide poisoning.9 Silibinin is a semisynthetic, commercialized, active derivative of silymarin, the hepatoprotectant and antioxidant mixture of medicinal flavonolignans derived from milk thistle (Silybum marianum). Administering silibinin intravenously (20 to 50 mg/kg/day in four doses) substantially increases the survival rate in people.9 Unfortunately, the injectable form of this antidote is not available in the United States, and the poor water solubility and bioavailability of silymarin may limit the effectiveness of this potential antidote when orally administered. Silipide, a complex of silymarin and phosphatidylcholine (lecithin), is about 10 times more bioavailable than silymarin, but its effectiveness as an oral antidote for A. phalloides mushroom poisoning has not been investigated. The effectiveness of acetylcysteine for treating mushroom cyclopeptide poisoning is questionable. However, given its low risk of adverse effects, treatment can be attempted by administering a loading dose of 140 mg/kg orally followed by 70 mg/kg orally every six hours for as long as the patient needs it based on clinical judgment.
Monomethylhydrazine
Gyromitra species of mushrooms, often called false morels, vary considerably in their toxicity from year to year and location to location. Of the several different toxic hydrazine compounds found in these mushrooms, gyromitrin is the best known.9
The hydrolysis of gyromitrin in the gut results in the formation of monomethylhydrazine, a GI irritant, and subsequent gastroenteritis within six to eight hours of ingestion. Most cases are relatively mild and self-limiting; however, extreme poisonings characterized by hepatic damage have been reported in people.9 Monomethylhydrazine also directly inhibits the synthesis of gamma-aminobutyric acid (GABA) within the central nervous system (CNS) and antagonizes pyridoxine (vitamin B6), an essential cofactor for the synthesis of GABA. The net result is uncontrolled CNS electrical activity, anxiety, restlessness, excitation, and seizures.9
Treatment. Pyridoxine (25 mg/kg administered as a slow intravenous infusion over 15 to 30 minutes) has been recommended as an antidote for the neurologic effects of this type of mushroom poisoning.9 Additional treatment consists of upper GI decontamination and supportive care. Because of the risk of precipitating seizures, inducing emesis in severe monomethylhydrazine poisoning cases is potentially risky. Inducing emesis with due clinical prudence and judgment may be appropriate for milder cases. Activated charcoal administration has been recommended, although its effectiveness is unknown.9 Rehydration by using intravenous crystalloids is the most commonly required supportive treatment.9 Oral GI protectants may be beneficial. If necessary, anxiety, restlessness, and seizures can be controlled with a benzodiazepine (0.25 to 0.5 mg/kg diazepam intravenously or intramuscularly).9
Coprine
Coprine, the major fungal toxin associated with Coprinus atramentarius mushroom poisoning, inhibits aldehyde dehydrogenase, thus inhibiting the conversion of ethanol (alcohol) to acetate and resulting in an accumulation of acetaldehyde. This effect only occurs if there is an association between the consumption of C. atramentarius mushrooms and ethanol.9 If ethanol is not consumed concurrently with these mushrooms, the poisoning does not occur. Thus, this poisoning is unlikely in veterinary medicine.
Muscarine
Muscarine is a muscarinic receptor agonist that produces postganglionic parasympathomimetic effects, such as increased genitourinary muscle tone, bradycardia, miosis, and salivation.9 The most common mushrooms involved in muscarine poisoning include members of the Inocybe and Clitocybe genera.9 Although Amanita muscaria has been classically associated with muscarine toxicity, it contains insignificant amounts of this toxin.9
Clinical signs usually occur within two hours after ingestion and are characterized by the acronym SLUD (salivation, lacrimation, urination, diarrhea).9 Other common clinical signs include bradycardia, hypotension, shock, dyspnea and wheezing due to bronchoconstriction and increased respiratory secretions, abdominal pain, miosis, visual disturbance, and rhinorrhea.9 An alternative acronym sometimes used to describe the effects of excessive muscarine stimulation is DUMBBELS (diarrhea, urination, miosis, bronchorrhea, bronchoconstriction, emesis, lacrimation, salivation).
Treatment. Performing early upper GI decontamination is useful, although spontaneous vomiting may eliminate the need for this treatment.9 Activated charcoal administration is potentially useful. The specific reversal agent for muscarine poisoning is atropine.9 If clinical signs of excessive muscarine stimulation are present, administer atropine (0.2 to 2 mg/kg; 50% of the dose administered intravenously and 50% intramuscularly or subcutaneously) slowly and progressively to effect using the drying of the oral and respiratory secretions as the clinical endpoints.9 Do not use the correction of miosis to judge the atropine dose since by the time the pupils return to normal, most patients have received too much atropine, resulting in potentially adverse cardiovascular effects.9 Intravenous crystalloids are usually sufficient to control any hypotension that develops.9
Isoxazole derivatives
Amanita muscaria and Amanita pantherina are the principal North American mushroom species associated with poisoning from isoxazole derivatives.9 Given the popular recreational use of these mushrooms by people, it is surprising that poisoning in companion animals is poorly documented.9
Ibotenic acid and muscimol, the principal psychoactive isoxazole derivatives present in these mushrooms, alter visual perception rather than cause true hallucinations in people.9 Ibotenic acid, a CNS glutamate acid receptor agonist, acts as a CNS stimulant; muscimol, a CNS GABAB agonist, acts as a CNS depressant and sedative.9 In people, the primary effects are periods of CNS stimulation and depression that may alternate and may manifest as periods of manic excitement followed by periods of somnolence and deep sleep. Clinical signs typically associated with poisoning in people include dizziness, ataxia, euphoria, muscle twitches, and initial psychic stimulation followed by dream-filled sleep.9
Treatment. Treatment consists of upper GI decontamination and supportive measures, such as observation, confinement in a dark and quiet cage, and possibly sedation. Use all hypnotic drugs with caution because the isoxazole derivatives potentiate their effects.9
Psilocybin and psilocin
Because of its popularity as a recreational drug, this group of mushrooms, know as hallucinogenic or magic mushrooms, occasionally causes poisoning in dogs.3 Important genera involved in poisoning include Psilocybe, Panaeolus, Copelandia, Gymnopilus, Pluteus, and Conocybe.9 The principal toxins in these mushrooms are psilocybin and psilocin, which have LSD-like properties.9 These compounds typically produce a transient (less than 12-hour duration), dysphoric, and sympathomimetic syndrome. Coingestion of other drugs of abuse such as LSD, PCP, and marijuana is common in people and is a potentially important consideration in veterinary patients.9
Common clinical signs, which develop a half an hour to four hours after ingestion, include anxiety, aggression, disorientation, visual hallucinations (e.g. following and biting at imaginary flies, pointless barking), weakness, mydriasis, tachycardia, and hyperreflexia.3,9 Hypertension, hyperthermia, or convulsions may occur, and patients may become comatose in cases of extreme overdose. However, trauma caused by altered behavior is usually the greatest and most immediate threat to life.3,9
Treatment. Emergency GI decontamination in a conscious patient poisoned by these mushrooms may be difficult because of the patient's altered behavior and aggression. An easier option may be gastric lavage after anesthesia and placement of a cuffed endotracheal tube.9 The main potential difficulty associated with anesthesia is the induction because of the dysphoric, and potentially aggressive, mental state of the patient. Prior sedation with a benzodiazepine (0.5 to 1 mg/kg diazepam intravenously or 1 to 4 mg/kg rectally) or an alternative induction technique, such as using an induction chamber, may be required. The use of induction chambers carries with it the increased risks associated with decreased access to the patient, so their use with dysphoric patients requires careful clinical judgment.
Treatment usually consists of supportive care. Since the most immediate concern is preventing accidental trauma, often the most successful supportive care is placing the animal in a quiet, dark, padded cage in the presence of its owner.9 Warn the animal's owners and handlers of the potential for aggressive behavior. If sedation is required, a benzodiazepine (0.5 to 1 mg/kg diazepam intravenously or 1 to 4 mg/kg rectally) can be administered.
GI irritants
Numerous mushroom genera are GI irritants (Table 1).9 For the most part, the toxic principles involved are unknown,9 although idiosyncratic and allergic mechanisms have been proposed. Typically, clinical signs of acute GI upset occur within two hours of ingestion and consist of malaise, weakness, nausea, vomiting, and diarrhea.9 The greatest risk associated with poisoning by these mushrooms is fluid and electrolyte imbalance. Most cases are mild and usually resolve without treatment within 24 hours. If required, supportive care would consist of subcutaneous or intravenous crystalloids. The administration of oral GI protectants could be considered once vomiting has ceased.
Orelline and orellanine
While Cortinarius species exist in North America, no poisoning has been recorded to date.9 European and Japanese species from this genus cause acute, irreversible tubulointerstitial nephritis and acute renal failure.9
PREVENTION
As with most poisonings, the best method of controlling mushroom poisonings is preventing exposure. This means that only those who are knowledgeable about mushroom identification should collect wild-growing mushrooms for consumption. Dogs should be prevented from consuming mushrooms or roaming when they are being exercised. As with most poisonings, prompt upper GI decontamination and supportive care are critical elements of treatment.
"Toxicology Brief" was contributed by Rhian B. Cope, BVSc, BSc (Hon 1), PhD, DABT, Department of Environmental and Molecular Toxicology, College of Agricultural Sciences, Oregon State University, Corvallis, OR 97331. The department editor is Petra Volmer, DVM, MS, DABVT, DABT, College of Veterinary Medicine, University of Illinois, Urbana, IL 61802.
REFERENCES
1. Bernard MA. Mushroom poisoning in a dog. Can Vet J 1979;20:82-83.
2. Cole FM. A puppy death and Amanita phalloides. Aust Vet J 1993;70:271-272.
3. Kirwan AP. 'Magic mushroom' poisoning in a dog. Vet Rec 1990;126:149.
4. Naude TW, Berry WL. Suspected poisoning of puppies by the mushroom Amanita pantherina. J S Afr Vet Assoc 1997;68:154-158.
5. Ridgway RL. Mushroom (Amanita pantherina) poisoning. J Am Vet Med Assoc 1978;172:681-682.
6. Tegzes JH, Puschner B. Amanita mushroom poisoning: efficacy of aggressive treatment of two dogs. Vet Hum Toxicol 2002;44:96-99.
7. Yam P, Helfer S, Watling R. Mushroom poisoning in a dog. Vet Rec 1993;133:24.
8. Spoerkem D. Mushroom exposure. In: Peterson ME, Talcott PA, eds. Small animal toxicology. Philadelphia, Pa: WB Saunders Co, 2001;571-592.
9. Schonwald S, Mushrooms. In: Dart RC, ed. Medical toxicology. 3rd ed. Philadelphia, Pa: Lippincott Williams and Wilkins, 2004;1719-1735.
10. Menser GP. Hallucinogenic and poisonous mushroom: field guide. 2nd ed. Berkeley, Calif: Ronin Publishing Inc, 1997;1-115.
11. Peterson M. Toxicologic decontamination. In: Peterson ME, Talcott PA, eds. Small animal toxicology. Philadelphia, Pa: WB Saunders Co, 2001;85-98.
12. Enjalbert F, Rapior S, Nouguier-Soule J, et al. Treatment of amatoxin poisoning: 20-year retrospective analysis. J Toxicol Clin Toxicol 2002;40:715-757.
Newsletter
From exam room tips to practice management insights, get trusted veterinary news delivered straight to your inbox—subscribe to dvm360.